
Some nights, dry eyes don’t just “feel dry”—they feel like sandpaper blink, sticky corners, and a morning penalty you didn’t agree to.
When the bedroom air runs desert-dry, a fan hits your face, and your lid oil flow is sluggish, your tear film doesn’t stand a chance. Keep guessing with random drops and you can lose weeks—plus sleep—without ever knowing what actually helped.
A 15-minute night routine for dry eyes
Built around humidifiers, warm compresses, and eyelid hygiene, this gives you a repeatable way to lower overnight evaporation, support meibomian gland oil flow, and calm a cranky lid margin (often tied to blepharitis).
A 15-minute night routine can calm dry-eye flareups by reducing overnight tear evaporation and supporting healthier eyelid oil flow: set bedroom humidity to a comfortable range, use a warm (not hot) compress for several minutes, then do gentle lid-margin hygiene to clear debris where oils exit. Keep it clean (humidifier + hands), avoid harsh scrubbing, and keep water away from contact lenses.
Safety / Disclaimer: Educational only—not medical advice. Stop and seek care for severe pain, sudden vision changes, marked light sensitivity, or thick discharge.
Table of Contents
Humidifier night routine: who it’s for (and who should pause)
This is for time-poor people who want results without turning their bathroom into a supply closet. If your eyes feel dry mostly at night and in the morning, you’re exactly the audience this routine was built for.
Good fit signs
- Gritty sensation at night or “sticky” lids in the morning
- Morning crusting, burning, or redness that improves later
- Heavy screen days, indoor heating/AC, or a fan pointed at the bed
- “My eyes are fine at noon, terrible at 10 p.m.” (classic)
Pause (or do it with your clinician)
- Recent eye surgery or an eye injury
- Severe pain, strong light sensitivity, sudden vision changes
- Thick discharge, significant swelling, or fever
- Contact lens pain that feels new or sharp
The promise stays small: the routine aims to improve overnight comfort and morning function. Not “cure dry eye.” Not “replace medical care.” Just a practical nightly reset.
- Set the room to reduce evaporation
- Warm the lids to support oil flow
- Clean the lid margin gently (no scrubbing Olympics)
Apply in 60 seconds: Turn off the fan aimed at your face and see if tomorrow feels different.
A quick personal note: I used to “solve” dry eyes by buying new drops every month. My drawer looked like a tiny pharmacy. What helped more was boring consistency—especially at night.
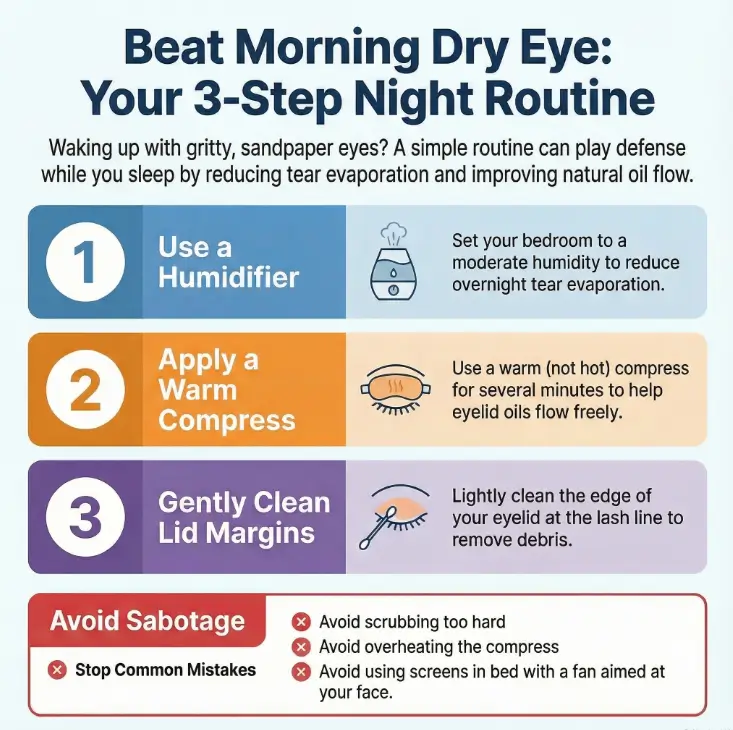
Night dry eye mechanics: why bedtime is the danger zone
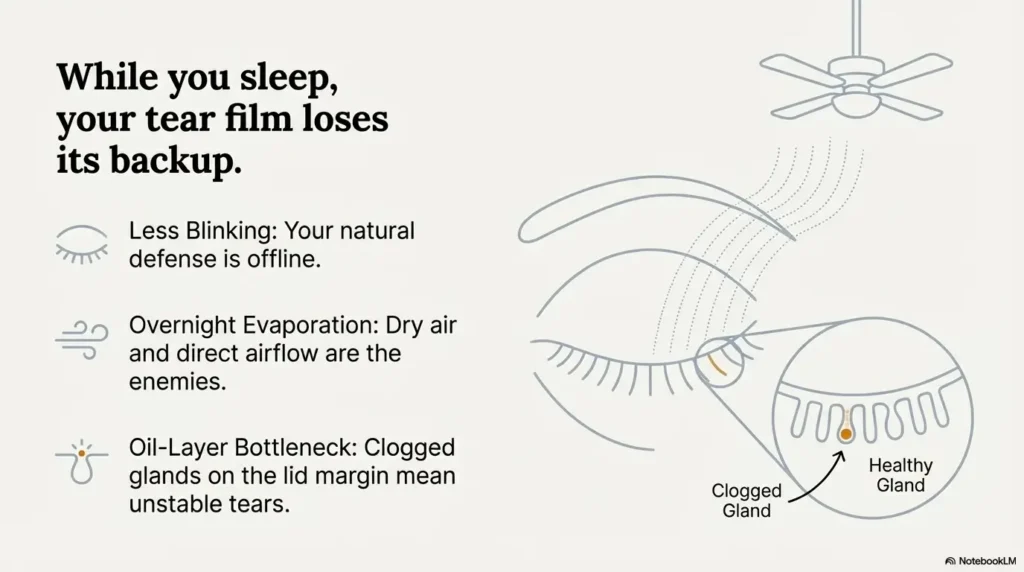
Nighttime dryness isn’t just “you being dramatic.” Sleep is when your tear film loses backup. You blink less (obviously), the air is often drier, and the tiny oil layer that slows evaporation can get… let’s say “moody.”
Overnight evaporation: low humidity + airflow + incomplete lid closure
Two things make eyes feel like they’ve been gently toasted: dry air and moving air. Heating season, AC season, ceiling fans, vents—your eyes don’t care which. If your lids don’t fully seal during sleep (it happens more than people realize), evaporation can spike.
Oil-layer bottleneck: when lids don’t flow, tears don’t last
The eyelids house oil glands that help stabilize tears. When the lid margin is inflamed or clogged, the oil layer can thin out, and tears break up faster. That’s why a “lid routine” can improve a “dry eye” problem.
Open loop: the bedtime habit that quietly cancels your warm compress
There’s one habit that undoes the whole plan. I’ll call it out in the Common mistakes section—because you deserve the truth with the fix attached.
Room air sets the evaporation rate while you sleep.
Warmth supports lid oil flow—if it’s gentle and consistent.
Clean the “oil exit zone” without irritating the skin.
Goal: reduce evaporation + improve oil layer support + lower lid inflammation.
Think of it like this: you don’t need to win the whole day. You need to win the 8 hours when your eyes can’t blink their way out of trouble.
Humidifier setup first: make the room do some work
If you only do one part of this routine, do the room part. It’s low effort, high leverage—like putting a lid on a pot so your soup doesn’t evaporate. (Yes, I just compared your eyes to soup. It’s bedtime. Let me have this.)
Humidity target: comfortable—and not “tropical”
Many indoor air-quality guides emphasize keeping indoor humidity in a moderate band. The U.S. Environmental Protection Agency often discusses keeping humidity from getting too high because it raises mold risk, and it notes that a middle range is typically more comfortable for homes. Translation: you want “less desert,” not “rainforest.”
Placement that helps (and placement that backfires)
- Do: Place the humidifier a few feet from the bed so mist doesn’t blow straight onto your face or pillow.
- Do: Aim for open air circulation—not inside a tight corner where moisture collects.
- Don’t: Point it at the headboard or directly at bedding (hello, damp pillow).
- Don’t: Put it on a delicate wood surface without a tray—humidity has hobbies.
Cleaning cadence: the part that protects your lungs
Humidifiers can be wonderful. They can also become a science experiment if ignored. If you hate cleaning, choose the easiest-to-clean tank. You’re not weak; you’re realistic.
Show me the nerdy details
Humidity is a mold-and-mite variable. Too low can feel drying; too high increases condensation and microbial growth risk. That’s why “moderate” is a safer target than “as high as possible.” A simple hygrometer (often inexpensive at hardware stores) can keep you honest.
- Moderate humidity reduces overnight evaporation
- Bad placement can create damp bedding and irritation
- Cleaning isn’t optional—choose a setup you can maintain
Apply in 60 seconds: Put a small towel/tray under the humidifier tonight to prevent surface moisture.
- Room size: small bedroom vs large open plan (pick capacity accordingly)
- Cleaning reality: daily quick rinse vs weekly deep clean—be honest
- Noise tolerance: if you hate hum, you’ll stop using it
- Water habits: are you willing to refill nightly?
- Placement: can you keep it off the bedline and away from electronics?
Neutral next action: Write down your room size and your “I will actually clean this” schedule before you compare models.
Short Story: The night I learned “dry eye” was also “dry room”
One winter, I did everything “right.” Warm compress. Lid wipes. Drops. And I still woke up feeling like my eyelids had been lightly sanded. I blamed myself—because that’s what we do. Then, on a whim, I moved a cheap hygrometer from the living room to my bedroom. The number was embarrassingly low.
Not tragic, just… dry enough to make evaporation win all night. I ran a humidifier for a few nights and didn’t feel a miracle. I felt something better: a quiet reduction in the morning sting. The kind of improvement that doesn’t make headlines but changes your day. The lesson wasn’t “humidifiers fix everything.” It was “stop fighting the room with your eyeballs.” I kept the routine simple after that, and it finally stuck.
Warm compress done right: heat that helps (not heat that irritates)
Warm compress is the hinge of the whole routine. Not “burn your face” warm. Not “barely lukewarm” warm. Just comfortable warmth for long enough to matter.
Time + rewarming: washcloth vs microwavable mask
- Warm washcloth: cheap and simple, but it cools fast—rewarm it once or twice.
- Microwavable eye mask: often holds heat longer, which can make it easier to stay consistent.
I used to do the washcloth method and quit halfway through because it got cold and I got annoyed. (It’s amazing how quickly bedtime becomes a negotiation.) The mask approach made me more consistent—not because it’s magical, but because it’s less fussy.
Mistake to avoid: “hotter is better”
If the compress is uncomfortably hot, you’ll either irritate the skin or you’ll stop doing the routine entirely. Consistency beats intensity every time.
Let’s be honest… the routine you won’t do won’t work
If you dread it, shrink it. A gentle 5 minutes nightly beats a heroic 15 minutes twice a month.
Show me the nerdy details
Warm compresses are commonly recommended in self-care plans for eyelid inflammation and blocked oil gland function. The mechanism is simple: heat can soften thickened secretions and loosen debris along the lid margin. The practical challenge is maintaining steady warmth long enough to be useful—hence the “choose a tool you can repeat” emphasis.
- Comfortable warmth beats “as hot as possible”
- Pick a tool that stays warm without drama
- Rewarm once if the cloth cools quickly
Apply in 60 seconds: Set a 6-minute timer so you don’t bargain with yourself mid-compress.
Eyelid hygiene focus: clean the lid margin, not the whole eyelid
This is where competitors often go vague: “clean your eyelids.” But the lid margin—the lash-line edge where oils exit—is the point. Clean gently, precisely, and briefly.
Where to clean: lash base / lid edge technique
Wash hands first. Then use your chosen method to lightly clean along the lash line with the eye closed. The goal is to remove debris and reduce irritation at the margin, not to scrub your skin raw.
Cleanser choices: wipes vs foams vs diluted baby shampoo
There isn’t one universal winner—there’s what your skin tolerates. Some people like pre-moistened lid wipes for simplicity. Others prefer a gentle foam cleanser. Some use a very diluted baby shampoo method. If you try something new and it stings or reddens your lids, step back and simplify.
Mistake to avoid: cleaning the lashes but missing the lid margin
It’s easy to “clean” the visible lashes and avoid the edge because it feels tender. That’s like washing the doorknob but ignoring the sticky hinge. The hinge matters.
Here’s what no one tells you… “clean” can still inflame
If you scrub hard, you create irritation, and irritation makes everything feel drier. Gentle wins. Always.
Tap-water rule: keep water away from contact lenses
If you wear contact lenses and rely on daily eye drops, treat “water” like the villain in a small horror movie. The U.S. Centers for Disease Control and Prevention repeatedly warns against exposing contact lenses to water (showering, swimming, rinsing), because water exposure can increase infection risk. That doesn’t mean tap water is evil. It means contacts + water is a risky combo.
Show me the nerdy details
Eyelid cleaning methods range from simple at-home wipes/cleansers to clinician-guided options. The common thread is reducing debris and inflammation at the lid margin. If you’re contact-lens dependent or have recurrent symptoms, it’s worth asking an eye clinician which approach fits your case, because “too harsh” can backfire.
Choose A (wipes/foam) if you want maximum simplicity and consistency.
Choose B (diluted cleanser method) if you’re sensitive to preservatives and prefer controlling dilution.
Stop and reassess if you get worsening redness, burning, or skin irritation after 2–3 nights.
Neutral next action: Try one method for 7 nights before you switch—so you can actually tell what helped.
- Hands clean first
- Short, gentle strokes along the lash line
- Don’t “scrub to prove you tried”
Apply in 60 seconds: If your lids look red after cleaning, reduce pressure by 50% tomorrow.
My most embarrassing dry-eye moment: I once “cleaned my lids” so aggressively I basically exfoliated my confidence. My eyes were not impressed. Gentler was better.
60-second finish: lock in comfort without overdoing products
This is where people accidentally turn a simple routine into a chemistry set. The goal is comfort, not a nightly product audition.
Lubrication timing: drops vs gel/ointment
If you use lubricating drops, many people prefer preservative-free eye drops for frequent use, especially if they’re sensitive. Thicker gels or ointments can last longer overnight but may blur vision—so they’re best right before sleep (and not right before reading one more chapter “for relaxation”).
Makeup rule: don’t sleep in it
Eye makeup can contribute to lid margin irritation for some people—especially when you’re already working on eyelid hygiene. If you can’t commit to removing it, at least commit to not rubbing your eyes afterward. (I’m saying this as someone who has absolutely negotiated with mascara at 11:47 p.m.)
Open loop: the tiny morning clue your lids may not fully close
If you wake with dryness mainly at the center of the eye, or you notice morning blur that clears quickly, it can be a clue (not a diagnosis) that your eyes dry out during sleep. If it’s persistent, that’s a good “ask your clinician” topic—because there are targeted strategies beyond DIY.
Enter your current bedroom humidity (from a hygrometer). This tool gives a conservative comfort hint—not medical advice.
Neutral next action: Don’t chase perfection—pick one target change and test it for 7 nights.
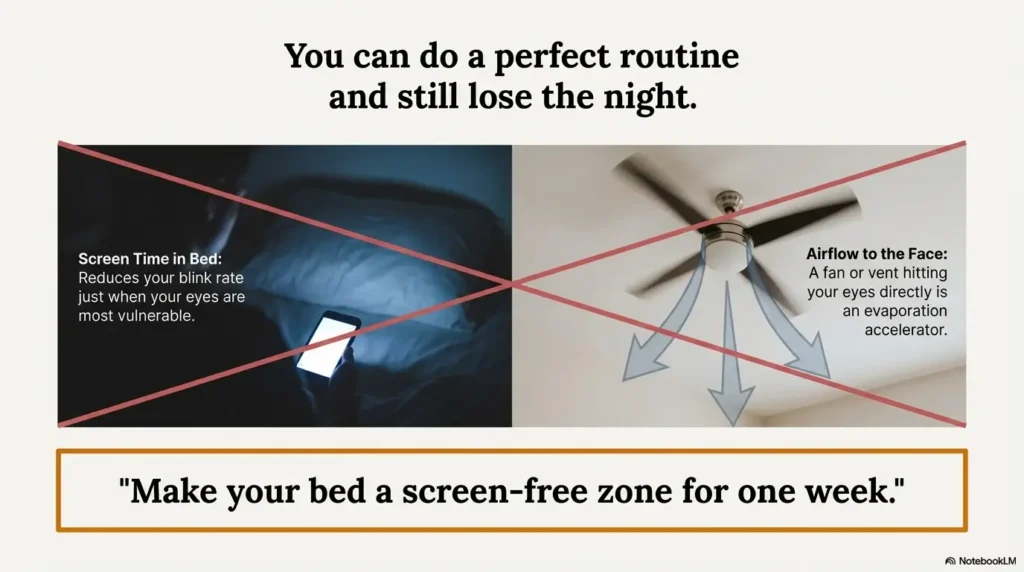
Screen-time + airflow sabotage: the last 2 hours matter more than you think
Here’s the part that feels unfair: you can do a great routine and still lose if the last two hours before bed are a blink-starvation marathon in dry, moving air.
Break + blink patterns (adult version)
Organizations that talk about screen health often emphasize breaks and blinking because staring reduces blink frequency. You don’t need perfection. You need a pattern you can remember—especially if you’re dealing with digital eye strain that shows up as painful, dry eyes.
- Micro-break: Every 30 minutes, look far away for 30 seconds.
- Reset blink: Do 10 slow blinks (not rapid fluttering) and relax the face.
- End-game: Put screens away 20–30 minutes before lights out if you can.
Bedroom airflow triage
- Turn fans away from your face (or off, if possible).
- Avoid sleeping directly under a vent stream.
- If heating dries you out, balance temperature with humidity rather than blasting hot air.
If you change one thing: keep screens out of bed
This is the habit that quietly cancels your warm compress. Bed becomes “the place you blink less” and “the place the air hits your face.” If you want a single lever, make the bed screen-free for a week. Your future morning might surprise you.
Confession: I used to “wind down” with my phone in bed. I called it relaxation. My eyes called it overtime.
Common mistakes: the fastest ways to make dry eyes worse
Let’s do the loss-prevention part—because it’s cheaper, faster, and usually the reason people think “nothing works.”
Overheating the compress (or doing it once and quitting)
If it’s too hot, you’ll skip it tomorrow. If it’s only “special occasion self-care,” it can’t carry the load.
Under-cleaning the humidifier
A dirty tank is the opposite of soothing. If you can’t keep up with the cleaning schedule, shrink the solution. You can win without a complicated setup.
Scrubbing too hard: inflammation pretending to be cleanliness
When the lid margin gets irritated, everything feels worse—especially dryness. “Gentle and consistent” beats “aggressive and rare.”
Changing three variables at once
If you swap the humidifier, cleanser, drops, and pillowcase in one night… you’ll have no clue what helped. Your routine becomes a mystery novel you didn’t ask for.
Using water with contact lenses
The CDC is blunt about avoiding water exposure with contacts (showering, swimming, rinsing), because it can raise infection risk. If water hits your lenses, the safest response is usually to remove them and follow proper disinfection guidance.
- Too hot → you quit
- Too harsh → you inflame
- Too many changes → you can’t learn
- Too much airflow/screens in bed → you undo the work
Apply in 60 seconds: Choose one variable to change this week—only one.
When to seek help: don’t white-knuckle these symptoms
Home routines are for comfort and maintenance. But some symptoms deserve a clinician, not a “wait and see” pact—especially if you want to show up prepared with an annual eye exam checklist for seniors and the right questions.
Same-day / urgent
- Sudden vision changes
- Severe eye pain or rapidly worsening symptoms
- Marked light sensitivity
- Eye injury or chemical exposure
Within 24–48 hours
- Thick discharge, significant swelling, fever
- Worsening redness that doesn’t settle
- Contact lens pain, especially if sharp or increasing
If it’s chronic and you’re doing “everything”
Ask about eyelid inflammation (blepharitis), oil gland dysfunction, allergies, and whether your lid closure during sleep might be incomplete. This is where a personalized plan can beat generic advice.
FAQ
1) What humidity should my bedroom be for dry eyes?
Many indoor air-quality guides emphasize keeping humidity in a moderate range—comfortable for breathing and less likely to cause condensation and mold issues. If your room is extremely dry, modest humidity plus airflow changes can reduce overnight evaporation. If your room is already humid, focus more on lid routine and trigger control.
2) Cool-mist or warm-mist humidifier—which is better for sleeping?
Either can add moisture. The more important factors are cleaning ease, noise level, and whether you can keep it from misting directly onto bedding. If you’re choosing between two, pick the one you will actually clean and actually use.
3) How long should I use a warm compress for meibomian glands?
Most at-home routines aim for several minutes of comfortable warmth. The key is steady warmth (not scorching heat) and consistency. If you’re unsure, a clinician can recommend a plan that fits your specific symptoms.
4) Can eyelid hygiene sting at first—and when should I stop?
Mild sensation can happen, especially if your skin is sensitive or you’re using a new product. Stop and reassess if you get worsening burning, significant redness, swelling, or pain. In that case, simplify the routine and consider clinician advice.
5) Are eyelid wipes better than diluted baby shampoo?
“Better” often means “more tolerable and more consistent.” Wipes can be easier and more standardized. Diluted cleanser methods can be cost-effective but may irritate some people. Try one approach for a week before switching so you can actually measure results.
6) Can I do warm compresses every night?
Many people do, especially when eyelid inflammation or clogged oil glands are part of the story. The guardrails are comfort and skin tolerance—if the skin feels irritated, reduce heat, pressure, or frequency.
7) What’s the safest way to clean a humidifier to avoid mold?
Follow the manufacturer’s instructions, keep the tank from sitting with stagnant water, and stick to a routine you can maintain. If you see buildup or smell anything “off,” treat it as a signal to deep clean or pause use until it’s back to clean.
8) Is it safe to rinse my eyes with tap water?
In general, eyes and water can be a risky mix if you wear contact lenses. The CDC specifically warns against exposing contacts to water (including showering and swimming), because water exposure can increase infection risk. If you don’t wear contacts and you’re flushing an irritant, follow clinician guidance and use appropriate sterile solutions when available.
9) Why are my eyes worse in the morning than during the day?
Nighttime is prime time for evaporation: fewer blinks, drier air, airflow from vents/fans, and sometimes incomplete lid closure. A bedtime routine addresses the environment (humidity/airflow) and the lid margin (warmth + gentle cleaning) to reduce that overnight drop.
10) If I wear contacts, what’s the #1 bedtime rule to reduce infection risk?
Keep water away from contact lenses—no rinsing, no showering with lenses, no swimming with lenses. If water touches your lenses, remove them and follow safe disinfecting steps before wearing them again.
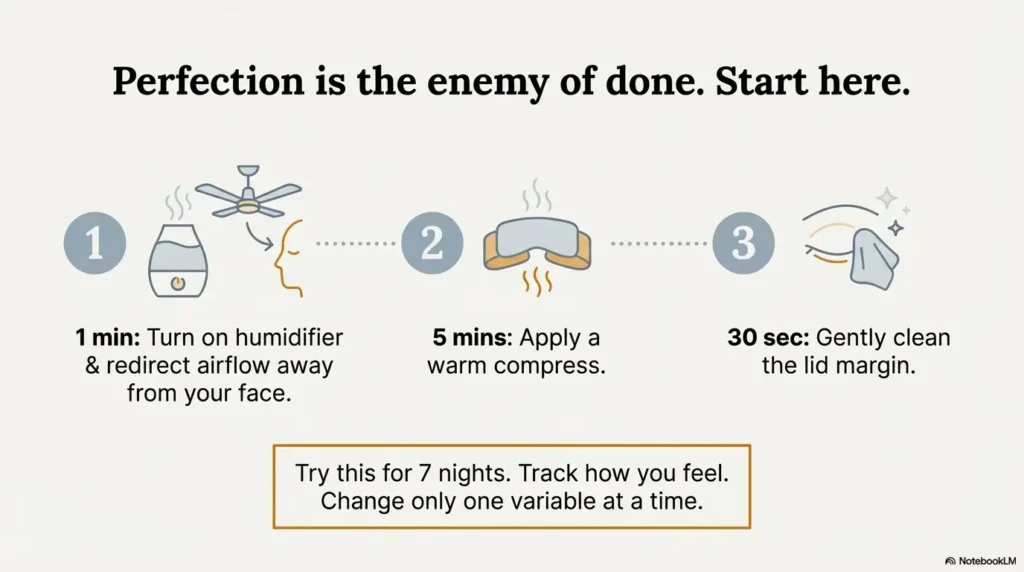
Next step tonight: do the “minimum viable” 6 minutes (then repeat 7 nights)
If you’re tired, do the small version. The routine works because it’s repeatable—not because it’s fancy.
Minute plan (6 minutes)
- 0:00 — Turn the humidifier on (and turn off/redirect face airflow).
- 0:30 — Warm compress on closed lids (comfortable warmth).
- 5:30 — Gentle lid-margin clean (short, light strokes).
Track 3 numbers for 7 mornings
- Gritty (0–10)
- Redness (0–10)
- Blur (0–10)
If you want an easy way to stay consistent, use a printable symptom diary for seniors so you can actually see patterns instead of guessing from memory.
Only after 7 nights: change one variable
Pick just one: humidity target, compress tool, or cleanser. If you change three things, you’ll learn nothing—and you’ll blame yourself for the confusion.
- 6 minutes is enough to start
- 7 nights gives you a fair test
- Change one variable at a time
Apply in 60 seconds: Put a sticky note on your humidifier: “ON + CLEAN.”
My favorite part of a routine like this is psychological: it turns bedtime from “I hope I wake up okay” into “I did the reasonable thing.” That matters.
Conclusion: close the loop (and make tomorrow morning easier)
Remember the open loop—the habit that cancels your warm compress? It’s usually screens in bed + airflow to the face. You can warm your lids and clean the margin perfectly, then lose the night to dry moving air and a blink-free scroll session.
So here’s the honest CTA: don’t overhaul your life. Run the 6-minute minimum tonight. Keep the room moderate. Keep the compress comfortable. Keep the lid cleaning gentle. Track three numbers for a week. If you improve, you’ve earned the right to stay simple. If you don’t, you’ve earned the right to escalate to clinician-level personalization—without guessing.
Last reviewed: 2025-12-19

