
Printable Symptom Diary for Seniors: Track Changes in Your Vision Week by Week – 7 Life-Saving Lessons from My Mom’s Scary Vision Crisis
The night my mom squinted at the TV and said, “The words are swimming,” I didn’t respond with some inspirational quote about resilience. Honestly, I just froze for a second… then grabbed a notebook.
That scrappy little “vision diary” I started on a whim? Within six weeks, it helped her eye doctor spot a pattern, rush the right tests, and catch something just in time—something that could’ve led to permanent vision loss if we’d waited. No dramatic interventions, no all-caps Googling at 2 a.m.—just a pen, paper, and a few scribbled notes each day.
Here’s what I learned: when a parent says, “It’s just age,” what they usually mean is, “Please don’t make a fuss.” But data? Data is quiet. It doesn’t argue. A simple, printable symptom tracker can do what panic never will—it turns fuzzy “I dunno, maybe?” moments into clear trends a doctor can actually use.
In this guide, I’ll show you how to make a one-page weekly diary that even the most stubborn loved one won’t hate. I’ll walk you through what to track, how to bring it up without triggering their “I’m fine” defense, and seven lessons I learned the hard way—so maybe you won’t have to.
You’ll also learn how to use this little tool during real appointments, how to get your parent (sort of) on board, and how to do a 60-second check-in right now—before the next “It’s nothing, really” turns into an avoidable emergency.
Table of Contents
Why a printable vision symptom diary matters more than you think
Vision loss in older adults is common, but that doesn’t make it inevitable or untreatable. In richer countries, millions of people over 65 live with vision impairment that could often be slowed, treated, or even prevented with earlier detection. The catch? Early changes are usually subtle and easy to shrug off.
That’s where a printable vision diary comes in. It doesn’t diagnose anything. It simply turns “I don’t know, it’s been getting worse for a while” into concrete notes like, “Trouble reading small print in the evening, three times this week, right eye worse.” Eye doctors love that kind of detail. It lets them see patterns in weeks instead of years.
When you write things down:
- You notice changes sooner (because “once in a while” might actually be “three times this week”).
- Your parent has something to lean on when their memory blanks in the exam room.
- The doctor can prioritize testing, referrals, and treatment based on real patterns, not fuzzy recollections.
I still remember my mom squinting at her crossword and saying, “The letters look pale today.” Two months earlier, that would’ve been a random complaint. With the diary, it became a data point—one of many pointing toward something we needed to act on.
- Write down what you see, not what you fear.
- Look for patterns: time of day, which eye, which activity.
- Bring the diary to every eye appointment.
Apply in 60 seconds: Grab any sheet of paper and write today’s date, “Right eye,” “Left eye,” and one sentence about how things looked today.
Who should use this diary (and who probably doesn’t need it yet)
Not every older adult needs a printed symptom diary. Some are already seeing an eye specialist regularly, have stable conditions, and remember everything. Others are walking around insisting they “just need better lighting” while holding the newspaper three inches from their nose.
Think of this diary as a low-tech safety net for seniors who are:
- Noticing new or changing vision symptoms.
- Losing track of which day something happened.
- Juggling multiple conditions like diabetes, glaucoma risk, or macular degeneration.
- Being politely ignored when they tell busy doctors, “It’s been weird lately.”
Here’s a quick way to decide if it’s worth starting.
Money Block #1 – Eligibility checklist: Who should start a printable vision diary today?
Answer “yes” or “no” for your mom (or older loved one):
- Age 60+ and no eye exam in the last 12–24 months.
- Has diabetes, high blood pressure, or a strong family history of glaucoma or macular degeneration.
- Recently said something like “the lines are wavy,” “colors look dull,” or “the print keeps blurring.”
- Has tripped, misjudged steps, or missed curbs more than once in the last 3 months.
- Gets headaches or eye strain after reading or screen time.
If you answered “yes” to 2 or more: a printable symptom diary is a smart, low-cost way to prepare for the next eye exam.
If you answered “yes” to 4 or more: start the diary and schedule an eye appointment within the next few weeks.
Save or print this checklist and confirm any specific recommendations with your eye care provider.
When I ran this checklist on my mom in hindsight, we hit four “yes” responses without even trying. If I’d done it earlier, we might have shaved a stressful month off her diagnosis journey.

How my mom’s scary vision crisis taught us to write things down
My mom’s crisis didn’t start with lightning bolts or dramatic darkness. It started with “The streetlights look smudged tonight.” We both laughed it off, because it was late and we were tired. A week later: “These book pages look a little yellow, don’t they?” Another shrug.
Only when she stopped midway through her favorite mystery novel and said, “I can’t keep the lines straight,” did my stomach drop. In the clinic, though, something familiar happened. The doctor asked, “When did this start?” and my mom, usually razor-sharp, said, “Oh, I don’t know…recently.”
That’s the quiet trap many seniors fall into:
- Symptoms drift in slowly.
- They normalize them (“Everyone’s eyes get tired”).
- By the time they’re worried enough to see someone, the timeline is a blur.
After that appointment, we sat at her kitchen table with a cheap spiral notebook. I drew three columns—Date, Right Eye, Left Eye—and added one more called “What I was doing.” It was the opposite of fancy. But over a few weeks, her scribbles—“darker than usual,” “letters fade after 10 minutes,” “hard to see faces across the room”—painted a picture we hadn’t seen before.
When we brought that notebook back, the doctor paged through it, frowned, and said, “I want imaging sooner rather than later.” That “sooner” probably saved vision in one eye.
“Your mom doesn’t have to remember perfectly—her diary can remember for her.”
- Start the diary before the next appointment.
- Ask your parent to jot notes in their own words.
- Keep the paper where they already sit: by the TV, favorite chair, or bedside.
Apply in 60 seconds: Put a pen and notebook where your mom usually reads or watches TV and label the top of the page “Vision Today.”
How to set up your printable symptom diary step-by-step
You don’t need a designer, an app, or a subscription. You need one printable page and a pen. Think “checklist meets calendar,” not “art project.” If it’s too pretty, your parent will be afraid to “mess it up.”
Here’s a simple weekly layout you can copy into Word, Google Docs, or any basic editor and print:
| Date | Time of day | Right eye | Left eye | Activity (reading, TV, walking, driving) | Light (dim / normal / bright) | Headache / pain (Y/N) | Notes |
|---|---|---|---|---|---|---|---|
| Print 2–3 copies and keep them in the same place every week. | |||||||
When I gave my mom her first printed page, she rolled her eyes and said, “This looks like homework.” A week later, she was filling it in more faithfully than her crossword, mostly because it took less than a minute per entry.
Tips that make seniors more likely to use the diary:
- Use big fonts. 14–16 pt, clear sans-serif. No delicate cursive.
- Keep it one page. If it feels endless, they’ll avoid it.
- Allow “messy.” Scribbles, arrows, and “not sure which eye” are still better than silence.
- Add a weekly “big picture” box: “Overall this week my vision felt…” with options: same / slightly worse / much worse.
Show me the nerdy details
Paper diaries win in older adults because they’re visible, tangible, and don’t require passwords, updates, or remembering how to open an app. Research on habit formation suggests that making the action shorter than 30 seconds and attaching it to an existing routine (like TV time or evening tea) drastically increases follow-through. Your goal is not perfect data; it’s consistent data that your parent can record on “tired days” without thinking.
- One page per week is ideal.
- Big fonts beat beautiful fonts.
- “Good enough” entries beat perfection.
Apply in 60 seconds: Open any word processor, create a simple 8-column table like the one above, and print 3 copies.
What to track week by week: 7 life-saving lessons from my mom’s crisis
My mom’s diary taught us that it’s not only what you track but how you describe it. These seven lessons came straight from her kitchen table.
Lesson 1 – Track which eye is worse, even if you’re not 100% sure
Mom’s earliest notes said “both eyes tired.” A month later, we saw more “right eye fuzzy” entries. That side-to-side difference helped the doctor pinpoint where to look first.
Lesson 2 – Time of day matters more than you’d think
She wrote “evening TV: faces blurry” several times before we realized her symptoms flared when she was tired. That pattern suggested more than just dry eyes.
Lesson 3 – Activities reveal hidden problems
A senior who only notices trouble when reading small print is different from one who gets lost walking to the bathroom at night. A diary that distinguishes “reading, walking, stairs, driving, TV” turns random complaints into diagnostic clues.
Lesson 4 – Don’t skip the “weird one-off” days
One of my favorite entries of my mom’s reads, “Wednesday: grocery store lights too bright, words dancing.” She almost didn’t write it down because it felt “dramatic.” That one line ended up being a major clue.
Lesson 5 – Add how you felt, not just what you saw
Words like “dizzy,” “uneasy,” or “afraid of falling” are clinically useful. They also give the doctor a sense of urgency that “a bit blurry” doesn’t.
Lesson 6 – Track headaches, eye pain, and halos
Headaches behind the eyes, pain when moving the eye, or halos around lights can be important. The diary gives them a place to live instead of being lost in “Oh, I get headaches sometimes.”
Lesson 7 – Mark the “first time I noticed this” as clearly as possible
When did “normal” change? A star, a colored pen, or a highlighted row around that first “something is off” entry can be priceless later.
Short Story: One Thursday afternoon, my mom wrote: “3 p.m., reading – middle of page looks like a gray cloud.” She almost erased it, thinking, “That sounds silly.” The next day, she saw it again and circled both entries with a shaky red pen. By Monday, we were in the retina specialist’s office. When he flipped through her diary and saw those two red circles, he said, “You came at the right time.” It wasn’t magic; it was ink and timing. But in that moment, it felt like we’d been handed a second chance in ballpoint.
Money Block #2 – 60-second vision risk estimator (not a diagnosis)
This quick check won’t tell you what’s wrong, but it can tell you whether to act today or “soon.”
This tool is for planning, not diagnosis. When in doubt, err on the side of calling your eye doctor.
Save this block and confirm timing with your own provider, especially if you have diabetes or known eye disease.
What eye exams really cost after 65 in 2025 (US): out-of-pocket vs coverage
A printable diary is free. The eye exam that follows? Not so much—and cost is one big reason seniors delay care. In the United States, routine eye exams for glasses are often not covered by original Medicare, which means many people over 65 pay the full amount for those visits.
On the other hand, certain medically necessary eye services—like glaucoma screening for high-risk groups or exams for diabetic retinopathy—are covered under Medicare Part B, typically at 80% after the deductible, leaving patients with about 20% of the approved amount as coinsurance. That gap can still feel painful if money is tight, but it’s much cheaper than emergency care and potential long-term disability costs.
Private Medicare Advantage plans, supplemental insurance, and standalone vision plans may cover more routine exams, but the rules vary widely. This is where your parent’s diary becomes powerful: it helps justify medically necessary care and makes conversations with insurers and providers much more specific.
Money Block #3 – Sample fee and coverage table for senior eye exams (US, 2025)
| Service type | Typical price range | Who often pays | Notes |
|---|---|---|---|
| Routine eye exam for glasses | $80–$200+ | Patient (original Medicare usually doesn’t cover) | May be discounted via vision plans or retail chains. |
| Medically necessary exam (sudden change, disease follow-up) | Clinic-dependent, often higher than routine exams | Medicare Part B / insurer + patient coinsurance | Documentation of symptoms helps justify medical necessity. |
| Glaucoma screening (high-risk groups) | Varies by provider | Often 80% covered by Part B after deductible | Available yearly for qualifying high-risk patients under Part B. |
| Diabetic eye exam | Varies; often bundled with other care | Frequently covered annually under Part B | Strongly recommended every year for people with diabetes. |
All numbers are approximate and vary by location and provider. Always confirm current prices and coverage with your clinic and insurer.
Save this table and confirm the current fee and coverage rules on your provider’s and insurer’s official pages.
Out-of-pocket cost for a Medicare Part B glaucoma screening after a sudden vision change, 2025 (US)
If your mom qualifies as high risk—for example, she has diabetes or a family history of glaucoma—Medicare Part B may cover annual glaucoma screenings at 80% of the approved amount once the annual deductible is met. The remaining 20% coinsurance is typically your out-of-pocket share, unless a supplemental plan helps cover it. For seniors on tight budgets, knowing this difference can be the nudge they need to schedule an exam instead of delaying it “until next year.”
Show me the nerdy details
From a cost–risk standpoint, even a $40–$80 coinsurance for a medically necessary exam is small compared with the long-term financial impact of vision loss: assistive devices, home modifications, lost independence, and higher fall risk. Health economists often talk about “avoiding downstream costs.” Your mom’s diary, by prompting timely exams, is a tiny investment that can reduce the odds of needing far more expensive interventions later.
- Check what your parent’s plan covers before booking.
- Use the diary to explain why the visit is medically necessary.
- Ask the clinic for an itemized quote with codes if money is tight.
Apply in 60 seconds: Call the number on your parent’s insurance card and ask, “How is a medically necessary eye exam billed under this plan for someone over 65 with new symptoms?”
Red-flag symptoms: when “wait and see” is dangerous
Not every blurry moment is an emergency. But some are. One quiet benefit of keeping a diary is that it trains everyone—parent, caregiver, doctor—to distinguish “log it and watch” from “drop everything and call.”
Red-flag symptoms that deserve immediate attention:
- Sudden loss of vision in one or both eyes.
- A curtain or shadow moving across the field of vision.
- Sudden flashes of light or a shower of new floaters.
- Severe eye pain, especially with nausea or vomiting.
- Sudden, dramatic change in central vision (faces or words distorted).
If any of these appear, you don’t wait for the diary to fill. You use the diary to explain exactly what changed and when.
Money Block #4 – Decision card: watch at home, call today, or seek urgent care?
| Situation | Action | Timing |
|---|---|---|
| Mild, occasional blur with reading; no pain; diary shows no rapid change. | Keep logging symptoms and follow your existing eye exam schedule. | Bring diary to next routine visit. |
| New or worsening blur, especially in one eye; more frequent diary entries. | Call eye clinic, describe diary entries, ask for earlier appointment. | Within days to a couple of weeks, based on clinic advice. |
| Sudden vision loss, flashes, curtain effect, or severe eye pain. | Seek emergency or urgent eye care; use the diary to give exact timing. | Same day, as soon as possible. |
Save this card and adjust it with your eye doctor’s specific guidance for your parent’s diagnoses.
If you’re outside the US—say, in a country with a national health service—the decision card still applies, even if the phone numbers and pathways differ. In the UK, for example, older adults may qualify for free eye tests, while in South Korea or other countries you may go directly to an eye hospital or specialist clinic. The diary travels well across borders, even when coverage rules don’t.
How to use the diary at eye appointments without wasting time
You’ve done the work. You printed the diary, your mom filled it out, you’ve circled the worrying bits. Now you’re in the exam room, and the clock is ticking. How do you use all this without derailing the appointment?
Here’s the simple script that worked best for us:
- Hand the diary to the nurse or doctor and say, “We tracked her vision for the last four weeks. The worst days are starred.”
- Point to one or two representative entries: “Here, the lines looked wavy; here, the center was gray.”
- Then stop talking. Let the professional ask follow-up questions.
In my mom’s case, this turned a vague conversation into a precise one:
- Without diary: “It’s been off for a while.”
- With diary: “These wavy lines started about six weeks ago and are now happening three times a week, mostly in the evenings.”
That level of detail helps the doctor decide whether to order imaging, adjust medication, refer to a specialist, or simply watch and repeat the exam later.
You can also gently ask:
- “Would it help if we keep this kind of weekly diary between visits?”
- “Is there anything specific you’d like us to track for the next month?”
Some clinics will even suggest small changes to your template—like adding a blood sugar column for someone with diabetic retinopathy or a “fall or near-fall” column if balance is becoming an issue.
- Lead with the scariest or most frequent symptom.
- Show, don’t monologue—let the doctor skim.
- Leave the diary with the clinic if they ask to scan it.
Apply in 60 seconds: Clip this week’s diary page to your parent’s appointment card or calendar so it actually makes it into the exam room.
Helping a reluctant parent stick with the diary
If your mom is anything like mine, she has a PhD in brushing things off. The first week I handed her the diary, she sighed and said, “Do I get college credit for this?” But underneath the jokes was fear—fear that writing things down made them more real.
Here’s what actually helped:
- Frame it as a favor to the doctor, not a homework assignment. “It’ll make their job easier.”
- Keep it tiny. One or two entries a day is enough.
- Pair it with a pleasant ritual. “Fill this out while your tea cools.”
- Do it together once in a while. I’d sit and say, “Let’s do today’s line together,” and she’d start talking.
One night, she joked, “I should charge my ophthalmologist a consulting fee for this paperwork.” I replied, “Great—your fee is paid in better vision.” She rolled her eyes, but she kept writing.
For caregivers who are exhausted (which is almost all of us), remember:
- You’re not aiming for a perfect scientific record.
- Even a partially filled diary is better than none.
- If your parent can’t or won’t write, you can be their “scribe” for a few weeks.
Show me the nerdy details
Behavior researchers often talk about “friction.” Every point of friction (finding the paper, finding a pen, deciding what to write) reduces the odds of follow-through. By keeping the diary in one spot, using checkboxes where possible, and attaching it to an existing routine, you remove friction and increase consistency—without nagging or guilt.
- Attach it to a daily ritual.
- Celebrate effort, not perfection.
- Offer to be the scribe when they’re worn out.
Apply in 60 seconds: Ask your mom, “When is the easiest time of day for you to jot one line about your eyes?” Then build the habit around that time, not yours.

Digital vs printable diary: which one actually gets used?
There are excellent apps and digital trackers for vision and health. But for many older adults, the winning solution is still…paper. No passwords. No software updates. No “I forgot which app it was in.”
That said, a hybrid approach can work:
- Printable diary for daily notes.
- Photos of key pages on your phone to share via patient portals or telehealth.
- Optional spreadsheet if you enjoy looking for trends over months (caregivers who love charts, I see you).
In countries with strong digital health systems, you might even be able to upload diary snapshots directly to your parent’s medical record or email them ahead of the visit. The key is always the same: use the tool that your parent will actually use consistently for at least a few weeks.
If you’re caring for someone in South Korea, the US, or another country with complex insurance rules, remember that written symptom timelines can support referrals, prior authorizations, and coverage decisions. A well-kept diary won’t replace formal documentation, but it can make those conversations more efficient and less stressful.
You can also cross-link your tracking with other resources, like a family history article or checklists about age-related eye disease, if you’re building a full “vision binder” at home.
Infographic: your weekly vision diary flow in 5 minutes
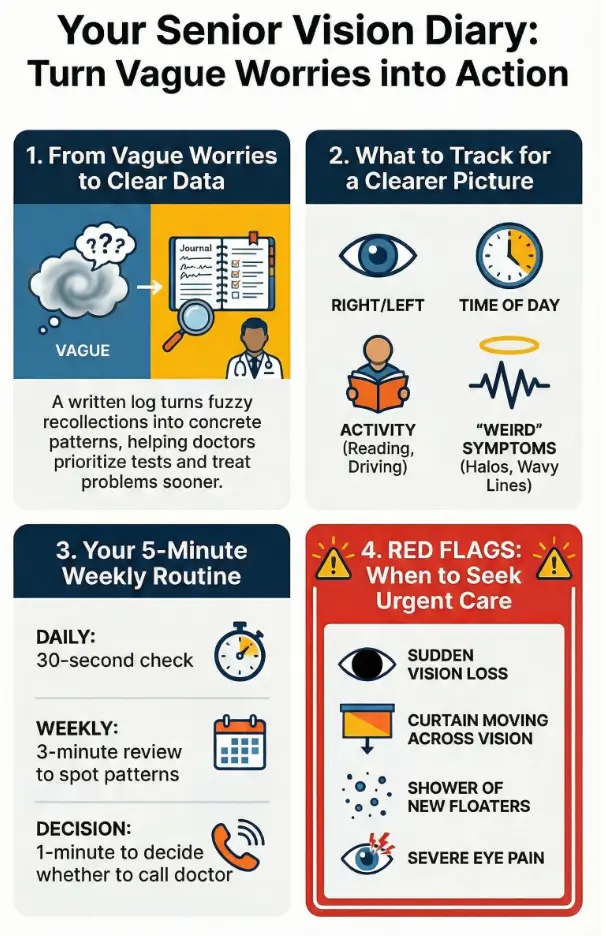
Weekly Vision Diary Flow (5-Minute Routine)
1. Daily check (30 seconds)
Once a day, ask: “How did my eyes behave today?” Jot one line in the diary.
2. Weekly review (3 minutes)
Circle bad days, star anything new or scary, and mark if the week felt better, same, or worse.
3. Decision check (1 minute)
Look at your circles and stars. Use the decision card and risk estimator to decide whether to call the clinic.
4. Appointment prep (1 minute)
Clip the latest pages together, add a sticky note with your top 2 questions, and bring them to the visit.
FAQ
Q1. How often should my mom get a dilated eye exam if she’s over 65?
Most major eye organizations recommend that adults 65 and older have a comprehensive, dilated eye exam every 1–2 years, even if they don’t notice symptoms. If she has diabetes, known eye disease, or strong family history, yearly—or even more frequent—visits may be recommended.
60-second action: Call her eye clinic and ask, “Given her age and conditions, how often do you want to see her?” Then write that answer at the top of the diary.
Q2. What if we start the diary and everything looks stable?
That’s actually great news. A stable diary is a reassuring baseline for future changes. Bring it to the next routine exam anyway; if things change later, you’ll know what “normal” looked like.
60-second action: At the end of a quiet week, write “Baseline week” across the top of the page and save it.
Q3. Can this diary help with insurance or Medicare coverage decisions?
It can’t replace formal documentation, but it can help your doctor justify medically necessary exams, tests, or referrals by showing a clear timeline of symptoms. That, in turn, can support coverage under benefits like Medicare Part B when certain criteria are met.
60-second action: Before the next visit, highlight any entries that show sudden or worsening symptoms and tell the doctor, “These are the days that worried us most.”
Q4. What if my parent has early memory issues or dementia?
A diary can still help, but you’ll probably take a bigger role. Instead of expecting them to write everything, you can observe and jot notes yourself—especially changes in walking, bumping into objects, or trouble recognizing faces. Vision impairment and dementia are closely linked in older adults, so keeping an eye (and a pen) on both is worth the effort.
60-second action: Add a simple row labeled “Falls, stumbles, or near-misses” to the weekly diary and mark any incidents.
Q5. Is it ever “too late” to start a symptom diary?
It’s never too late to start paying attention. Even a week or two of notes before an upcoming appointment can be helpful. If your parent already has a diagnosis—like glaucoma, cataracts, or macular degeneration—the diary can help track how well treatment and daily life are going, not just whether the condition has a name.
60-second action: Choose the date of the next appointment and write it at the top of a fresh diary page titled “Lead-up to visit.”
Q6. Should we use separate diaries for each eye disease (like diabetes, glaucoma, cataracts)?
Usually, one well-designed diary is enough. You can add simple tags or color codes for specific conditions (for example, a blue dot for diabetes-related notes, a green dot for glaucoma concerns). More than one diary often means none of them get filled.
60-second action: Agree on one template and add a small legend at the bottom: “Blue dot = diabetes,” “Green dot = glaucoma,” and so on.
Conclusion: your next 15 minutes
My mom still jokes that her “little eye spreadsheet” saved her from a much scarier outcome. She’s not wrong. The diary didn’t cure anything, but it gave her doctor a clearer view of what was happening between appointments—and gave us a way to act before her world got dimmer.
In the next 15 minutes, you can:
- Print a simple weekly diary page.
- Fill out today’s line with your mom (or for her).
- Run the 60-second risk estimator and, if needed, put “Call eye clinic” on tomorrow’s to-do list.
You don’t have to become an expert in eye disease overnight. You just have to capture what’s really happening, one line at a time, so that when your parent finally sits in that bright exam chair and hears, “So, tell me what’s been going on,” they’re not answering from memory—they’re answering from evidence.
Last reviewed: 2025-12. Informed by current guidance from public health and professional eye-care organizations.
For deeper dives, you may also want to read about family history of eye disease, how often seniors should get dilated eye exams, and the real blindness risk after 70.
You’ve already done something powerful by reading this far: you’ve decided your parent’s sight is worth tracking. Now give that decision a home on paper—and let the ink do some of the worrying for you.
Printable Symptom Diary for Seniors, vision symptom diary, senior eye exam checklist, tracking vision changes, caregiver tools for aging parents

