
By day three after LASIK, a “healthy” lunch can still end in 3 p.m. grit.
Your eyes aren’t asking for virtue. They’re asking for stability.
If you’re dealing with post-op dryness that spikes on screen days, feels worse under AC, or flares after restaurant meals, the problem usually isn’t effort. It’s a predictable mix of evaporation, sleep debt, and hydration timing—plus an omega-3 routine that’s too complicated to survive a real week.
A smart diet for dry eyes after LASIK isn’t about superfoods; it’s about removing the quiet triggers (sodium, alcohol, sugar crashes), keeping caffeine from creating spikes, and building a repeatable “water + oils + calm surface” rhythm. Keep guessing and you pay twice: uncomfortable eyes now, and weeks of buying fixes you can’t troubleshoot later.
Table of Contents
1) Dry eye after LASIK: what’s happening (and why diet still moves the needle)
LASIK is a corneal procedure, but dry eye is a whole-system experience. Your tear film is a layered “coat” that needs water, oils, and a calm surface to spread smoothly. After surgery, nerves involved in sensation and reflex tearing can be temporarily disrupted, blinking patterns can change, and the ocular surface can feel more sensitive.
This is why your day-to-day choices matter: not because kale is magical, but because hydration status, inflammation load, sleep quality, and oil availability can influence how stable that tear film feels hour by hour. Think of it like tuning a piano: the surgery changes the instrument; your routine decides whether it stays in tune.
- Evaporative dryness: tears evaporate too fast (often tied to oil layer/meibomian glands, airflow, screens).
- Aqueous dryness: not enough watery tear volume (hydration, medications, autoimmune factors can matter).
- Inflammatory loop: irritation → rubbing → more irritation (diet and sleep can influence this loop).
Personal note: I tried to “out-health” my symptoms with salads while working under an AC vent, blinking like a startled deer. Spoiler: the vent won.
- Stability comes from water + oils + calmer surface habits.
- Diet helps most when it’s consistent and measurable.
- Your environment (screens/airflow/sleep) can overpower “healthy eating.”
Apply in 60 seconds: Notice where air hits your face right now—vent, fan, car heater—and redirect it away from your eyes.
Open loop: There’s a daily routine that cancels “healthy eating” without you noticing—and it’s not your lack of discipline. We’ll name it later.
2) Who this is for / not for (so you don’t waste 2 weeks)
If you’re time-poor, screen-heavy, and you want something you can run on autopilot, this guide is for you. (If your screen time is the main accelerator, you may also want the deeper “why” behind digital eye strain and screen-driven dryness patterns—the mechanics are similar even if your age isn’t.) But if your symptoms are red-flag intense, don’t use diet as a substitute for medical care. Use it as support.
Best fit: mild–moderate symptoms + screen-heavy days
- Dryness that fluctuates through the day (often worse mid-to-late afternoon).
- Grittiness, burning, “tired eyes,” or blur that improves after blinking/drops.
- Symptoms clearly influenced by screens, wind, travel, dehydration, or salty meals.
Not enough: situations that need clinician input now
- Increasing pain, strong light sensitivity, discharge, fever, or sudden vision changes.
- Severe symptoms that don’t ease at all with basic measures.
- Known autoimmune disease or significant ocular surface disease history.
Supplement caution list (common-sense safety)
Omega-3 supplements are not “bad,” but they’re not neutral for everyone. If you’re on blood thinners, have bleeding risk, are pregnant, or your surgeon has post-op restrictions, ask before starting or stacking supplements. (Food-first is the easiest safety move.)
Personal note: I once started a “helpful” supplement stack after a procedure because the label looked comforting. My stomach disagreed loudly. My lesson: if your plan is unsustainable, it’s not a plan.
- If you’re unsure: default to food sources, and keep changes simple for 14 days.
- If you’re already taking supplements: don’t add more “just in case.” Measure what you’re doing first.
3) Omega-3 timing after LASIK: “timing” = absorption + consistency + patience
Omega-3 advice is everywhere—and somehow still vague. Timing matters in three ways: absorption (how your body actually takes it up), consistency (whether you’ll keep doing it), and patience (whether you quit right before it could help).
Food-first omega-3 schedule: simple, repeatable
If you do one thing, do this: pick two fish meals per week and lock them to days that already have structure (e.g., Tuesday dinner + Saturday lunch). Consistency beats heroic bursts.
- Easy grocery wins: canned salmon, sardines, trout fillets, or frozen salmon portions.
- If you hate fish: consider algae-based omega-3 as a conversation with your clinician (not a self-prescription moment).
- Support fats: olive oil, avocado, nuts—helpful for meals, and often better tolerated than isolated oil capsules.
Supplement timing: the “take it with food” rule (and why)
If your surgeon/clinician says supplements are fine, take omega-3 with a fat-containing meal. This is less about ritual and more about absorption and stomach comfort.
- Breakfast with eggs/avocado? Good.
- Lunch with olive-oil dressing? Good.
- Empty stomach + coffee + fish oil? That’s how people accidentally decide omega-3 “doesn’t work.”
Dose reality: why “more” isn’t always better
You don’t need a supplement arms race. High doses can cause side effects (GI upset, reflux, “fish burps”), and if it makes you quit, it fails the only metric that matters: did you do it long enough to judge?
Let’s be honest—most people quit right before it could help
This is the classic pattern: Week 1, motivated. Week 2, “I missed a day, so I’m behind.” Week 3, life happens. Week 4, you declare it “did nothing.” The fix is not more intensity. The fix is frictionless design.
- Make it boring: tie it to one meal you rarely skip.
- Make it visible: keep the chosen food/supplement where you already reach daily (not buried behind chia seeds you bought once).
- Make it measurable: track comfort and screen tolerance (we’ll do this in the 14-day plan).
Show me the nerdy details
Omega-3s (EPA/DHA) are incorporated into cell membranes over time; that’s one reason “I took it for three days” rarely tells you anything. Absorption is generally improved with dietary fat, and tolerability often improves when taken with meals. For post-procedure contexts, clinicians may also consider bleeding risk and medication interactions—another reason food-first is a sensible baseline.
Personal note: The first omega-3 routine that stuck for me wasn’t the “perfect” one. It was the one that survived a bad week.
Open loop: There’s a label phrase that makes you think you’re covered when you’re not. We’ll unpack it in the vitamins section.
4) Hydration targets that don’t backfire (US-friendly, measurable)
“Drink more water” is the most common advice—and also the easiest to do in a way that backfires. The goal isn’t to drown yourself; it’s to stay steadily hydrated so your body isn’t constantly playing catch-up.
The “pale-yellow by midday” rule + a simple triad
Instead of obsessing over ounces, use a practical checkpoint: aim for pale-yellow urine by midday. Add two more signals: thirst and headache. If all three line up, you’re probably under-hydrated.
- Signal 1: darker urine by late morning → you’re behind.
- Signal 2: constant thirst → your intake is lagging your needs.
- Signal 3: frequent mild headache → common dehydration clue (not the only cause, but a useful flag).
- Use midday “pale-yellow” as your checkpoint.
- Pair water with meals to make it automatic.
- Avoid sugary/salty “hydration” hacks unless you truly need electrolytes.
Apply in 60 seconds: Fill one bottle/glass now and place it where your mouse/keyboard lives.
Electrolytes: when helpful vs when they worsen dryness
Electrolytes can be useful if you’re sweating heavily, dealing with GI illness, or in heat. But many “electrolyte drinks” are basically flavored sodium delivery systems—sometimes with sugar on top. If your dry eye flares after salty foods, you don’t want to accidentally turn your hydration into a salt load.
- Helpful: heavy sweat, long workouts, heat exposure, illness-related fluid loss.
- Not helpful: office days, light activity, “I just want something tasty.”
- Practical alternative: water + a meal with normal salt (not a neon sports drink as your daily baseline).
Caffeine timing: avoid spikes/crashes that trigger “compensatory dehydration”
Caffeine isn’t automatically evil. The bigger issue is the spike/crash pattern: big morning caffeine, little water, then a late-day slump. That slump often comes with mouth dryness, eye irritation, and the urge to “fix it” with more coffee.
- Try this: water first, then coffee.
- Or: pair coffee with a full glass of water, every time.
- Avoid: energy drinks as hydration (they often combine caffeine + sugar + additives).
Here’s what no one tells you about “just drink more water”
If you’re drinking tons of water at night, you’ll wake up to pee, sleep worse, and feel drier the next day. Hydration is a daytime practice. The best “hydration plan” is one that doesn’t sabotage your sleep.
Show me the nerdy details
Tear film comfort is influenced by systemic hydration status, but also by evaporation rate (airflow/screens) and inflammatory signaling. Overcorrecting hydration late in the day can fragment sleep, which can worsen symptom perception and recovery. Practical targeting (midday checks, meal pairing) tends to outperform rigid ounce-counting for real-life adherence.
Personal note: My driest days weren’t the days I forgot water entirely. They were the days I remembered water at 10 p.m.—like a guilty apology.
5) What to avoid after LASIK (the fast-track flare triggers)
If you’re looking for the quickest relief, focus less on “superfoods” and more on avoiding the predictable flare triggers. These are the things that make you wake up feeling like your eyelids are sandpaper sleeves.
Alcohol: why even small amounts can feel brutal the next day
Alcohol is a classic “sleep + hydration” double hit. You may fall asleep faster, but the sleep quality often suffers—and dehydration risk rises. The next day, dryness can feel louder, especially if you add travel, late-night salt, or a screen-heavy morning.
- Reality check: You don’t have to “never drink.” But if you’re flaring, treat alcohol as an experiment, not a default.
- Easy mitigation: alternate alcohol with water, and avoid salty “bar snacks” as your dinner.
Restaurant sodium: the hidden reason your eyes burn tomorrow
Restaurant meals can be sodium-dense even when they taste “normal.” That salt load can shift fluid balance and make you feel thirstier later—often when you’re not in a good position to hydrate well. The next morning, the dryness can show up like a bill you didn’t remember signing.
- High-risk meals: ramen, fast food, deli sandwiches, pizza, wings, anything “smothered” or “loaded.”
- Low-friction fix: ask for sauce on the side, choose grilled options, add a simple side salad, and drink water before the meal arrives.
Ultra-processed + high sugar: inflammation + poor sleep spiral
High sugar and ultra-processed foods can push cravings, crash energy, and nudge sleep in the wrong direction. Sleep is when your whole system tries to repair, and dry eye recovery is not a fan of 2 a.m. doom scrolling fueled by cookies.
- Swap idea: if you want sweet, pair it with protein/fiber (Greek yogurt + berries, nuts + fruit) to soften the spike.
- Practical truth: the best plan is the one you can repeat on your worst day.
Personal note: I used to blame my eyes for being “dramatic,” then I tracked flare-ups after takeout nights. My eyes were not dramatic. My sodium was.
6) The anti-inflammatory plate (LASIK edition): build meals that don’t require motivation
Motivation is a flaky friend. Build a plate you can assemble when you’re tired, busy, or annoyed at your own eyeballs. You want a formula, not a philosophy.
Plate formula: protein + color + fat + fiber (5-minute examples)
- Protein: eggs, chicken, tofu, Greek yogurt, beans.
- Color: leafy greens, carrots, peppers, berries (pick one).
- Fat: olive oil, avocado, nuts (small portions are enough).
- Fiber: oats, brown rice, quinoa, lentils, veggies.
Examples that don’t require a personality transplant:
- Breakfast: oatmeal + walnuts + berries (add yogurt if you want more protein).
- Lunch: tuna/salmon packet + salad kit + olive oil drizzle.
- Dinner: frozen salmon + microwave rice + bagged greens.
Best fats: portion realism (so it’s sustainable)
Healthy fats help, but portion creep is real. A “healthy” snack can become a calorie avalanche (hello, nut butter spoon). Aim for a measured handful of nuts, a slice of avocado, or a drizzle of olive oil—enough to support you, not overwhelm you.
7-day grocery list (US staples) mapped to your week
- Omega-3 anchor: salmon (fresh or frozen), sardines (optional), tuna packets.
- Proteins: eggs, chicken, tofu, Greek yogurt.
- Carbs/fiber: oats, microwave brown rice, quinoa, beans/lentils.
- Color: spinach/greens, carrots, peppers, berries.
- Fats: olive oil, avocado, mixed nuts.
- Pick 2 omega-3 meals weekly and repeat them.
- Make meals “assembly-based” when energy is low.
- Support recovery by protecting sleep and steady hydration.
Apply in 60 seconds: Choose your two omega-3 meals for this week and put them on your calendar.
Short Story: I once tried to “eat clean” after a procedure with a complex meal plan. Day 3, I was standing in my kitchen at 9 p.m., hungry, squinting at a recipe that required five pans and a calm spirit. I made cereal instead, felt guilty, and then—because guilt is an efficient liar—ordered takeout the next day.
That’s when it clicked: the plan wasn’t failing because I lacked discipline. The plan was failing because it wasn’t built for a human with a job, a phone, and a tired brain. When I switched to a plate formula—protein, color, fat, fiber—my week stopped swinging between perfection and collapse. My eyes didn’t become “fixed,” but my flare-ups became less mysterious. (120–180 words) …
7) Vitamins & eye nutrients: keep what’s evidence-aligned, skip what’s risky
The supplement aisle is a concert hall of loud promises. Your job is not to buy every instrument. Your job is to play one clean melody. For most people, the safest move is food-first, then targeted supplementation only if a clinician agrees it fits your situation.
Common nutrients you’ll hear about (and what they’re for)
- Vitamin A: important for ocular surface health, but more isn’t automatically safer—especially via supplements.
- Vitamin C: supports general tissue health and antioxidant roles (food sources are usually enough).
- Zinc: involved in many cellular processes; best handled through diet unless advised otherwise.
- Lutein/zeaxanthin: often discussed for retinal health; food sources include leafy greens.
Vitamin A caution: “more” can be a bad plan
Vitamin A is one of those nutrients where excessive supplementation can be risky. If you’re considering a high-dose product, that’s a “talk to your clinician” moment, not a “TikTok said so” moment.
The label phrase that tricks people
Here it is: “Eye health blend” (or any version of “proprietary blend”). It sounds comprehensive, but it often hides amounts, stacks many ingredients, and makes it hard to tell what you’re actually taking. If you can’t measure it, you can’t troubleshoot it.
- Better approach: one change at a time, tracked for 14 days.
- Better source: foods that naturally bring nutrients without extreme dosing.
- Better outcome: fewer variables, clearer cause-and-effect.
Personal note: My most expensive supplement phase was also my least informative. I had five bottles and zero clarity.
8) Common mistakes that keep LASIK dryness stuck (loss-prevention section)
This section exists to save you time and money. Because the fastest way to stay uncomfortable is to work hard on the wrong things.
Mistake #1: Starting/stacking supplements without clearance post-op
Post-procedure instructions can vary. If you add multiple supplements at once, you can’t tell what helps, what irritates your stomach, or what conflicts with your surgeon’s plan. Keep it simple. Keep it trackable.
Mistake #2: “Hydration” via sugary drinks or salty broths
Many “hydration” drinks add sugar and sodium, which can worsen the very patterns you’re trying to calm. Water + meals + steady daytime intake is usually the boring winner.
Mistake #3: Cutting caffeine cold turkey → rebound harder
If you cut caffeine abruptly, headaches and fatigue can spike, sleep can get weird, and you may end up “making up for it” with more caffeine later. If caffeine is a trigger for you, taper gently and pair it with water.
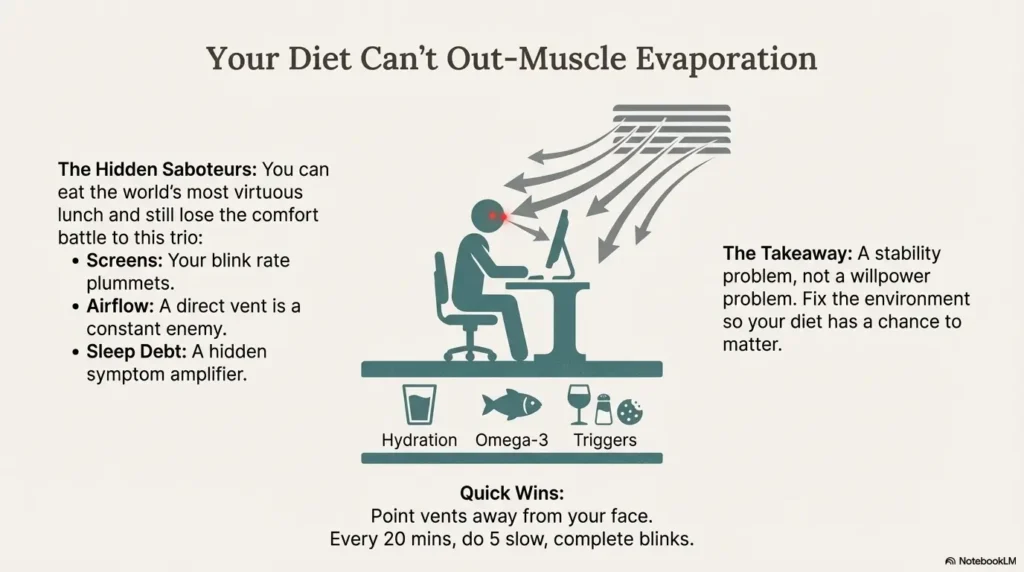
Mistake #4: Ignoring screens, sleep, and airflow
Diet can’t out-muscle evaporation. If your blink rate drops during screens, or air blasts your face all day, your tears will evaporate faster. Fix the environment and habits alongside nutrition. (If you want a frictionless add-on, borrow a simple bedtime pattern from this 15-minute night routine for dry eyes—it pairs beautifully with the “hydrate earlier” rule.)
- Screen hack: every 20–30 minutes, do 5 slow blinks (fully closing for 1 second).
- Airflow hack: point vents away from your face; consider a small desk humidifier if your room is very dry.
- Sleep hack: keep hydration earlier in the day to protect sleep continuity.
- Change one lever at a time so you can learn.
- Protect sleep; it’s a hidden symptom amplifier.
- Fix airflow/screens so diet has a chance to matter.
Apply in 60 seconds: Set a recurring reminder for 3 slow blinks every 30 minutes during work.
Personal note: The day I moved my desk away from the vent, my “diet plan” started working better—without changing a single meal.
9) Dry-eye toolbelt beyond diet (keep the intent—make it sharper)
Diet is support, not the whole toolkit. If you want the highest-yield comfort basics, here’s the operator list—organized by what it helps.
Artificial tears + preservative-free logic
If you’re using drops frequently, preservative-free options are often preferred because repeated preservatives can irritate some eyes. Your clinician’s plan comes first—follow their specific drop schedule if you have one. (If you’re deciding what “preservative-free” really means in practice, this guide to preservative-free eye drops and how to choose them safely can help you avoid the usual shopping traps.)
Warm compress + lid hygiene (when oil glands are the bottleneck)
If your symptoms feel “evaporative” (worse with screens, wind, AC), your oil layer may be struggling. Warm compresses and gentle lid hygiene can help support meibomian gland function for some people.
Humidifier + wind/AC strategies for real homes and offices
- Redirect vents away from your face (home, car, office).
- Use wraparound sunglasses outside on windy days.
- If air is very dry, a humidifier may help comfort—especially overnight.
Show me the nerdy details
A stable tear film depends on an adequate aqueous layer plus a functional lipid layer to slow evaporation. Screen use reduces blink frequency and completeness for many people, increasing evaporation. Environmental humidity and airflow changes can produce outsized symptom swings even when diet is consistent.
Personal note: I used to blame “bad eye days” on random biology. Then I noticed a pattern: airports, hotel AC, and long screen sessions were basically a dryness triathlon. (If you wake up with irritation that feels “sleep-related,” it’s also worth checking whether CPAP mask leak into the eyes is quietly drying your surface overnight.)
10) The 14-day reset (and the reintroduction protocol competitors don’t give)
This is where everything becomes testable. A reset isn’t punishment—it’s a short experiment to identify what’s actually driving your flares. The goal is not to live like a monk. The goal is to get your comfort predictable.
How to track (3 signals, once daily)
- Comfort score (0–10): overall dryness/irritation.
- Screen tolerance: how long you can work before discomfort spikes.
- Morning dryness: how your eyes feel in the first 30 minutes after waking.
Days 1–3: stabilize hydration + remove top triggers
- Use the midday pale-yellow checkpoint.
- Remove alcohol completely for 3 days.
- Avoid the saltiest restaurant meals and ultra-processed snacks.
Days 4–10: omega-3 rhythm + plate formula
- Lock two omega-3 meals into your week.
- Run the plate formula daily (protein + color + fat + fiber).
- Keep caffeine steady (don’t add chaos while you’re trying to learn).
Days 11–14: reintroduce one trigger at a time
This is the part competitors rarely give you: reintroduce one variable, then watch the next day.
- Day 11: reintroduce caffeine timing change (e.g., second coffee) OR keep the same—don’t stack changes.
- Day 12: reintroduce one restaurant meal (choose a controlled situation).
- Day 13: if you drink, reintroduce a small amount of alcohol (optional; skip if you’re flaring).
- Day 14: return to baseline and compare your 3 signals.
- Stabilize first (hydration + fewer triggers).
- Build the omega-3 rhythm you can keep.
- Reintroduce one variable at a time to learn what matters for you.
Apply in 60 seconds: Create a note called “LASIK Dry Eye Log” with three daily lines: comfort, screen tolerance, morning dryness.
Mini calculator: your midday hydration check (inputs ≤3)
Midday Hydration Check (no math obsession—just a quick decision)
- Is your urine pale-yellow by midday? Yes/No
- Do you feel noticeably thirsty? Yes/No
- Any mild headache or dry mouth? Yes/No
Output: If you answered “No” to #1 or “Yes” to two of the three signals, increase water earlier in the day and pair it with meals. If signals are fine, maintain—don’t overcorrect late at night.
Neutral action: Use this check once daily for 7 days, then adjust your routine.
11) Next step (one concrete action)
If you try to change everything today, you’ll change nothing by Friday. So here’s your one move—small enough to do, strong enough to matter.
Do this today (10 minutes)
- Schedule one omega-3 meal for the next 48 hours (buy it today if needed).
- Run the midday hydration check and write the result in a note.
Do this tomorrow (5 minutes)
- Remove one trigger (alcohol OR a salty restaurant meal OR ultra-processed snacks).
- Log your comfort score at the same time you logged it today.
Eligibility checklist (binary yes/no + next step)
Can you run the 14-day reset?
- Can you track 3 signals once daily for 14 days? Yes/No
- Can you keep alcohol out for 3 days? Yes/No
- Can you pick 2 omega-3 meals this week? Yes/No
- Do you have any red-flag symptoms (pain, discharge, sudden vision change)? Yes/No
Next step: If you answered “Yes” to the first three and “No” to red flags, run the plan. If red flags are “Yes,” contact your eye care professional first.
Neutral action: Print or copy this checklist into your notes and review it before you start.
Decision card: when A vs B (time/cost trade-off)
Food-first vs supplement-first
A) Choose food-first if you want low risk, fewer side effects, and clearer tracking (usually best starting point).
B) Consider supplements if you can’t meet food intake, your clinician agrees, and you can keep it consistent.
Neutral action: Pick A or B for the next 14 days and don’t mix strategies mid-experiment.

FAQ
1) How long does dry eye last after LASIK?
Many people improve over time, but the timeline can vary widely. If symptoms are severe, worsening, or disrupting daily life beyond what your surgeon described as expected, it’s worth checking in—especially if you notice pain, discharge, strong light sensitivity, or sudden vision changes.
2) When can I start omega-3 after LASIK?
Follow your surgeon’s post-op plan first. If you want omega-3 support, a food-first approach (like two fish meals per week) is often the simplest starting point. For supplements, ask your surgeon/clinician—especially if you have bleeding risk, are on blood thinners, or have post-op restrictions.
3) Fish oil vs flaxseed vs algae—what’s best for dry eye?
People choose based on diet preference and tolerability. Fish provides EPA/DHA directly; flaxseed provides ALA (which the body partially converts), and algae can provide DHA/EPA as a fish-free option. The “best” choice is the one you can do consistently and safely for your situation—ideally with clinician guidance if supplementing.
4) Does drinking more water help dry eye or is it a myth?
Hydration can influence comfort, but it’s not the only factor. If your issue is mainly evaporation (screens, wind, AC), water alone won’t fix it. A steady hydration rhythm plus environmental fixes (airflow, blinking habits) tends to be more effective than nighttime water overcorrection.
5) How much caffeine is too much for post-LASIK dry eye?
There’s no single number that fits everyone. The bigger issue is timing and spikes: large caffeine doses with little water can trigger an afternoon crash that feels like dryness. Try pairing each caffeinated drink with a full glass of water and keeping intake steady while you run the 14-day experiment.
6) Can alcohol slow recovery or worsen dryness the next day?
Alcohol can worsen dehydration risk and disrupt sleep, both of which can amplify dryness symptoms the next day. If you’re flaring, treat alcohol as a variable: remove it for 3 days, then reintroduce cautiously and observe.
7) Are electrolyte drinks good for dry eyes?
They can help in heat, heavy sweat, or illness. But for typical office days, many electrolyte drinks add extra sodium (and sometimes sugar), which can backfire if salty foods trigger your dryness. Water paired with meals is a safer default unless you have a clear reason for electrolytes.
8) What foods trigger dry eye flare-ups within 24 hours?
Many people notice flare patterns after high-sodium restaurant meals, alcohol, and ultra-processed/high-sugar foods—often through dehydration, sleep disruption, and inflammatory load. The 14-day reset helps you identify your personal triggers rather than guessing.
9) What supplements should I avoid right after LASIK?
Don’t add new supplements without checking your surgeon’s guidance, especially if you’re on blood thinners or have bleeding risk. If you do supplement, avoid stacking multiple “eye blends” at once—keep variables minimal so you can track what helps and what harms.
10) When should I call my eye doctor about dryness?
Call promptly for increasing pain, strong light sensitivity, discharge/fever, or sudden vision changes. Also reach out if symptoms remain severe, don’t improve as expected, or interfere with daily function despite basic measures.
Conclusion
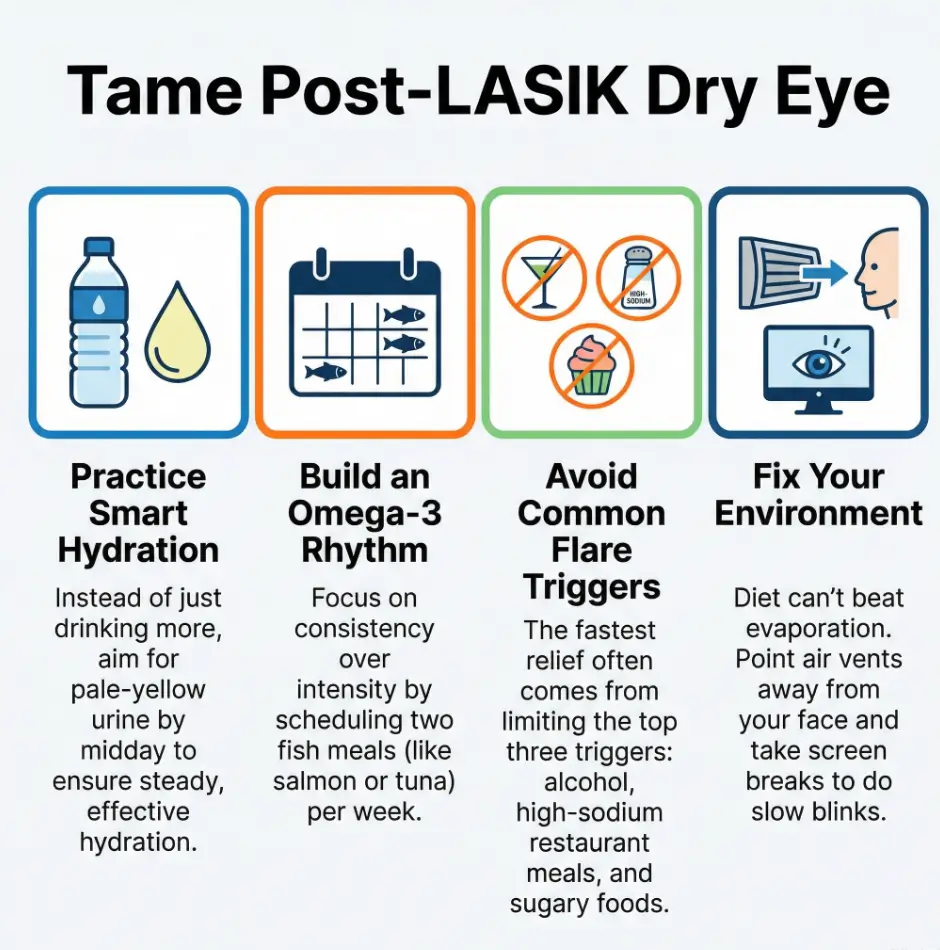
Remember the daily routine that cancels “healthy eating” without you noticing? It’s this trio: screens + airflow + sleep debt. You can eat the world’s most virtuous lunch and still lose the comfort battle if your eyes are evaporating under a vent while your blink rate disappears.
The good news is wonderfully unromantic: when you stabilize hydration earlier in the day, build a boring omega-3 rhythm, and remove the biggest flare triggers, your symptoms often become less mysterious. Not perfect—just predictable. And predictability is where relief begins.
Infographic: The 3-Lever Comfort System (Post-LASIK Dry Eye)
1) Hydration Rhythm
Midday pale-yellow check + water with meals + avoid late-night overcorrection.
Goal: steady, not extreme.
2) Omega-3 Consistency
Two fish meals/week (repeatable) or clinician-approved supplement with meals.
Goal: boring and sustainable.
3) Trigger Control
Alcohol, restaurant sodium, ultra-processed sugar spikes—reintroduce one at a time.
Goal: fewer “mystery” flare-ups.
If you want a next step you can finish within 15 minutes: open your calendar, choose your two omega-3 meals for the week, and start the “3-signal” log today. Tomorrow, remove one trigger and compare. That’s it. Small levers, repeated. (If seasonal allergies are part of your story, it can also be worth checking whether your “non-drowsy” pill is quietly drying you out—see Claritin vs Zyrtec vs Allegra for dry eye to spot common patterns.)
Last reviewed: 2025-12-23

