
Predictable Nights: Low-Vision Bedside Logic
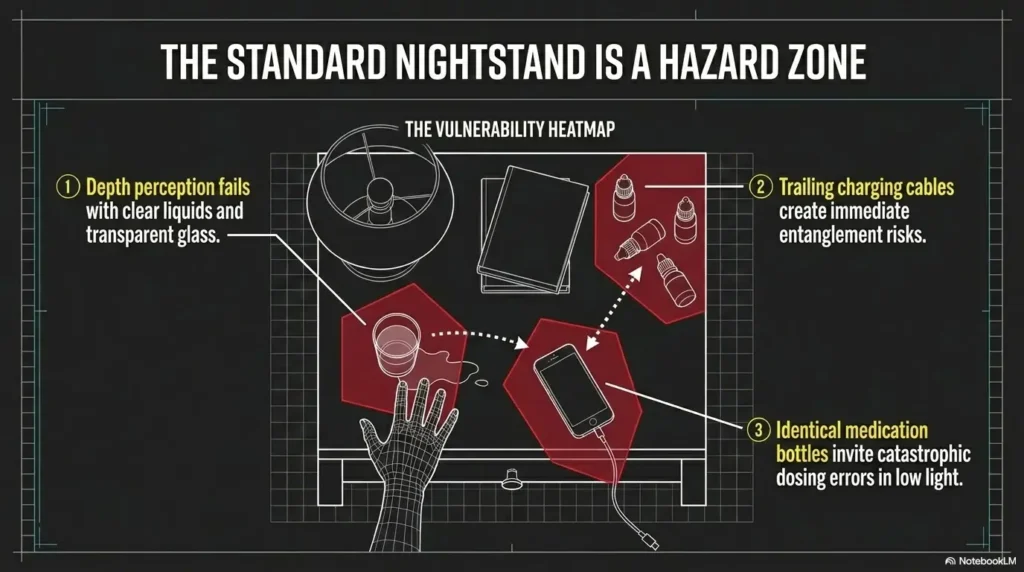
At 2 a.m., a nightstand can turn into a tiny obstacle course: the wrong bottle under your fingers, a charging cable snagging your wrist, or water suddenly one careless nudge away from your phone. A bedside organization system for low vision is about making the room behave better when your eyes are tired and your brain is still surfacing from sleep.
Most setups follow “daylight logic,” which fails during nighttime fatigue and glare. A truly effective layout prioritizes touch, position, and repetition over décor trends, reducing friction and the risk of sleepy mistakes.
Once the layout starts working by feel, the whole room gets quieter.
Table of Contents
Fast Answer: A good bedside organization system for low vision keeps the most-used items in fixed, touch-friendly zones so nighttime tasks require less searching, less reaching, and fewer risky guesses. The goal is not making the nightstand look tidy. It is making glasses, eye drops, phone, and water easy to find by habit, texture, and position, even when vision is limited, lighting is low, and you are half awake.

Start With Reach, Not Decor: What a Bedside System Actually Needs to Do
A bedside setup for low vision should reduce searching, not just reduce clutter
A tidy bedside table can still be a terrible bedside system. A clean-looking surface often photographs well and functions badly. One glossy tray, one decorative lamp base, one cup holding six unrelated objects, and suddenly the whole setup behaves like a silent prank. For low vision, the real question is not “Does this look organized?” but “Can I find the right thing on the first reach with low light and low patience?”
I learned this the annoying way years ago while staying in a room with a beautifully styled nightstand. The lamp was lovely. The coaster was tasteful. The water glass sat next to my phone like a small domestic still life. At 3 a.m., it became a slapstick scene without the soundtrack. My hand found the cord, then the glass, then regret. That is when the philosophy changed for me: bedside organization is not décor with morals. It is functional choreography.
A better setup reduces three specific frictions: search time, reach complexity, and error risk. If your hand has to move across several objects before it reaches your glasses, the system is already asking too much. If your eye drops live beside lip balm, hand cream, and vitamins, the system is too socially optimistic about sleepy decision-making. If your phone must be unplugged, lifted, rotated, and rescued from a cable nest before you can use it, the layout is not helping you. It is issuing tiny invoices all night long.
- Search time: How long it takes to identify the item
- Reach path: How many objects the hand crosses on the way
- Reset ease: How easy it is to return the item to the same place
- Error risk: How easy it is to grab the wrong thing
The safest layout begins with the first five seconds after waking or reaching in the dark
The first five seconds matter because they are ruled by instinct, not polished reasoning. You are not a calm systems engineer at 2:14 a.m. You are a person with dry eyes, uneven balance, and the motor finesse of a mildly confused raccoon. So the layout must serve that version of you. The first touch should orient you. The second should confirm. The third should deliver the object.
This means the highest-priority items belong inside the easiest reach arc. For many people, that is a shallow semi-circle beside the dominant hand, within one forearm’s reach, with no need to lean or twist. The American Academy of Ophthalmology and the National Eye Institute both emphasize practical adaptations and environmental support for people managing vision limits. In everyday life, that translates to something humbler than most people expect: stable routines, predictable object placement, and fewer visual surprises.
Why “pretty but movable” often fails when the room is dim and the brain is foggy
A movable basket, a decorative tray you slide around for cleaning, a cup you sometimes use for earbuds and sometimes for drops, a charger that lives “wherever it lands” can all feel harmless in daylight. But low-light success depends on consistency. The best bedside system is a little boring in the most useful way. It repeats itself. It resists improvisation. It teaches your hand the room.
- Reduce search time first
- Keep the reach path clear
- Make every item return to one fixed home
Apply in 60 seconds: Sit on the bed, close your eyes, and test whether your hand can find the most important item without touching anything else.
Fix the Four Essentials First: Glasses, Drops, Phone, and Water Need Different Rules
Glasses need a stable landing zone that protects lenses and rewards muscle memory
Glasses are not just another bedside object. They are often the bridge between confusion and competence the moment you wake. Treating them like loose jewelry is how they end up under a tissue, half on a book, or teetering at the edge of the table like a tiny expensive dare. A proper landing zone should be flat, non-slip, and visually or tactically distinct from everything else on the surface.
A shallow tray with a soft liner works well. So does a dedicated mat with a raised edge. What usually fails is a narrow stand that requires precise placement in low light. A stand can be elegant, but if it asks sleepy hands to perform a small parking maneuver, it becomes one more thing to miss. For many people with low vision, a broad landing pad beats a narrow target every time.
Eye drops need upright storage, easy identification, and zero confusion with other bottles
Eye drops deserve their own rules because a bottle mistake at the bedside is not a funny inconvenience. It is a real safety issue. Drops should be stored upright whenever the product instructions support that, separated from cosmetics, supplements, and any other similarly sized containers. If two bottles feel too similar, that is your signal to change the system, not trust your memory.
One simple fix is tactile differentiation. Use a small silicone ring around one bottle, a textured pouch for another, or a shallow container that holds only drops and nothing else. Do not create a tiny bottle neighborhood and expect your fingers to negotiate zoning law in the dark. The FDA and major eye-care providers regularly remind patients to follow product labeling and use medicines correctly. At the bedside, good organization becomes part of that correctness, much like the tactile strategies used in pill bottle label placement for low vision or a broader low-vision medication management routine.
Phones need predictable placement without creating cable chaos or swipe-and-drop risk
A phone at night is alarm clock, flashlight, magnifier, emergency contact device, and sometimes the place where you check the time and accidentally learn something upsetting about the news. It needs a home that is reachable but protected. The ideal placement keeps it from sliding, hides excess cable length, and does not force your hand across water or medicine.
I prefer a phone zone with one rule: the charger arrives from behind or along the far side, never across the front edge where the hand enters. Front-edge cables are ankle-level rake handles for the wrist. A phone stand can help if it is low and stable. Tall flimsy stands tend to become catapults. Even without a stand, a non-slip mat plus a cable clip can tame most bedside phone drama. If your phone also doubles as a visual aid, settings like Back Tap for Magnifier can make that reach even more useful without adding another device to the table.
Water needs spill-aware positioning that stays reachable without crossing over other items
Water is the bedside peacemaker until it is the bedside saboteur. A glass placed beside electronics or medication creates a zone of mutual suspicion. A better setup gives water its own stable footprint, preferably in a bottle or lidded tumbler with a wide base. The point is not paranoia. The point is reducing the cost of one drowsy bump.
Think in lanes. If your hand must reach across the phone to grab water, the system is asking for trouble. Water belongs in a position that can be reached directly and returned directly, with no crossing over the glasses zone or the medicine zone. Once you see the nightstand as traffic design, the mistakes become easier to spot.
Decision Card: Open glass vs lidded bottle
Choose an open glass if you have excellent hand control at night, plenty of surface space, and no electronics or drops nearby.
Choose a lidded bottle or tumbler if you wake often, reach quickly, share the surface with a phone or medication, or have had even one recent spill.
Neutral next step: Test both with the room dim and keep the version that requires fewer correcting movements.
Zone the Surface Like a Map: One Bedside Table Should Not Behave Like One Big Pile
Create left-right or front-back zones so each item category has a permanent home
A nightstand should behave more like a map than a basket. Maps reduce uncertainty by assigning meaning to position. One area is for glasses. One is for drops. One is for phone. One is for water. Once you do this, your hand stops conducting random searches and starts navigating known territory.
The exact map depends on your body and sleep habits. If you sleep on your right side and reach with your right hand, the front-right zone usually becomes premium space. If you reach across your body, your layout may need to favor front-center access. The point is not copying someone else’s diagram. It is designing around your real reach path, not the imaginary orderly person you become only while shopping.
Use tactile boundaries, trays, mats, or shallow containers to separate objects by feel
Boundaries matter because a bare tabletop turns every object into part of one big country. A shallow tray, a felt pad, a silicone mat, or a small open bin gives each item an address you can feel. That feeling is doing more cognitive work than most people realize. It tells the hand: this is the glasses zone, this is the bottle zone, this is where the phone stops moving.
Shallow is important. Deep containers create hidden layers and force digging. At the bedside, digging is just panic with a storage label. Keep containers open enough to allow direct touch and direct retrieval. If a container makes you pinch, fish, or rotate objects to identify them, it is not bedside-friendly.
A system works better when each item can be found without visual scanning
This is the quiet standard behind the whole setup. A person with low vision should not have to visually scan the nightstand to complete a routine task. Some nights vision is better. Some nights it is not. Dry eyes, fatigue, glare, medication, and stress all shift the experience. A touch-first setup respects that variability instead of arguing with it.
Here is a useful test: close your eyes or dim the room, then pick up each item and return it. If you hesitate on where to place it back, the zone is not distinct enough. A good system feels obvious even before it feels attractive.
Infographic: A Simple Bedside Map for Low Vision
Front Zone
Fastest-reach items only
Usually glasses or phone
Side Zone
Water with stable base
No cables crossing this lane
Protected Zone
Eye drops upright in a tactile holder
Keep separate from all other bottles
Back Edge
Cable routing, lamp base, low-priority items
Nothing that must be found half asleep
Rule: No object should require crossing over water, wires, or lookalike bottles to reach something more important.
Show me the nerdy details
Human factors design often works best when high-frequency tasks are given the shortest, clearest movement path. At the bedside, that means fewer object categories in the prime reach zone, strong tactile differentiation, and minimal need for visual confirmation. You are not optimizing storage density. You are optimizing retrieval accuracy under fatigue.
Don’t Stack the Night: Vertical Storage Can Make Low-Vision Access Worse
Tiered organizers, deep caddies, and narrow compartments can hide the thing you need most
There is a certain kind of organizer that looks like it was designed by someone who has never tried to find eye drops while half asleep. It has tiers, slots, cups, and hopeful little partitions. It promises control and delivers archaeology. Vertical storage often fails because it hides items behind other items, creates shadow, and makes touch less reliable. What looks efficient by day becomes guesswork by night.
Depth is the usual villain. When the hand cannot immediately identify what is inside a compartment, the search turns into rummaging. For low vision, rummaging increases both frustration and error. And the thing with nighttime frustration is that it rarely stays small. One missed bottle becomes a bright light switch, then a fully awake body, then a night that feels broken over something that should have been simple.
The best bedside storage is often shallow, open, and easy to reset by touch
Shallow storage feels almost humble compared with elaborate organizers, but humility has excellent bedside manners. A low tray, an open-front bin, or a single-level caddy lets the fingers identify objects without moving them much. It also makes resetting easier. Resetting matters more than most buying guides admit, because nighttime systems live or die by whether they recover cleanly after use.
One night in a hotel, I placed my glasses in a deep woven basket because it was “the obvious storage spot.” In the morning, they had migrated into towel-company retirement. I found them only after patting through tissues, a remote, and a tiny tourism pamphlet. Since then I have had strong feelings about bedside baskets, and none of them are poetic.
Here’s what no one tells you… the “space-saving” organizer can become a fumbling machine at 2 a.m.
Space-saving products are not automatically task-saving products. In tight spaces, people often reach for more compartments when they really need fewer decisions. The better question is: does this organizer help me identify, grasp, use, and return the item with one simple motion pattern? If not, it is saving inches and costing peace.
- Hidden items increase fumbling
- Open access improves tactile finding
- Easy reset keeps the system from drifting
Apply in 60 seconds: Remove one deep container from the nightstand and replace it with a flat tray or mat.
Make Touch Do the Work: Texture Beats Guessing in the Dark
Different materials can help distinguish glasses space from drops space from phone space
Texture is one of the smartest tools in a low-vision bedside setup because it quietly hands part of the job from the eyes to the fingers. A felt mat feels different from silicone. A ridged tray feels different from smooth wood. A fabric pouch feels different from a plastic stand. These differences become a tactile language, and the body learns that language faster than many people expect.
You do not need an elaborate coding scheme. In fact, too many textures can become their own kind of noise. Two or three clearly different surfaces are enough. For example, glasses on felt, phone on silicone, drops in a lightly textured cup. The point is immediate distinction, not sensory maximalism. Your nightstand is a bedside helper, not an escape room.
Non-slip mats, raised edges, and tactile markers reduce hand-searching and accidental knocks
A non-slip mat does two useful things: it prevents drift, and it confirms location. Raised edges add another layer of confidence because they tell the hand where the zone begins and ends. Small tactile markers can also help, especially if you need to distinguish one container from another. A raised dot, a strip of textured tape, or a rubber band placed with intention can make the right object easier to identify without overcomplicating the layout.
People sometimes resist these small modifications because they fear the setup will look less elegant. That concern makes sense. But bedside safety has a way of making elegance answerable to reality. A system that feels slightly less polished and works every night is better than a polished one that keeps creating little failures. The same logic shows up in other touch-first systems, from a low-vision key identification setup to tactile labels that keep similar bottles from getting mixed up.
Why identical containers create more errors than a slightly imperfect-looking setup
Matching containers are satisfying in catalogs because uniformity looks calm. At night, uniformity can become a trick mirror. If every small container feels the same, you have stripped away valuable sensory information. A slightly mismatched setup often performs better because each object has its own tactile identity. Beauty is not banned here. It just has to make peace with function.
Eligibility Checklist: Is your bedside setup touch-friendly yet?
- Yes / No: Can you identify the glasses area by touch alone?
- Yes / No: Do drops feel physically different from other bottles nearby?
- Yes / No: Does the phone stay in place when you brush the cable?
- Yes / No: Can you reach water without crossing another object zone?
Neutral next step: Any “No” answer marks the first thing to fix tonight.
Light the Task, Not the Whole Room: Night Visibility Without the Glare Trap
Low-level warm lighting can support orientation without blasting tired eyes awake
Lighting for low vision at the bedside is a balancing act. Too little light, and everything becomes guesswork. Too much, and the room turns hostile. The best lighting usually supports the task rather than flooding the whole space. A low-level warm light aimed at the table edge, tray, or floor path often works better than a bright exposed bulb. The purpose is orientation, not interrogation.
Warm light is often more tolerable at night, though the exact preference varies by person and condition. What matters most is not a trendy color temperature number but glare control, bulb shielding, and placement. Even a helpful lamp can feel awful if the bare bulb hits the eye directly. A kind lamp with bad manners is still bad company. If you are sorting out bedside comfort, it may help to compare 2700K vs 3000K lighting for glare-sensitive eyes or the practical tradeoffs in Reduce White Point vs Night Shift when your phone is part of the nighttime routine.
Motion lights and under-table glow can help when the switch itself is hard to find
Motion-activated or touch-activated lights can reduce the awkwardness of locating a switch in the dark. Under-table strip lights or subtle puck lights aimed downward are especially helpful because they define edges without shining directly into the eyes. For some people, this small pool of light does more good than an overhead light ever could.
The National Eye Institute often stresses that lighting needs vary widely for people with low vision. That is the practical truth worth remembering. The “best” light is not universal. It is the one that makes your specific bedside task easier without causing glare, reflection, or full-body wakefulness. Test at the hour you actually use it. Daytime approval means very little here.
Avoid reflective surfaces and exposed bulbs that turn one glance into a flare storm
Reflective lamp bases, glossy trays, glass tabletops, and shiny accessories can turn a little light into a lot of visual chaos. If you already deal with glare sensitivity, these surfaces are not decorative details. They are functional obstacles. The same goes for bulbs visible from the pillow position. If you can see the source directly, you may be building discomfort into the design.
One of the quiet upgrades I recommend most often is matte over shiny. Matte finishes, shaded bulbs, and directed light create a softer visual field. The difference can feel surprisingly large, especially when the room is otherwise dark. That same principle is why articles on matte vs glossy paint for glare control and bathroom mirror glare end up sounding less like décor advice and more like peace treaties for tired eyes.
Mini Calculator: How many steps does your night routine take?
Count the motions needed to find, use, and return your glasses, drops, phone, and water.
If one item takes more than 3 motions or requires crossing another item’s lane, that zone probably needs redesign.
Neutral next step: Reduce one task by just one motion and retest tonight.
Who This Is For, and Who It Is Not
This is for people with low vision who need safer, repeatable access to bedside essentials
This guidance is for readers who are not looking for a Pinterest-perfect nightstand. It is for people who want the room to behave better at night. If you rely on glasses immediately after waking, use drops during the night or early morning, need a phone for alarms or magnification, or want water within easy reach without adding risk, this setup is for you.
It is also for readers whose vision fluctuates. Some nights are sharper. Some nights are foggier. Some mornings begin with dry eyes, glare sensitivity, or delayed focus. A good bedside system absorbs that variation instead of punishing it. You should not need perfect vision to use the things that help you function. If mornings have begun with more than ordinary haze, you may also want to read about waking up with blurry vision so the room is not forced to explain what may be a bigger change.
This is for caregivers and family members trying to reduce nighttime confusion and spills
If you are setting up a room for a parent, partner, or family member, the goal is not to over-manage the space. It is to make the most common nighttime tasks simpler and safer. Many caregivers understandably buy organizers first. But the purchase is not the plan. The plan is reducing confusion, keeping important items distinct, and making the room easier to navigate half awake.
Caregivers also bring one important advantage: they can observe the actual reach pattern from the outside. Sometimes the person using the nightstand has adapted around a bad setup for so long that the awkwardness feels normal. A fresh pair of eyes can spot the silly things immediately. Why is the water behind the charger? Why are two nearly identical bottles touching? Why is the lamp switch hiding like it owes money? If you are supporting someone more broadly, the same gentle logic appears in helping a spouse with vision loss and other small-environment adjustments that reduce friction without making the room feel overmanaged.
This is not a substitute for medical advice when vision changes suddenly or medication use becomes uncertain
If nighttime access keeps getting harder because vision has changed suddenly, if medication is being mixed up, or if there are repeated near-falls or wrong-bottle moments, organization alone may not be enough. The room matters, but so do medical review, medication counseling, and low-vision support. The American Foundation for the Blind, ophthalmology clinics, and rehabilitation services often emphasize that environmental changes and professional guidance work best together, not as rivals.
In other words, a better nightstand can do a lot. It just should not be forced to solve everything.
Common Mistakes: The Nightstand Errors That Quietly Create Stress
Keeping “important things nearby” without assigning each one a fixed location
This is one of the most common mistakes because it feels responsible. Everything important is nearby. Excellent. Except “nearby” is not a location. Nearby is a mood. Nearby becomes anywhere on the table, which means nowhere reliable when you need it most. Fixed location matters because memory loves repetition and hates improvisation.
I once watched someone keep their glasses “right here” every night, by which they meant somewhere within a hand-span of a lamp, a book, a tissue box, and a phone charger. They were not disorganized in life. They were simply trusting a sleepy brain to perform precision recall without landmarks. That is a difficult job description for anyone.
Using lookalike bottles, dark containers, or unlabeled accessories that feel the same by hand
Objects that look different in daylight can feel identical at night. Dark containers can also vanish visually against a dark tabletop. If two items share size, shape, or texture, the system needs more contrast. Tactile markers, lighter surfaces, and dedicated containers reduce the chance of wrong-item grabs. A low-vision setup should never rely on thin visual differences alone. The same problem shows up when trying to read medicine leaflets with low vision or sort similar packaging without a clear labeling method.
Letting charging cables snake across the reach path where hands and water already compete
Cables are bedside opportunists. Left unmanaged, they drift into the most inconvenient lane and claim it as if by ancient right. A cable across the front edge or between water and phone creates a two-part hazard: snagging and repositioning. Once the cable moves, everything else moves with it. Now the map has changed, and your hand is working from yesterday’s memory.
Let’s be honest… most bedside chaos begins with convenience decisions that worked only in daylight
That lamp looked fine at noon. The open glass seemed sensible after dinner. The extra bottle was “just temporary.” The charging block could “sit there for now.” Bedside clutter rarely arrives as rebellion. It arrives as a series of small reasonable choices made under daylight assumptions. Night exposes the flaws like a stern editor.
- “Nearby” is not a usable address
- Lookalike items increase wrong grabs
- Cables should never cross the prime reach lane
Apply in 60 seconds: Label one exact home for each essential and remove one lookalike item from the nightstand.
Don’t Put Safety Behind Convenience: Some Easy Choices Age Badly Fast
A full glass without a stable base can become a spill source near electronics and medication
Convenience is persuasive because it whispers. Just set the glass here. Just keep the drops beside the lotion. Just run the cable this way for tonight. But at the bedside, easy choices age quickly. What feels convenient in the evening may become fragile by midnight. Water near electronics, open containers near medicine, and unstable objects near the front edge all carry more cost than their daytime innocence suggests.
A wide-base bottle or tumbler with a lid often solves several problems at once. It reduces spill risk, tolerates clumsy reaches better, and can usually be identified by shape more easily than a low glass. This is not about wrapping life in bubble wrap. It is about making ordinary mistakes less expensive.
Keeping drops, supplements, and cosmetics together can turn a sleepy reach into a wrong-bottle moment
Mixed-use bedside storage is one of those ideas that sounds efficient until you examine it under fatigue. Products with similar packaging should not coexist in one sleepy grab zone. If a bottle is important enough to use near the bed, it is important enough to give a distinct tactile identity and a protected location. One zone, one purpose. That simple rule prevents many preventable mix-ups.
The closest spot is not always the safest spot if it forces crossing over other objects
People often assume the safest place is simply the nearest place. But the nearest spot can still be wrong if it forces the hand over water, cords, or lookalike containers. Safety is about the path as much as the distance. A slightly farther item in a clean lane is often safer than a closer item in a crowded one. The same principle sits underneath broader fall-prevention at home for aging vision and even low-vision nighttime bathroom safety: the path matters as much as the object.
Quote-Prep List: What to gather before buying a bedside organizer
- Measure table width and depth
- List the 4 items used most often at night
- Note whether each item needs upright storage
- Count cables that must remain plugged in
- Test dominant-hand reach from your actual sleeping position
Neutral next step: Buy storage only after you know the table, the tasks, and the reach path.
Build for the Half-Awake Version of You: Morning Logic and Night Logic Are Not the Same
The best system still works when hands are slow, eyes are dry, and attention is thin
This may be the single most important design principle in the whole article. Build for the half-awake version of you. Not the efficient afternoon version. Not the optimistic online-shopping version. The half-awake version. The one with dry eyes, fuzzy depth judgment, and a suspicious relationship with fine motor skills. If the system works for that person, it will usually work for everyone else you become during the day.
A bedside routine should ask for recognition, not reasoning. You should not have to remember which identical pouch holds what. You should not have to think about whether the glasses are on the tray or behind the lamp or inside the book you forgot was there. The system should reduce choices until the right action is simply the easiest action.
Reduce the number of motions needed to find, pick up, use, and return each item
Count motions, not intentions. A useful system can often cut one or two movements from each task, and that difference matters more than it sounds. Fewer movements mean fewer chances to knock, spill, misplace, or fully wake yourself into irritation. If your phone can be lifted and docked with one clean motion instead of a cable untangle saga, that is a real improvement. If your drops can be found and returned without rotating the bottle to verify it, that is a meaningful gain.
A good bedside layout should feel obvious even before the brain is fully online
Obviousness is a design achievement. It does not happen by accident. It comes from fixed positions, clean lanes, tactile cues, and ruthless item editing. The bedside does not need twenty useful things. It needs four or five truly necessary ones behaving predictably. Everything else should earn its place or leave.
Short Story: A friend once told me her bedside table always looked “organized enough” before bed, yet every morning began with an absurd scavenger hunt. Glasses under the edge of a book. Phone half off the charger. Drops somewhere behind a lamp shaped like a ceramic pear. We changed nothing fancy.
We gave the glasses a felt square, the phone a silicone mat and one cable clip, the drops a textured holder, and the water a lidded bottle at the far side. That was all. The next week she laughed and said the table had become “weirdly obedient.” I loved that phrase because it captured the goal exactly. Not beauty. Not perfection. Just a small obedient system that stopped making mornings harder than they already were.
Show me the nerdy details
Under fatigue, error rates rise when tasks depend on discrimination among similar objects, variable placement, or multi-step reach paths. Bedside design improves when it reduces item similarity, reach crossings, and return ambiguity. This is less about décor than about cognitive load management in a dim environment.
Small Bedroom, Big Difference: Low-Vision Bedside Systems for Tight Spaces
Wall pockets, clip-on trays, and bed rails can help when table space is limited
Small bedrooms change the math but not the principles. If the bedside table is narrow, use nearby vertical support only where it does not hide priority items. A clip-on tray, a slim wall pocket for low-priority items, or a bed rail with a small attached shelf can expand function without crowding the top surface. The trick is to reserve the easiest access zone for the truly essential items only.
One caution: small-space solutions should not reintroduce the deep-pocket problem in another form. A fabric organizer hanging by the bed can be useful for tissues, a notebook, or a sleep mask, but less useful for glasses or drops if the pocket shape swallows them. Small spaces reward discipline. They do not forgive casual accumulation.
In very small rooms, reducing item count may matter more than buying a better organizer
This is the tough-love part. Sometimes the best organizer is subtraction. If the surface is tiny, every extra object taxes the system. Books, hand cream, receipts, pens, remotes, decorative objects, and tomorrow’s intentions all compete with the items that matter at 2 a.m. Remove enough clutter and the room suddenly feels as if it has grown a few inches. It has not. Your decisions just got cleaner.
Why narrow spaces need clearer priority rules, not just smaller containers
Smaller containers are not a strategy by themselves. Priority is the strategy. Ask one blunt question: what must be reachable without thought? Those items get the prime zone. Everything else either moves back, moves away, or earns a different home entirely. Tiny rooms can still have excellent bedside systems if they stop trying to host every object with sentimental ambition.
Coverage Tier Map: How “complete” does your bedside system need to be?
Tier 1: Glasses only
Tier 2: Glasses + phone
Tier 3: Glasses + phone + water
Tier 4: Add drops or one medication-related task
Tier 5: Full low-vision night routine with lighting, cable control, and tactile zoning
Neutral next step: Start at the tier that matches your real nightly routine instead of buying for a fantasy version of it.
FAQ
Where should glasses go on a bedside table for low vision?
Glasses should go in a fixed, easy-to-reach zone with a non-slip or soft base, usually at the front or dominant-hand side of the bedside surface. Avoid narrow stands that require precise placement unless they truly work for your hands at night. A broad landing zone is usually easier to use half awake.
How can I keep eye drops easy to identify at night?
Keep drops in their own dedicated holder, separate from all other bottles. Add a tactile cue such as a textured band, a small raised marker, or a container with a clearly different feel. If two bottles feel similar by hand, the system is not distinct enough yet.
Is it safer to keep water with a lid next to the bed?
For many people, yes. A lidded bottle or tumbler with a stable base often reduces spill risk, especially if the bedside surface also holds a phone, glasses, or drops. An open glass can work in some setups, but it is less forgiving of sleepy bumps and crowded surfaces.
What kind of bedside light works best for low vision without too much glare?
A low-level, warm, directed light usually works better than a bright exposed bulb. Lights aimed downward or toward the task area can help define edges without blasting the eyes. Matte finishes and shaded bulbs also help reduce glare and reflections.
Should a phone charger stay plugged in on the nightstand?
Usually yes, but the cable should be controlled. Use a cable clip or routing path that keeps the cord away from the prime reach lane and away from water. The goal is for the phone to be easy to dock and lift without creating a snagging hazard.
Are bedside caddies better than a standard nightstand for low vision?
They can be, but only if they are shallow, open, and easy to use by touch. Deep fabric pockets and narrow compartments can hide objects and make retrieval harder. A standard nightstand with strong zoning often works better than a more complicated caddy.
How do I organize a bedside setup if I sleep on one side but reach across with the other hand?
Design the layout around the hand that actually performs the task, not the side of the bed alone. Test from your real sleeping position and place the most-used item in the path that requires the fewest motions and the least crossing over other objects.
What should never be stored together on a low-vision nightstand?
Try not to store eye drops with cosmetics, supplements, or other similarly shaped bottles. Also avoid placing water immediately beside electronics or letting cables run through the same lane as the hand path. Mixed-use zones tend to create mistakes.

Next Step: Fix One Reach Tonight, Not the Whole Bedroom at Once
Put glasses, drops, phone, and water into four permanent zones tonight and test whether each one can be found with the room lights low and your eyes half closed
If the whole article has been whispering one thing, it is this: do not try to renovate the entire bedroom in one burst of noble energy. Fix one reach tonight. Then another tomorrow if needed. Give glasses a landing zone. Give drops a separate tactile home. Give the phone a safe cable path. Give water its own stable lane. Then dim the room and test the system honestly.
This is where many people finally close the loop from intention to proof. A bedside setup is not good because it sounds sensible. It is good because it works under real conditions. Test at night. Test sleepy. Test from the position you actually wake in. Tiny experiments beat grand plans here. In fifteen minutes, you can improve the first five seconds of your morning more than a week of scrolling product pages ever will. If you use your phone as part of that proof, even small tweaks like making an iPhone flashlight less harsh can help you test without turning the room into a tiny operating theater.
If the Setup Still Fails: Signs the Problem Is Bigger Than Organization
Repeated spills, missed medications, or difficulty identifying routine items may signal that the current lighting or vision support is no longer enough
If you have improved the layout and the problems keep repeating, pay attention. Repeated spills, trouble identifying routine items, frequent wrong reaches, or growing dependence on bright overhead light may suggest the issue is not just storage. It may be time to reassess lighting quality, bottle differentiation, medication counseling, or low-vision support strategies more broadly.
Some changes arrive quietly. The room seems harder. The nightstand seems more annoying. The morning routine takes longer. These are easy to blame on clutter alone, but sometimes they are gentle evidence that your needs have changed. There is dignity in noticing that early. There is wisdom in not forcing a tray to solve a larger problem.
When nighttime access keeps breaking down, it may be time to reassess lighting, labeling, or functional vision needs rather than just buying another organizer
Buying another organizer is emotionally appealing because it feels actionable. Sometimes it is useful. Sometimes it is merely decorative optimism in plastic form. If the same failure points keep returning, step back. Review the light source. Review bottle identification. Review whether the task itself has become harder. A more thoughtful adjustment often helps more than a more complicated product. Readers dealing with repeated changes may also find it useful to review warning signs of senior vision changes or consider whether a visit with a low vision specialist makes more sense than another organizer purchase.
The curiosity loop from the beginning closes here. The problem was never that your nightstand was not tidy enough. The problem was that nighttime asks different things of a room. It asks for predictability, tactile clarity, safer lanes, calmer light, and fewer decisions. Build that, and the night starts cooperating.
- Organize by task, not by looks
- Separate lookalike bottles and spill risks
- Test the setup in real nighttime conditions
Apply in 60 seconds: Choose the single most frustrating nighttime item and give it a permanent, touch-friendly home before bed tonight.
Last reviewed: 2026-04.

