
Best Home Setup for the First Week After Cataract Surgery: 7 Painful Mistakes I Made So You Don’t
I thought cataract recovery would be a peaceful week of naps and soft music. Spoiler alert: it was more like surviving a week-long obstacle course… blindfolded.
Somehow, I managed to turn my own home into a low-stakes survival game, where tripping over a slipper felt like a near-death experience and mastering eye drops became an Olympic sport in hand-eye coordination (emphasis on eye). What was supposed to be a “simple routine” turned into a daily improv performance—featuring me, a mirror, some questionable aim, and a lot of blinking.
If you’re short on time and just want a no-nonsense setup that keeps your eye safe, your stress levels down, and your wallet intact, this guide is your shortcut. I’ll walk you through a practical, room-by-room plan you can start setting up today—plus the seven avoidable mistakes that cost me comfort, sleep, and more money than I care to admit.
The goal? A calmer first week, fewer “I didn’t think of that” moments, and a recovery space that actually makes healing easier instead of harder.
Let’s turn your home into a healing zone—not a sitcom set.
Table of Contents
What the first week really feels like
The first week after cataract surgery is usually less Hollywood-drama and more “mildly annoying logistics.” Many people notice brighter colors, sharper edges, and a weird sense that the world just upgraded its contrast settings. You might also feel scratchiness, watering, mild light sensitivity, or that classic “Is something in my eye?” sensation. That’s common, but it’s also why your environment matters.
In my case, the most surprising part wasn’t pain—it was how quickly small inconveniences stacked into fatigue. A too-bright lamp, a missing bottle of drops, a low chair that required an Olympic-level stand-up maneuver. Each one stole 2–5 minutes. Multiply that by a day and you’ve lost 30 minutes to tiny frustrations.
Your home setup is basically a short-term recovery insurance policy for comfort and compliance. It reduces accidental rubbing, lowers fall risk, and makes it easier to follow your post-op plan even when you’re sleepy.
- Expect mild irritation and light sensitivity
- Plan for repeated drop schedules
- Remove tiny daily frictions
Apply in 60 seconds: Walk your main path and remove one trip hazard right now.

The 7 painful mistakes I made
I’m offering these with full, slightly embarrassed honesty. If you avoid even three, you’ll feel the difference by day 2.
- I didn’t create a “drop command center.” Result: I missed a dose and panicked for 20 minutes.
- I kept my lighting too harsh. It felt like living inside a refrigerator display case.
- I relied on memory for schedules. My brain, post-nap, was not a trustworthy administrator.
- I used a low couch. Standing up felt like a questionable CrossFit demo.
- I underestimated bathroom steam logic. I turned my shower into a fog machine.
- I left clutter on the floor. One near-stumble is enough to ruin your week.
- I bought the wrong “comfort extras.” The cheap pillow was a false economy.
Each mistake cost me either time, sleep, or out-of-pocket money. The fix is not complicated. It’s just deliberate.
The five-zone home setup
If you only have 30 minutes to prep, focus on these five zones. This is the shortest path to a safe, low-stress week.
- Pathway zone: bed ↔ bathroom ↔ kitchen, cleared and softly lit.
- Sleep zone: pillows or wedge arranged before you’re tired.
- Drop zone: one basket, one timer, one written schedule.
- Hygiene zone: towel, clean cloth, and instructions visible.
- Comfort zone: a supportive chair that doesn’t demand acrobatics.
I once set this up for a family member in 18 minutes. The secret? I treated it like packing for an overnight train: everything you need within arm’s reach, nothing that makes you bend, squint, or guess.
Show me the nerdy details
Small environment changes can improve adherence to multi-dose routines. One storage location plus one reminder system reduces missed-dose risk more than buying extra gadgets.
Sleep and positioning without regret
Sleep is where many people accidentally sabotage their best intentions. The goal is simple: protect your eye while keeping your neck and lower back from staging a rebellion.
A wedge pillow or a firm stack of two pillows can help keep your head slightly elevated. If you’re told to avoid sleeping on a specific side, place a pillow barrier behind you. It’s low-tech and surprisingly effective. The first night I skipped this, I woke up on the “wrong” side and spent the next hour doing the mental math of regret.
Decision card: If you already have back or shoulder pain, consider a wedge or a supportive recliner for 7–10 days. If you’re generally comfortable and your bed is supportive, a simple pillow setup can be enough. This is a time-and-comfort trade-off, not a moral test.
- When A (buy/borrow wedge): chronic neck/back pain, restless sleeper, strict positioning rules.
- When B (use existing pillows): stable sleeper, mild discomfort only, budget-tight week.
Save this decision and confirm any specific sleep-position rules with your surgeon’s written instructions.
- Prepare your pillow layout before surgery day
- Use a side barrier if needed
- Choose comfort over improvisation
Apply in 60 seconds: Place a “do-not-roll” pillow behind your back right now.
Eye drop station that actually works
This is the heart of the first week. You might have multiple drops, different frequencies, and a schedule that feels like it was designed by someone who has never had a nap in their life.
Build one small station near your main seat or bedside. Include:
- All prescribed drops
- Tissues and clean cotton pads
- A simple written schedule you can check at a glance
- A phone timer or smart speaker reminder
- Hand sanitizer or soap nearby
My early mistake was “distributing” drops like I was optimizing a warehouse. One bottle in the bathroom, one in the bedroom, one in the living room. I created a scavenger hunt for my own healing.
Quote-prep list: If you’re paying out of pocket for drops or protective eyewear, ask your pharmacy for the exact generic names, bottle sizes, and refill rules. In the U.S., this can save 10–20 minutes per call and prevent surprise refill denials. Ask for a written cost estimate if you’re comparing pharmacies.
Save this list and confirm your plan with your pharmacy’s current pricing and your insurer’s benefits portal.
Bathroom and hygiene: smoother and safer
Most post-op instructions emphasize keeping water, soap, and steam out of the eye early on. Your exact rules may vary, but your bathroom can be set up to support whatever your surgeon decides.
Quick wins:
- Place a clean washcloth and towel at eye level
- Use lukewarm water and avoid direct spray toward your face
- Reduce heavy steam by keeping the door slightly open if allowed
- Move slippery mats and add a non-slip option
I once took a “quick relaxing shower” on day 2 and got a face full of warm mist. Nothing catastrophic happened, but the anxiety tax was real. I learned to treat the bathroom like a controlled environment for a week, not a spa audition.
Show me the nerdy details
Steam and splashes raise the chance of accidental face and eye touching. The best prevention is not fear—it’s placing tools where your hands naturally reach.
Screens, reading, and lighting in 2025
Yes, you can probably use your phone. No, you shouldn’t pretend you’re immune to fatigue. Many people experience temporary glare or halos at night, and bright screens can feel more intense right after surgery.
My simple rule: short bursts, soft light, frequent breaks. I set my phone to larger text and reduced brightness. A warm bedside lamp with a shade beat overhead lighting by a mile. The first time I opened a high-contrast white screen in a dark room, my eye felt like it was judging me personally.
- Start with 5–10 minute reading blocks on day 1–2
- Gradually extend by 5 minutes as comfort allows
- Aim for 20–30 minutes of total screen breaks across the day
- Use larger text and softer brightness
- Prefer shaded lamps to overhead glare
- Take planned breaks before discomfort spikes
Apply in 60 seconds: Turn on large text and reduce your screen brightness right now.

Costs, supplies, and a 60-second out-of-pocket check
Even when the surgery itself is covered, the first week can bring add-on costs: drops, artificial tears, protective shields, a supportive pillow, or a ride you didn’t plan to book twice. The trick is to separate “nice-to-have” from “prevents a bad week.”
Common first-week items and rough U.S. price ranges in 2025:
| Item | Typical range (USD) | Notes |
|---|---|---|
| Protective eye shield | $5–$20 | Often included; confirm before buying |
| Artificial tears (preservative-free) | $10–$25 | Helpful for dryness; brand varies |
| Wedge pillow | $30–$80 | Borrowing can be a smart option |
| Extra sunglasses | $15–$60 | Useful for glare sensitivity outdoors |
Save this table and confirm the current item price on the manufacturer or retailer’s official page.
Mini calculator (inputs ≤3):
- Expected pharmacy copays for post-op drops
- Comfort items you plan to buy (pillow, tears, extra glasses)
- Transportation costs for 1–2 follow-ups if you won’t be driving right away
Your 7-day estimate: add those three numbers. If the total looks higher than expected, your fastest fixes are comparing pharmacy options, borrowing a wedge pillow, or skipping non-essential upgrades until week 2. Save this estimate and confirm your insurer’s current benefits and pharmacy rules.
Red flags and when to call your surgeon
This section isn’t here to scare you; it’s here to protect your time and your eye. Most people recover smoothly, but knowing the “call now” signals is part of a smart home setup.
Eligibility checklist for urgent contact (yes/no):
- Yes to sudden vision drop
- Yes to severe or rapidly worsening pain
- Yes to increasing redness with discharge
- Yes to flashes, a curtain-like shadow, or many new floaters
- Yes to nausea or headache paired with eye pain
If any answer is yes, contact your surgical team immediately using their emergency instructions. Save this checklist and keep the clinic number visible in your phone favorites.
I once tried to “tough it out” with discomfort that was probably normal. The problem wasn’t the symptom—it was the uncertainty. A two-minute reassurance call would have saved me an hour of worry and a truly dramatic conversation with my ceiling.
- Sudden vision changes are not a “wait-and-see” moment
- Severe pain deserves same-day guidance
- Keep emergency instructions easy to find
Apply in 60 seconds: Add your clinic number to favorites and label it “Eye Surgery Team.”
Caregiver plan for time-poor families
If you’re helping a parent, partner, or friend, your job is not to hover—it’s to remove friction. The best support is quiet, organized, and slightly boring. Boring is good in week 1.
- Drive on day 1 and plan for at least one follow-up trip
- Set up the drop station together once
- Prep two easy meals and visible hydration
- Do a 3-minute nightly floor clear
- Ask for the written post-op plan and store it in one place
I learned this the hard way while trying to be “helpful” by giving too many reminders. It came off like a lovable robot with Wi-Fi issues. Once I switched to setting timers and quietly refilling the drop basket, everything got calmer.
U.S. note: If your family is navigating Medicare Part B coverage for cataract surgery, private insurance, or a premium lens upgrade, ask the clinic for an itemized estimate that separates the surgical fee from lens choices and post-op medications. Outside the U.S., you may have a different cost structure, but the same principle holds: get the written breakdown and confirm what’s included in your package.
Show me the nerdy details
Caregiver effectiveness is often a logistics problem, not a motivation problem. A shared schedule and centralized supplies can reduce repeated decision-making and improve adherence without nagging.
Short Story: Recovery is a logistics game (120–180 words)
Short Story: Recovery is a logistics game (120–180 words)
On the second day after surgery, I felt confident enough to “go back to normal.” That confidence lasted exactly nine minutes. I couldn’t find my drops, my living room lamp was blasting stadium-level brightness, and my phone reminder was set to the wrong time because I’d labeled two bottles with identical sticky notes. I sat there blinking like a confused owl, trying to remember whether I’d already done the morning dose or just thought about doing it.
The funniest part was how quickly my pride melted into gratitude for the simplest fixes. Once I put everything into one basket, switched to a softer lamp, and wrote the schedule in plain English, the day stopped feeling like a quiz. It felt like recovery again. That’s the secret of week one: you don’t need heroic willpower. You need a system that still works when you’re sleepy, tender-eyed, and a little emotionally dramatic about lighting.
Quick day-by-day reset for days 1–7
This is your lightweight roadmap. Adjust based on your surgeon’s instructions.
- Day 1: Rest, protect the eye, start the drop routine, keep lighting soft.
- Day 2: Short walks indoors, confirm drop timing, limit heavy chores.
- Day 3: Re-check floor clutter, test comfort seating, build a predictable rhythm.
- Day 4: Gradually increase reading/screen time if comfortable.
- Day 5: Review any lingering glare or dryness and adjust environment.
- Day 6: Prep questions for follow-up—vision changes, drop side effects, sleep notes.
- Day 7: Decide what to keep long-term (better lamp, safer pathway, simpler routines).
I like to do a two-minute evening reset—refill tissues, confirm tomorrow’s drop schedule, and clear the travel path. It’s tiny effort with a surprisingly big comfort return.
A simple at-home infographic
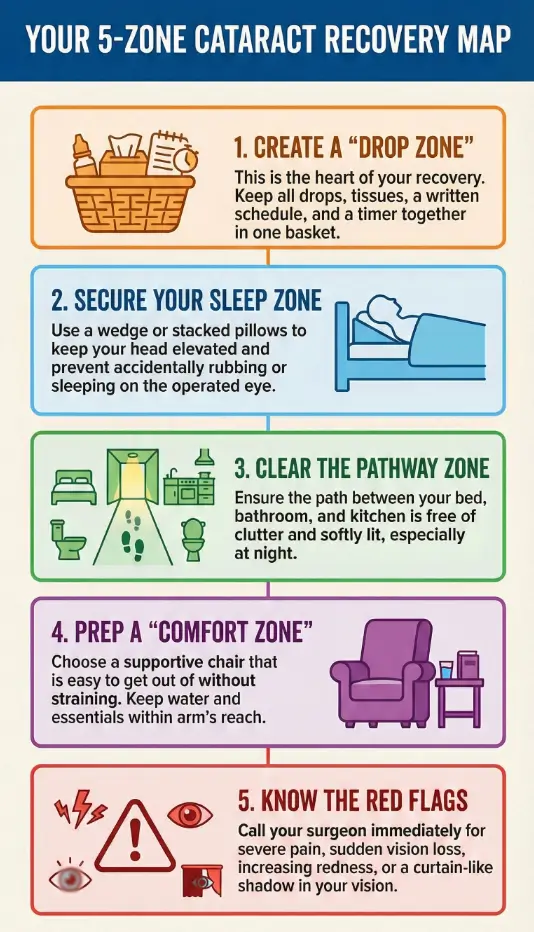
This quick visual is meant to be screenshot-friendly for families.
FAQ
How long should I wear the eye shield at home?
Follow your surgeon’s exact timeline. Many people wear it while sleeping for several nights to prevent accidental rubbing. Apply in 60 seconds: Place the shield next to your bed with a reminder note.
Can I cook and do light chores during the first week?
Often yes, but avoid heavy lifting, strain-heavy bending, and anything that risks dust or splashes. Keep tasks under 10–15 minutes at a time early on. Apply in 60 seconds: Move your most used kitchen items to counter height.
What lighting is best right after surgery?
Soft, indirect lighting tends to be more comfortable than overhead glare. A shaded lamp and dimmable bulbs can make day 1 feel 30% less irritating purely by comfort perception. Apply in 60 seconds: Switch on a shaded lamp and turn off harsh overhead lights in your main room.
Do I need special sunglasses?
Not always, but a comfortable pair can help with outdoor glare and wind. If you already own a good pair, you may be set. Apply in 60 seconds: Put sunglasses by your keys to avoid last-minute scrambling.
How can I reduce the cost of post-op drops?
Ask for generics where appropriate, confirm refill timing, and compare pharmacy pricing if you’re paying out of pocket. Request a written estimate when you can. Apply in 60 seconds: Write the exact drop names and ask your pharmacy for a quick cost check.
When can I use my computer or phone normally?
Many people start with short sessions the same day, then build up as comfort allows. If you get headaches or notable glare, scale back. Apply in 60 seconds: Turn on large text and set a 10-minute break timer.
Your 15-minute win before the next nap
The week I finally stopped improvising, recovery got easier. Not because my eye magically became invincible, but because my home stopped asking me to make decisions while half-awake. That’s the real secret behind a good first-week setup: you design a space that protects you from your own tired habits.
If you want the highest-leverage next step within 15 minutes, do this mini trio: clear the bed-to-bathroom path, build a single drop basket, and set two reminders for tomorrow. That small system will save you repeated stress and preserve the calm you actually deserve while your vision settles.
- One pathway, one basket, one schedule
- Soft light reduces irritation
- Plan comfort before fatigue hits
Apply in 60 seconds: Take a photo of your drop schedule and set it as your lock screen.
Last reviewed: 2025-12; sources: AAO / NEI / NHS.
home setup after cataract surgery, cataract recovery first week, post-op eye drops schedule, cataract surgery supplies cost, sleep positioning after cataract surgery

