
Two “Healthy” Items Can Quietly Burn Through 500–900 mg of Sodium Before Dinner
If you’re trying to follow a 7-Day DASH Meal Plan Grocery List for high blood pressure + macular degeneration, that’s the modern frustration: you buy the “good” foods, you cook at home, and sodium still sneaks in—while you’re also trying to stack lutein and zeaxanthin (leafy greens, eggs, orange/yellow produce) without turning meals into a joyless project.
Keep guessing and you lose twice: blood pressure progress stalls, and eye-supportive eating becomes another “I’ll start Monday” plan that collapses midweek.
This post gives you a repeatable week: a simple DASH-style structure, mix-and-match meals, and a brand-agnostic US grocery list that makes low-sodium choices easier—without pretending food replaces AMD care. I’m using the same method I use for my own busy weeks: fewer decisions, more defaults, and a label routine that catches the stealth culprits.
Table of Contents
Safety first: use this meal plan without risky assumptions
This plan is general education, not medical advice. It’s designed for the common US situation: you want a lower-sodium eating pattern (DASH-style) while also choosing foods that are naturally rich in lutein and zeaxanthin (two carotenoids often discussed in AMD nutrition). But a few situations change the rules—fast.
I learned this the awkward way: years ago I “cleaned up” my food overnight, felt dizzy by day three, and proudly told myself I was being disciplined. In reality, I was being reckless. The fix wasn’t heroics. It was calibration.
- Yes if you have uncomplicated high blood pressure and want a lower-sodium weekly template.
- Yes if you’re aiming for more leafy greens, eggs, and colorful produce for eye-supportive eating.
- Pause if you have kidney disease, heart failure, or are on a strict fluid restriction.
- Pause if you have diabetes using insulin or meds that can cause low blood sugar with diet changes (if you’re also managing eye complications, start with a clear baseline like what diabetic retinopathy is and why it changes follow-up urgency).
- Pause if you take blood thinners or have been told to keep vitamin K intake consistent.
Neutral action: If you checked any “Pause” box, bring this plan to a clinician or registered dietitian and ask for personalized targets.
High-risk conditions that change the rules (kidney disease, heart failure, diabetes meds)
These conditions don’t mean “you can’t eat well.” They mean you may need different limits (especially for potassium, fluids, or meal timing). A plan that’s great for one person can be problematic for another. If you’re unsure, treat your clinician’s targets as the scoreboard.
When to seek help: sudden vision changes or severe BP symptoms (don’t wait)
If you have chest pain, severe headache, shortness of breath, weakness/numbness, confusion, fainting, or your blood pressure readings are dangerously high, seek urgent care. For vision: sudden distortion, a dark curtain, new flashes/floaters, or rapid central blurring should be treated as “call today,” not “wait and see” (if you’re debating whether it’s “just aging,” bookmark the red-flag guide to serious eye disease vs normal aging).
Cooking with low vision: lighting + contrast tweaks that prevent kitchen mishaps (quick wins)
Meal prep is supposed to reduce stress, not create it. Use bright task lighting, increase contrast (dark cutting board for light foods, light board for dark foods), and keep a “same place every time” zone for knives and measuring spoons. It’s a small system that prevents the big drama (and if reading labels is the bottleneck, try the practical strategies in low-vision reading for AMD in your 70s and 80s).
AMD in 90 seconds: what matters for your grocery cart (dry vs wet)
Here’s the simplest framing that protects your time: AMD isn’t one thing. It’s a category. And the two big lanes—often described as dry and wet—change how urgent follow-up can be (if you want the cleanest overview, see dry vs wet age-related macular degeneration explained in plain language). Diet can support overall eye health, but it doesn’t replace evaluation or treatment.
I once watched a friend “eat perfectly” while postponing their eye appointment because it felt productive. I get it. Food is controllable. Clinics are not. But AMD is not a willpower contest.
| Type (common framing) | What it generally means | What food can realistically do |
|---|---|---|
| Dry AMD | Often slower progression; may have minimal early symptoms. | Support overall health, nutrient intake, and consistency; complement clinician-guided monitoring. |
| Wet AMD | Can change vision more quickly; requires prompt evaluation and treatment planning. | Support general health and treatment adherence (meal prep helps), but does not replace treatment. |
Dry vs wet: the two lanes that change follow-up urgency
Clinics often emphasize that “wet” changes can progress quickly, so sudden distortion or central blur is a “don’t sit on it” signal. Your grocery cart supports your baseline; your eye team manages the diagnosis and treatment lane.
Open loop: why “eye-healthy” eating still needs an eye exam (even if you feel fine)
Because early AMD can be quiet. You can be doing everything “right” and still need monitoring. Think of food as the foundation—not the entire building (and if you’re wondering how often you should actually be checked, how often seniors should get dilated eye exams is a useful starting point).
Red-flag symptoms: the 60-second distortion check (Amsler grid logic)
If straight lines start looking wavy, your brain may try to negotiate. “Maybe it’s the lighting.” “Maybe I’m tired.” The honest truth is simpler: distortion deserves attention.
I’ve done this denial dance myself—once with a tech issue, once with my own body. Both times I lost time I didn’t need to lose. Your goal isn’t panic. It’s signal detection.
- Check one eye at a time.
- Look for new bends, blank spots, or missing areas.
- Write down what changed and when (a simple structure helps—see a printable symptom diary for seniors you can keep on the fridge or in your phone).
Apply in 60 seconds: Do a quick one-eye-at-a-time straight-line check and note any change in your phone.
What “wavy lines” and central blur usually mean in AMD symptom language
People describe it as waviness, bending, distortion, or a “smudge” where details should be. The point is not self-diagnosis; it’s recognizing when vision changes should trigger professional evaluation.
Amsler grid: how it’s used and what counts as a change
An Amsler grid is a simple tool: you look at a central dot and notice whether the surrounding lines look straight and continuous. A change from your normal is the key signal. If you use it, keep the lighting and distance consistent so you’re comparing apples to apples.
Open loop: the symptom that people call “just glasses” (but isn’t)
If your prescription “suddenly feels wrong” in one eye—especially with new distortion—don’t assume it’s just time for new lenses. That’s a common delay point (and if you’re trying to understand bigger-picture risk in later decades, blindness risk after 70 can help you calibrate what’s “watch and wait” versus “act now”).
DASH targets: sodium wins without extreme rebounds
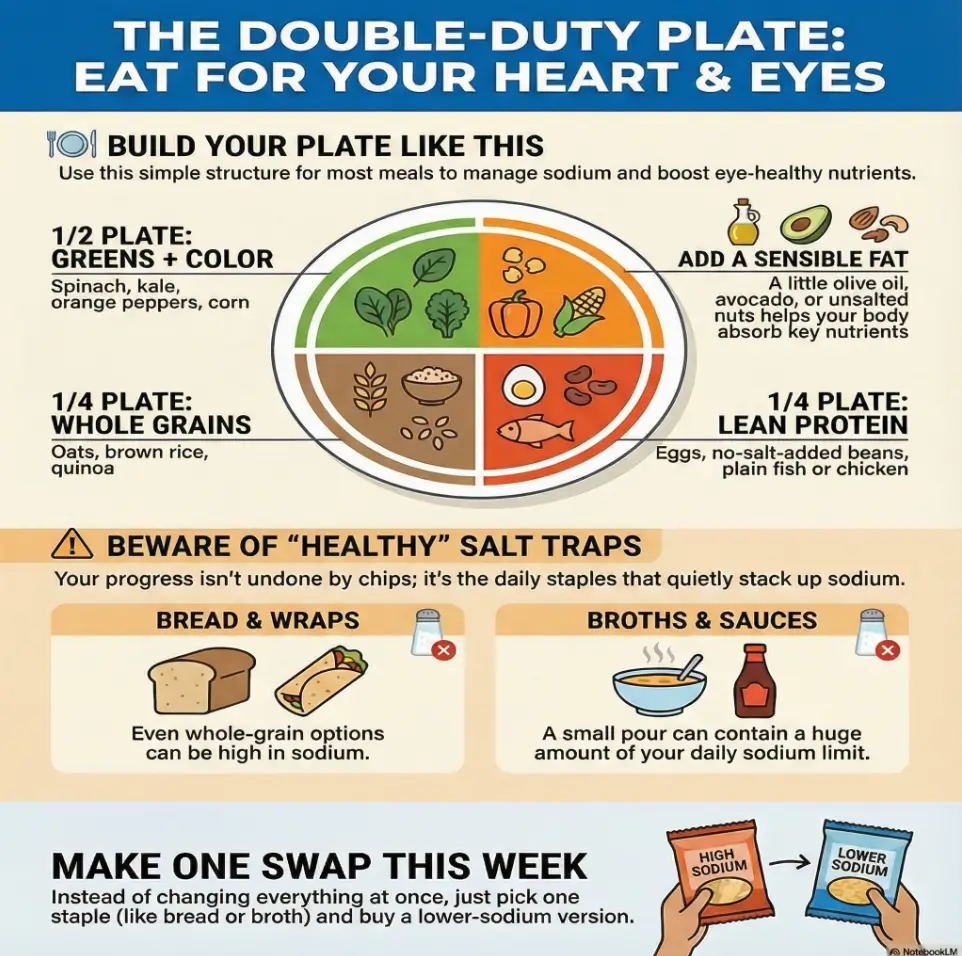
DASH is less a “diet” and more a default operating system: fruits/veg, whole grains, lean proteins, nuts/legumes, and a low-sodium approach that’s actually sustainable. In the US, sodium is the boss level—not because you’re doing anything wrong, but because it hides in “normal” foods.
Practical target framing: many people aim for somewhere in the neighborhood of 1,500–2,300 mg sodium per day, depending on clinician guidance, health conditions, and adherence. If you’ve been told a specific number, that’s your number.
Sodium basics: where DASH usually succeeds (and where it quietly fails)
Home-cooked meals with simple ingredients usually land lower in sodium—without you doing math. The quiet failure happens when you keep your old staples (bread, wraps, deli meat, jarred sauces, boxed broths) and assume the “healthy vibe” protects you. It doesn’t.
Potassium caution: when “more potassium” is not automatically better
Potassium-rich foods are a DASH hallmark, but certain conditions and medications require caution. If your clinician has ever warned you about potassium, treat it like a real constraint—not a suggestion. You can still do DASH. You just do it with the correct guardrails.
Open loop: why your “healthy bread” can erase a day of progress (label math preview)
Most people don’t blow sodium on chips. They blow it on “normal”: two slices of bread here, a splash of broth there, a “healthy” sauce that’s quietly loud. We’ll make this painfully clear (in a helpful way) in the label-reading section.
Double-duty food map: lutein/zeaxanthin + low-sodium staples (the overlap zone)
This is where the plan gets pleasantly unfair—in your favor. Some foods are high-leverage: they fit DASH, they play well with low sodium, and they naturally bring pigments commonly associated with macular nutrition.
My own “adulting trick” is boring but effective: I keep two bags of frozen greens and a carton of eggs in the house at all times. When I’m tired, my standards drop. My system catches me.
- Leafy greens: spinach, kale, collards (fresh or frozen)
- Eggs: especially as a quick lutein-forward breakfast base
- Orange/yellow produce: corn, orange bell peppers, squash
- Beans/legumes: no-salt-added canned or cooked-from-dry
- Whole grains: oats, brown rice, quinoa, whole-wheat pasta
- Fish (as tolerated): salmon, sardines (watch sodium in canned versions)
- Unsalted nuts/seeds: walnuts, chia, ground flax
- Olive oil: not “diet food,” just a useful tool for satisfaction
Show me the nerdy details
Carotenoids like lutein and zeaxanthin are fat-soluble, which is why a totally fat-free plate can under-deliver even if you ate the “right” vegetables. You don’t need a greasy meal—just a sensible fat source (olive oil, avocado, eggs, nuts) so the nutrition you bought actually counts.
The “green + orange” rule (kale/spinach + corn/peppers) you’ll actually repeat
Make it simple: one “green” and one “orange/yellow” most days. It’s not magic. It’s a memory aid that reliably improves nutrient density without requiring a PhD in meal planning.
Egg strategy: lutein-forward breakfasts without turning salty
Eggs become a sodium problem when they’re paired with processed meats, salted cheese, and restaurant-level seasoning. At home: eggs + greens + unsalted seasoning + a whole grain is a clean, repeatable win.
Fat matters (gently): why totally fat-free meals can under-deliver carotenoids
This is the part that surprises people. If your meals taste like punishment, you won’t stay with it. A tablespoon of olive oil isn’t a failure. It’s a strategy.

7-day meal plan: DASH structure with lutein built in (mix-and-match)
This week is designed like a capsule wardrobe: a few core pieces that combine well. You’re not cooking seven brand-new dinners. You’re remixing the same honest building blocks: grains, beans, greens, eggs, fish (optional), and low-sodium flavor.
Personal confession: my “meal planning era” started the day I realized takeout wasn’t a treat—it was a default. I didn’t need more motivation. I needed fewer decisions. This is that.
| Day | Breakfast | Lunch | Dinner | Snack |
|---|---|---|---|---|
| Day 1 | Oats + berries + chia | Bean bowl + greens + corn | Salmon (or chicken) + kale + brown rice | Unsalted nuts + fruit |
| Day 2 | Eggs + spinach + whole-grain toast | Greek yogurt + fruit + walnuts | Turkey or tofu stir-fry + peppers | Hummus + carrots |
| Day 3 | Smoothie (greens + fruit) + oats | Leftover bowl remix | No-salt-added chili + side salad | Apple + peanut butter |
| Day 4 | Egg + veggie scramble | Tuna/salmon salad (low sodium) + greens | Sheet-pan veggies + beans + quinoa | Cottage cheese (check sodium) or yogurt |
| Day 5 | Overnight oats | No-cook: rotisserie chicken (watch sodium) + bag salad | Whole-wheat pasta + olive oil + spinach + peppers | Fruit + unsalted nuts |
| Day 6 | Yogurt + berries + flax | Soup-and-salad (homemade, low sodium) | Sardines (if tolerated) + roasted veg + grain | Popcorn (unsalted) + fruit |
| Day 7 | Eggs + greens | Leftover remix day | “Clean-out-the-fridge” bowl | Whatever you didn’t finish |
Day-by-day menu (breakfast/lunch/dinner/snack) with 10-minute swaps
Swaps are the whole point. If you planned salmon and you’re not feeling it, swap to beans. If you planned cooked greens and you’re exhausted, use frozen. The only non-negotiable is the structure: plants + protein + whole grains, with sodium kept honest.
No-cook day + leftover remix day (the relapse-proofing design)
Your life will happen midweek. The plan expects it. No-cook day is not “cheating.” It’s a pressure valve that keeps you out of the drive-thru spiral.
Let’s be honest… the plan only works if Monday is easy
Make Monday the lowest-friction day. Use frozen greens, canned no-salt-added beans, and a grain you can reheat. Your future self will feel personally supported.
- Build 3 default breakfasts you don’t hate.
- Cook once, remix twice.
- Protect “no-cook day” like it’s a meeting.
Apply in 60 seconds: Pick your Monday dinner now: frozen greens + beans + grain + olive oil + seasoning.
Short Story: I once tried to “do everything right” in one week—new recipes, new ingredients, new habits, all at once. By Thursday, my kitchen looked like a small tornado had taken up residence. I was tired, I was annoyed, and I was mad at the plan (even though I was the one who made it impossible).
That night I ordered something salty and expensive and ate it standing up, because I didn’t even have the patience to sit. The next morning, I started over with a smaller promise: two breakfasts I actually liked, one big pot of grain, and frozen greens that didn’t ask me to wash, chop, or pretend I had extra time. My “perfect” week died, and my repeatable week finally showed up.
Grocery list: US aisles, brand-agnostic, printable (Buy This / Not That)
This is built for US grocery reality: big-box stores, regular supermarkets, and “I’m not going to three places” energy. Print it. Screenshot it. Use it as a default cart you can repeat weekly.
I keep a running list called “boring wins.” The second I stop buying boring wins, my week gets dramatic. This list keeps the drama low.
- No-salt-added beans and tomatoes are high-leverage.
- Frozen greens are a weekday superpower.
- Unsalted nuts prevent “snack sodium” creep.
Apply in 60 seconds: Add two bags of frozen spinach/kale and one carton of eggs to your cart right now.
Produce (lutein-forward picks + budget tiers)
- Greens: spinach, kale, collards (fresh or frozen)
- Orange/yellow: corn (frozen), orange bell peppers, carrots, squash
- Bonus color: blueberries, oranges, tomatoes
- All-purpose: onions, garlic, lemons/limes (flavor without sodium)
Proteins (low-sodium wins) + what to limit
- Buy this: eggs, plain chicken/turkey, tofu/tempeh, dried lentils/beans, low-sodium canned fish (if available)
- Limit: deli meats, heavily seasoned rotisserie chicken, jerky, most frozen breaded proteins
- Tip: If you do canned fish, check sodium and choose the lowest option you can find.
Pantry/freezer defaults that keep sodium down without “diet vibes”
- Whole grains: oats, brown rice, quinoa, whole-wheat pasta, barley
- No-salt-added: beans, tomatoes, tomato sauce (or low-sodium)
- Flavor tools: vinegar, mustard (check sodium), spices, salt-free blends, smoked paprika, cumin
- Freezer: frozen spinach/kale, frozen corn, frozen peppers, frozen berries
- Dairy/alt: plain yogurt, low-sodium cottage cheese (some are high—check), milk or fortified unsweetened alternatives
- Frozen greens if you need speed, less waste, and consistent “weeknight compliance.”
- Fresh greens if you love salads and will eat them within 3–4 days.
- Dried beans if you want the lowest sodium and the lowest cost (time trade-off).
- No-salt-added canned beans if you need “open, rinse, eat” convenience.
Neutral action: Choose one convenience option and one budget option so your plan survives both busy and calm weeks.
Sodium traps: label-reading in 90 seconds (the stealth culprits)
This section is where your blood pressure plan either quietly succeeds—or quietly gets kneecapped. In the US, sodium is often a packaging problem, not a personal failing. The fix is a repeatable label routine.
I used to read labels like a novel—slow, confused, emotionally invested. Now I read them like a bouncer. Three checks. Decision made. Move on.
Bread, wraps, cereal: the “looks healthy” aisle
Even “whole grain” can be sodium-dense. The trap isn’t one item—it’s the stack: breakfast toast + lunch sandwich + dinner grain bowl with packaged sauce. You can keep bread. You just have to choose it intentionally.
Broths, sauces, spice blends: the tablespoon problem
Broth and sauces are concentrated. A small serving can carry a lot of sodium, and many of us pour like we’re filming a cooking show. If you’re using broth often, look for low-sodium versions or make a simple homemade base when possible.
Here’s what no one tells you… “reduced sodium” can still be high
“Reduced sodium” usually means “less than the original,” not “low.” It can still be a lot. Your goal is not perfection. Your goal is avoiding the stealth hits that make your daily total spike.
Show me the nerdy details
On US Nutrition Facts labels, sodium is listed in mg per serving, and “servings per container” matters more than people expect. If something has 2 servings and you eat the whole package, you need to multiply. This is why “healthy snacks” can quietly become a sodium event.
This is not medical advice—just quick math so you can make smarter swaps.
Neutral action: If the number surprised you, swap just one staple (bread or sauce) to a lower-sodium option this week.
- Check mg per serving and servings per container.
- Beware “reduced sodium” language.
- Swap one staple at a time for better adherence.
Apply in 60 seconds: Pick one label you buy weekly and compare two brands by sodium per serving.
Treatment reality check: what food can support—and what it can’t replace
It’s tempting to want a meal plan to be a solution to everything. But AMD care is a system: monitoring, diagnosis, and (when needed) treatment. Food supports health, energy, and routine—especially when appointments and anxiety spike. But it does not replace clinical care.
I’ve been the person who tried to “research my way out” of needing a professional. It never ends well. The healthier move is using food as a support beam while you follow the actual care pathway.
Dry AMD support: where AREDS2 comes up (and why it’s stage-specific)
You may hear about AREDS2 supplements in the context of certain stages of AMD. The important part is not memorizing ingredients—it’s asking your eye clinician whether it fits your stage and your medication profile (especially if smoking history is part of your story, read AREDS2 for smokers: what to ask and what to avoid). Supplements can interact with other conditions and aren’t universally appropriate.
Wet AMD: anti-VEGF injections and other options (high-level, non-prescriptive)
For wet AMD, treatment discussions often include injections (commonly described as anti-VEGF therapy). Your clinician guides timing and selection (if you want a clear “what does the timeline look like?” overview, start with a typical wet AMD injection schedule, then review what to expect at your first anti-VEGF injection). Your job is to show up and keep routine stable—sleep, meals, hydration—so follow-up isn’t derailed by chaos.
Prevention basics that overlap with this plan (BP control, smoking, diet patterns)
Organizations like the National Eye Institute and major medical centers consistently emphasize risk-factor management: blood pressure control, not smoking, and overall healthy eating patterns. This plan is aligned with that “boring but powerful” lane (and if you want the eye-specific reason BP matters, see hypertensive retinopathy and what high blood pressure can do to the retina).
- Bring 7 days of home blood pressure readings (if you have them).
- List all medications and supplements (including “eye vitamins”).
- Note any vision changes: when they started, what you see, which eye.
- Ask: “Do I have dry or wet AMD?” and “Do I need AREDS2 for my stage?”
Neutral action: Put a one-line note in your phone with your key question for your next appointment (and if cost stress is part of the hesitation, it may help to read AMD treatment cost: what people actually pay and why it varies, plus Medicare coverage for Eylea injections if you’re navigating Part B realities).
Who this is for / not for (quick self-screen)
This is for time-poor people who want a plan that behaves like a tool, not a personality. It’s also for anyone who’s tired of being told to “eat healthy” with no operational instructions.
My rule: if a plan requires you to become a new person by Tuesday, it’s not a plan. It’s a fantasy.
Best fit scenarios (new hypertension, early/intermediate AMD support goals)
- You want a low-sodium weekly structure you can repeat.
- You’re willing to buy plain staples and season them yourself.
- You want to emphasize leafy greens, eggs, and colorful produce more consistently.
Not for: clinician-managed restrictions (fluid limits, renal diets, severe swallowing issues)
If you’ve been given strict medical limits, use this as a conversation starter, not a self-prescription. A registered dietitian can adapt the framework safely.
If you’re on BP meds: what to track in week 1 (symptoms + home readings)
Track home BP readings if you already do so, and watch for dizziness or unusual fatigue when changing dietary sodium. The goal is steady improvement, not “crash dieting.”
Common mistakes: the 7 ways people accidentally go high-sodium again
This is the section that saves money and regret. Most people don’t fail because they lack discipline. They fail because the environment is set up to push sodium and convenience together.
I’ve been humbled by this more times than I’d like to admit. The solution isn’t guilt. It’s design.
| Mistake | Why it happens | Fix (low-friction) |
|---|---|---|
| Switching everything at once | Rebound cravings + decision fatigue | Swap one staple per week (bread OR broth OR sauce) |
| “Healthy” snacks that are salty | Packaging looks virtuous | Keep unsalted nuts + fruit as default snack |
| Deli meats + sauces | Fast lunches become sodium stacks | Use leftovers, beans, or low-sodium canned fish |
| Cutting fat too far | Food tastes sad → you quit | Add olive oil/avocado in measured amounts |
- Bread + broth + sauce can quietly dominate your day.
- Swap one staple per week for real momentum.
- Keep a “no-cook rescue” option ready.
Apply in 60 seconds: Decide your single swap for this week: lower-sodium bread or lower-sodium broth.

FAQ
How much sodium should I aim for on a DASH-style week?
Many people aim for a range around 1,500–2,300 mg/day depending on clinician guidance and personal health factors. If your clinician gave you a target, use that. If you’re unsure, start by reducing stealth sodium (bread, broths, sauces) rather than trying to “hit a perfect number” immediately.
Which foods are highest in lutein and zeaxanthin that people actually eat daily?
Leafy greens (spinach, kale, collards), eggs, corn, and orange/yellow peppers are common, practical options in US stores. The best choice is the one you’ll eat consistently—most days, not once a month.
Are eggs okay for eye health and heart health?
For many people, eggs can be a useful, satisfying protein that fits into a DASH-style week when paired with vegetables and whole grains. The bigger issue is what comes with eggs (processed meats, salty cheese, restaurant seasoning). If you have specific cholesterol or heart-disease guidance, follow your clinician’s plan.
Is frozen spinach/kale as good as fresh for eye nutrients?
Frozen greens are often picked and frozen quickly, and they’re a strong choice for consistency and less waste. If fresh greens routinely go slimy in your fridge, frozen wins in the only category that matters: you actually eat them.
Do I need supplements like AREDS2 if I eat lutein-rich foods?
Some clinicians recommend AREDS2 supplements for certain stages of AMD, but it’s not a universal “everyone should take this” situation. The safest approach is to ask your eye clinician whether AREDS2 is appropriate for your stage and your medication profile.
How can I eat low sodium at US chain restaurants without guessing?
Use simple tactics: request sauces on the side, choose grilled/steamed items, skip soups and heavily sauced dishes, and look for nutrition information online when available. If the restaurant provides sodium data, it can save you a lot of guessing.
Can high blood pressure increase risk for AMD?
Major medical institutions list cardiovascular factors among the broader health context for AMD risk and progression discussions. Regardless of the exact risk contribution, blood pressure control is a strong “do it anyway” move for overall health—and it supports the routines that keep eye care consistent.
Conclusion: your 15-minute next step (and the “healthy bread” truth)
Let’s close the open loop: yes, your “healthy bread” can absolutely erase your progress—not because bread is evil, but because it’s quietly consistent. Two slices a day is 14 slices a week. If each slice is higher than you realized, the math adds up faster than your motivation can compensate.
Your win isn’t becoming perfect. Your win is becoming consistent. And consistency loves small, boring decisions repeated.
- Spinach/kale
- Orange peppers/corn
- Tomatoes/berries
- Eggs
- Beans/lentils
- Fish or poultry (plain)
- Oats
- Brown rice/quinoa
- Whole-wheat pasta
- Olive oil
- Avocado
- Unsalted nuts
- Pick one staple to swap: bread, broth, sauce, or deli meat.
- Buy the lower-sodium option on your next trip.
- Repeat the same swap for 7 days before you change anything else.
Neutral action: Write your single swap on a sticky note or phone reminder so you don’t “forget” at the store.
And if you want a quiet confidence boost: the National Eye Institute, the National Heart, Lung, and Blood Institute, and major heart-health organizations all emphasize the unglamorous basics—healthy patterns, sodium awareness, and consistency. Your job is not to become a different person. Your job is to make a different default (and if appointment fear is part of what makes “call today” hard, you’re not alone—see wet AMD injection anxiety in your 70s for practical ways to steady yourself and still follow through).
Last reviewed: 2025-12-29

