Tonight’s Pre-Op Calm: The 1:17 A.M. Protocol
Anxiety before eye surgery isn’t drama—it’s “threat math” around your most vital sense. When your brain treats the pre-op sheet like a thriller soundtrack, it’s time to switch from a mental spiral to a rule-friendly loop.
The Strategy
- Instruction Audit: Confirm fasting and drops.
- Grounding: Texture-heavy focus to break the “what-if” loop.
- Worry Window: Turn vague fear into a timed “next step.”
The Goal
Prioritize compliance and rest over perfection. No gadgets or midnight heroics—just a repeatable plan to show up steady.
If you feel anxious the night before eye surgery, keep it simple: confirm your instructions (food, meds, arrival time), then use a short calming loop. Try 2 minutes of slow nasal breathing (longer exhale than inhale), a 5–4–3–2–1 grounding scan, and a “worry window” where you write fears and one next action. Avoid late caffeine, alcohol, and doom-scrolling. If panic feels unmanageable, contact your surgical team.
Table of Contents

Safety and Disclaimer
This is educational, not medical advice. Always follow your surgeon’s instructions about eating/drinking, medications, eye drops, and sedation. Do not start supplements or new meds the night before surgery without clinician approval. If you have severe anxiety, panic attacks, suicidal thoughts, or feel unsafe, seek urgent help immediately (US: call/text 988).
- Don’t add new pills or supplements tonight.
- Do a quick instructions audit to reduce uncertainty.
- Use short, timed tools that settle your body without “fixing” your thoughts.
Apply in 60 seconds: Set a 2-minute timer, exhale longer than you inhale, and let “enough” be the goal.
Who this is for / not for
Who this is for
- Adults scheduled for common eye procedures (cataract, LASIK/PRK, retina injections, etc.) who feel “wired” the night before
- Caregivers helping a parent/partner stay calm and organized
- People who want non-drug mind-body tools that won’t interfere with pre-op instructions
Who this is not for
- Anyone with severe panic, mania, psychosis, suicidal thoughts, or substance withdrawal (needs professional support now)
- Anyone told they need medical clearance for anxiety/sedation changes (call the surgeon/anesthesia team)
- Anyone seeking dosing advice for sedatives, sleep meds, or supplements (not appropriate here)
Tonight’s game plan: calm + compliant, not “perfect sleep”
The 2-track goal (why it works)
- Track A: Medical compliance (instructions, arrival, meds, fasting) reduces uncertainty.
- Track B: Nervous system downshift lowers arousal even if sleep is imperfect.
Let’s be honest… you don’t need “8 hours,” you need “not spiraling”
Here’s a tiny truth that used to annoy me until it saved my night: sleep isn’t a moral test. The goal is not a perfect score, it’s functional calm. I’ve had nights before my own appointments where I slept in weird, chopped-up chunks and still showed up steady because I had a plan and I stopped negotiating with my thoughts at 1:17 AM.
- Yes to self-tools: you understand your fasting/med instructions, you feel anxious but safe, and breathing/grounding helps at least a little.
- No (call the surgical team/on-call line): you’re unsure about fasting/meds/drops, you took something you shouldn’t have, or you feel you might break instructions to cope.
- Urgent help now: chest pain, trouble breathing, fainting, or you feel unsafe (US: 988).
Next step: If you hit “No,” call the clinic now and ask for the on-call guidance.
The anxiety loop: why your brain picks “eye surgery” as a megaphone
Threat amplification 101 (especially with eyes)
Eyes are not “just another body part” in your nervous system’s imagination. Vision is your brain’s main dashboard, so the threat system treats anything eye-related like a five-alarm alert. That doesn’t mean danger is guaranteed. It means your brain is doing what it evolved to do: protect the camera.
For many common eye surgeries, people are often awake with local numbing and may receive medication to help them stay relaxed, which is one reason the night-before anxiety can feel mismatched with the actual experience. The mismatch is part of the problem: your body prepares for a bear; your calendar says “outpatient procedure.”
Show me the nerdy details
Anxiety is not just “thoughts.” It’s sympathetic arousal (heart rate, muscle tension, scanning behavior). Tools that change breathing and sensory attention work because they nudge autonomic tone. You don’t need to win an argument with your mind; you need to turn the volume down on the body signal that tells the mind, “We’re in danger.”
Curiosity gap: The one sentence your anxiety is trying to finish
Most spirals are one unfinished sentence on repeat: “What if ___ happens?” Your job tonight isn’t to erase the question. It’s to turn it into something your brain can file.
- Write the blank: “What if I panic during prep?”
- Then convert it: “If I panic, what is my next step?”
- Answer with one action: “I will tell the nurse I’m anxious and ask for coaching.”
I’ve watched anxiety shrink in real time when it finally gets a folder label. Not a guarantee, a next step.
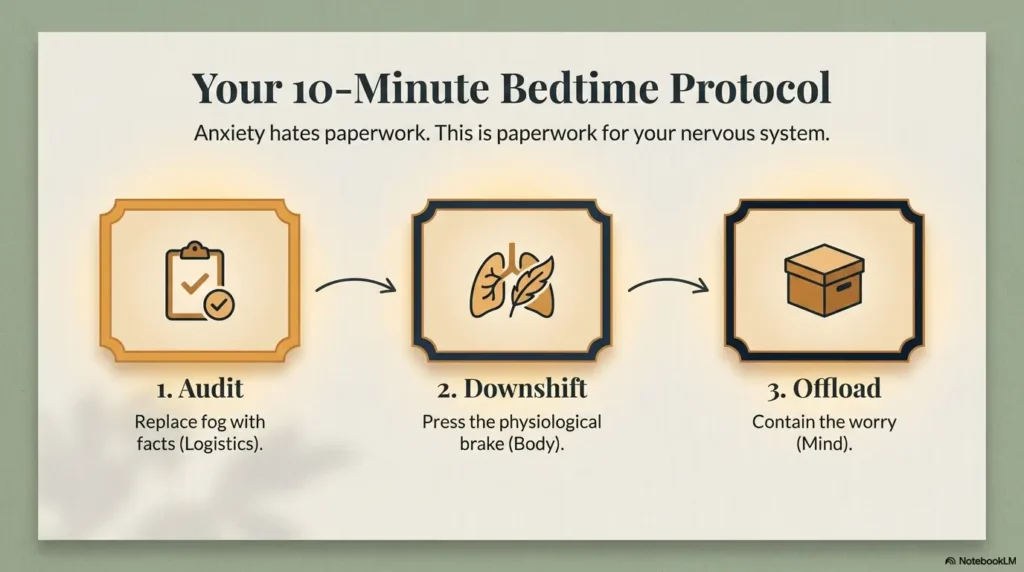
A 10-minute bedtime protocol that actually fits real humans
Step 1: “Instructions audit” (2 minutes)
- Fasting rules (food, water, coffee, gum, candy, mints)
- Meds to take/hold (especially diabetes meds, blood thinners, blood pressure meds)
- Eye drops (what time, which bottle, which eye)
- Driver/ride plan and contact
- Arrival time, location, ID/insurance
Tiny confession: I once “prepared” by thinking about the instructions very intensely without actually reading them again. My brain felt busy. My plan was… imaginary. The audit is not glamorous, but it’s calming because it replaces fog with facts.
Step 2: Body downshift (4 minutes)
Pick one tool: extended-exhale breathing, progressive muscle release, or legs-up-the-wall (if comfortable). The best technique is the one you’ll actually do without turning it into a performance review.
Step 3: Brain offload (4 minutes)
Write: 3 fears + 3 facts + 1 next action (one action per fear). This is how you stop hosting an all-night debate club in your skull.
- Audit reduces uncertainty.
- Downshift changes your body signal.
- Offload keeps thoughts from multiplying in the dark.
Apply in 60 seconds: Open Notes and write “3 fears, 3 facts, 1 next step.” Start with the first fear.
Technique 1: Extended-exhale breathing (the “physiological brake pedal”)
How to do it (no gadgets)
- Inhale 4 seconds through the nose.
- Exhale 6–8 seconds (nose or gently through pursed lips).
- Repeat 8–10 cycles (about 2 minutes).
Keep it gentle. No breath-holding competitions. If you feel lightheaded, shorten the inhale/exhale and slow down.
Curiosity gap: Why the exhale does the heavy lifting
Longer exhales cue a downshift in arousal. It’s the closest thing to a “brake pedal” you can press without swallowing anything. The mind may still chatter, but the body gets a calmer memo, and that memo matters.
Show me the nerdy details
Extended-exhale breathing tends to increase vagal influence and improve heart-rate variability patterns in some people, which correlates with calmer physiological states. You don’t need perfect ratios; you need a consistently longer exhale than inhale for a couple minutes to start shifting the signal.
Technique 2: Grounding for “spinning thoughts” (5–4–3–2–1 done right)
The fast script
- 5 things you see
- 4 things you feel (touch/temperature/pressure)
- 3 things you hear
- 2 things you smell
- 1 thing you taste
Here’s what no one tells you…
Grounding works better when you name textures, not just objects: “cool pillowcase,” “rough seam,” “warm mug,” “smooth phone screen.” Your brain can argue with “I’m safe.” It can’t argue with “cotton feels scratchy on my wrist.”
Small anecdote: once, during a pre-procedure wait, my thoughts were doing parkour. I grounded by counting the tiny acoustic “ticks” of a wall clock and feeling my shoes press into the floor. Nothing spiritual happened. I just stopped launching new fears every ten seconds. That was enough.
Input 1: How many minutes do you have? (2, 5, or 10)
Input 2: Anxiety level right now (0–10)
Input 3: Can you focus on your breath without feeling worse? (Yes/No)
Output:
If Yes + anxiety ≥6: do 2 minutes extended-exhale, then 1 round 5–4–3–2–1.
If No: skip breath focus and do 2 rounds 5–4–3–2–1 (texture-heavy).
If anxiety ≤5: do one tool and stop. Don’t “practice” your way into a spiral.
Next step: Choose your loop and set a timer now.
Technique 3: The worry window (contain anxiety instead of negotiating with it)
Set a timer for 7 minutes
- Write everything you’re afraid of, uncensored.
- Then add one line: “If this happens, my next step is ___.”
Curiosity gap: Why “scheduled worry” reduces nighttime spikes
Your brain relaxes when it trusts you won’t ignore the concern, but you also won’t host it all night. You’re basically telling your nervous system: “I heard you. Here’s the plan. Now we rest.”
A trick that helps: end your worry window with a physical action that signals closure. Fold the paper. Put it under a book. Or slide it into a drawer. This is not symbolism for symbolism’s sake; it’s your body learning the moment worry is “done.”
Sleep that respects pre-op rules: what helps without backfiring
Sleep supports that are usually safe (non-med)
- Cool, dark room; slightly lower temperature if you can
- Warm shower and clean sheets (sensory comfort counts)
- Calming audio (low-volume music, familiar podcast episode, or guided relaxation)
- Consistent bedtime and a “lights down” ritual
- Light snack only if your instructions allow it
What to avoid (common night-before traps)
- Late caffeine, alcohol, cannabis (can worsen sleep quality and conflict with instructions)
- “Just in case” supplements (melatonin, valerian, magnesium) unless cleared
- Screen doom-scroll spirals, medical forums at midnight
This is where I get gently bossy: don’t experiment tonight. The night before surgery is not the time to debut a new supplement, a new sleep device, or a new “I saw this on TikTok” hack. Your goal is calm + compliance, not novelty.
Also, a reassuring reality check: major medical sources describe many eye surgeries as outpatient procedures, and common ones like cataract surgery are often done with you awake while the eye is numb, sometimes with medicine to help you stay relaxed. That matters because it reframes tomorrow as “team-guided procedure,” not “you alone in the wild.” Read the official cataract surgery guidance (National Eye Institute).
Common mistakes the night before eye surgery (and what to do instead)
Mistake #1: “I’ll Google every complication until I feel prepared”
I understand the impulse. I have also been that person at 12:41 AM reading a forum thread from 2011 written by someone’s cousin’s neighbor. The result is rarely “prepared.” It’s usually “electrified.”
Instead: limit research to official instructions and your surgeon’s materials. If a question matters, write it down for the team. Google is not your overnight nurse.
Mistake #2: Trying to “power-control” sleep with new pills or supplements
This is the sneakiest trap because it feels responsible. But it can conflict with fasting/sedation instructions and can create new side effects at the worst time.
Instead: do breathing + grounding + routine. If you’re considering changing meds to cope, call the clinic or anesthesia/surgical team for guidance. If the stress is coming from a long medication list, use a one-page medication list template so you’re not relying on midnight memory.
Mistake #3: Skipping logistics because it’s “too stressful”
Avoidance looks like relief, but it keeps your brain in uncertainty. Uncertainty is anxiety’s favorite snack.
Instead: do the 2-minute instructions audit. Certainty is calming. Even imperfect certainty.
- You can follow instructions.
- Symptoms are anxiety-only (no chest pain, fainting, severe shortness of breath).
- Tools reduce intensity even a little (1–2 points on a 0–10 scale).
Time trade-off: 10 minutes now saves hours of spiraling.
- You’re unsure about fasting/meds/drops.
- You took something and worry it conflicts with instructions.
- You feel likely to break instructions to cope.
Cost trade-off: A short call can prevent a canceled or delayed procedure.
Next step: If you’re stuck, choose “Call.” It’s the safer fork.
What to tell yourself: 5 steadying scripts that don’t feel cheesy
Script set (pick one)
- “I can be anxious and still be safe and prepared.”
- “My job is compliance and showing up. The team handles the procedure.”
- “This is a temporary night. I’m allowed to feel wobbly.”
- “Facts first, stories second.”
- “I don’t need perfect calm. I need enough calm.”
Curiosity gap: The phrase that stops ‘catastrophe cinema’
Try this sentence whenever your mind starts screening Worst-Case Trailers: “What is my next step if I feel worse?” It forces your brain into planning mode. Planning is a calmer mental posture than predicting.
One of my favorite “non-cheesy” tweaks is to speak like a competent friend would, not like a motivational poster would. Example: “Okay. We’re anxious. Cool. We can still do the next right thing.” It’s oddly effective because it respects reality without worshiping it.
When to seek help tonight
Call your surgical team (or on-call line) if
- You’re unsure about fasting/meds/eye drops, or you took something you shouldn’t have
- Anxiety is escalating and you’re considering changing instructions to cope
- You have a history of severe panic around medical procedures and need a plan for check-in
Seek urgent help now if
- Chest pain, trouble breathing, fainting, or severe panic that won’t settle
- You feel unsafe, have suicidal thoughts, or cannot stop self-harm impulses (US: 988)
Caregiver note: if you’re supporting someone tonight, your goal is not to “win” against their anxiety. Your goal is to co-regulate and keep things compliant. Calm voice. Small steps. Fewer words. I’ve seen one gentle sentence do more than a whole lecture: “We can call the team if we need to. You’re not alone in this.” If you’re navigating vision change together, coping with vision loss as a couple can help you share the load without turning every night into a crisis meeting.
Short Story: The night I stopped trying to be brave and started being prepared (120–180 words)
Short Story: The night before a minor procedure years ago, I did what many smart, anxious people do: I tried to outthink fear. I read every page I could find, took mental notes, rehearsed questions, then wondered why my chest felt like a drumline. Around 2 AM, I finally did something embarrassingly basic.
I opened the instructions, checked the exact arrival time, put my ID and a water bottle by the door (for after), and texted my ride a simple confirmation. Then I set a 7-minute timer and wrote my fears like I was dumping a purse onto a table. The last line on the page was: “If I panic, I tell the nurse.” I still slept in fragments. But when morning came, I didn’t feel heroic. I felt ready. And ready is its own kind of calm.
FAQ
Is it normal to feel anxious the night before cataract surgery?
Yes. The night-before spike is common because uncertainty is high and control feels low. Many people are awake during cataract surgery while the eye is numbed, and medication may be used to help you stay relaxed, which can make the fear feel bigger than the actual experience. If your anxiety feels unmanageable, call your surgical team for a plan.
What can I do if I can’t sleep before eye surgery?
Aim for “rest and readiness,” not perfect sleep. Do a 2-minute instructions audit, then a short calming loop (extended-exhale breathing, grounding, worry window). If you don’t sleep much, you can still proceed safely in many cases, but always follow your team’s instructions and tell them you had a rough night. If screens are part of the spiral, consider a practical boundary like blue light glasses for insomnia and a hard “lights down” cutoff.
Can anxiety raise blood pressure and affect my eye procedure?
Anxiety can raise heart rate and blood pressure temporarily. Most surgical teams expect some pre-op anxiety and have ways to support you. The practical move is to use short body-calming tools tonight and tell the team tomorrow if you’re very anxious, especially if you have a history of blood pressure issues. If your dizziness or blur has been tied to meds before, see blood pressure medication dizziness and blurry vision so you can describe patterns clearly to your clinician.
Should I take melatonin the night before eye surgery?
Don’t start supplements the night before surgery unless your clinician has cleared it. Even “common” supplements can interact with sedation plans or affect how your body responds. If you already take something regularly, follow your pre-op medication instructions or call the team to confirm. If you’re juggling many medications or supplements, polypharmacy and vision problems can help you spot what’s worth flagging for the surgical team.
Can I drink coffee the morning of my eye surgery?
Follow your fasting instructions exactly. Some procedures allow small sips of clear liquids up to a cutoff time, but others do not, and “coffee” may not qualify depending on additives. If you’re unsure, call the clinic. Tonight’s goal is to remove ambiguity, not to gamble. If you’re also a glaucoma suspect and coffee is a recurring worry, you may find coffee limit for glaucoma suspects useful for a calmer, non-alarmist frame after your procedure.
What if I have a panic attack in the pre-op area?
Tell the nurse immediately. Use a simple script: “I’m having panic symptoms. I need coaching and a minute to breathe.” Then do extended-exhale breathing or texture-based grounding. Your team has seen this before; you’re not the first person whose nervous system showed up early.
How can a caregiver help someone calm down before eye surgery?
Be the external nervous system: handle the instructions audit, confirm ride logistics, and guide one short tool (2 minutes breathing or 5–4–3–2–1). Use fewer words and steady tone. Offer choices (“breathing or grounding?”) so the person feels agency without having to problem-solve. If the person is older and you’re trying to separate “normal nerves” from “something we should mention,” scan senior vision changes warning signs and bring the relevant notes to the appointment.
A caregiver “ready kit” and quote-prep list (so you don’t scramble at 6 AM)
This section is for the person doing the emotional labor and the logistics. If that’s you: you’re basically running a tiny, compassionate operation tonight. And you deserve a plan that doesn’t require superpowers.
- Procedure name and scheduled time
- Medication list (including OTC and supplements currently used)
- Allergies and prior anesthesia/sedation reactions
- Fasting question written as one sentence
- Anxiety history: “panic attacks yes/no,” and what has helped in the past
Next step: Put this list by your phone so you don’t rely on memory at midnight.
Caregiver micro-script that works surprisingly well: “We’re going to do three things: check the instructions, do one calming tool, then stop solving.” I’ve used versions of this with family members and, honestly, with myself. Anxiety is persuasive. Structure is more persuasive. If meds are part of the stress, print or screenshot a one-page medication list so you can answer questions cleanly without rummaging.
A simple infographic: the “Night-Before Flow” you can follow half-asleep
Coverage tier map: from self-tools to professional support (so you know where you are)
When anxiety spikes, people often jump straight from “I’m nervous” to “I’m doomed.” This map gives you a middle path. Think of it as your support ladder. You don’t have to climb to the top unless you need to.
- Tier 1: Self-tools (breathing, grounding, worry window)
- Tier 2: Caregiver co-regulation (calm voice, logistics handled, short scripts)
- Tier 3: Surgical team/on-call line (fasting/med/drops clarity; anxiety plan)
- Tier 4: Urgent medical evaluation (severe symptoms like chest pain, fainting)
- Tier 5: Crisis support (US: 988 if you feel unsafe or suicidal)
Next step: Circle your tier right now, then do the matching action only.
Commercial-entity reality check (neutral, not hype): if you’re reading official patient guidance, credible places to start include the National Eye Institute and the American Academy of Ophthalmology. For crisis support, the 988 Suicide & Crisis Lifeline is the right doorway. These aren’t “magic,” but they are calmer than random forums at midnight.

Next step (one concrete action)
Do this now: set a 10-minute timer and complete the Instructions Audit + Extended-Exhale Breathing. Then place your essentials (ID, insurance card, list of meds, glasses case, ride contact) by the door and stop problem-solving for the night. If “list of meds” is the hard part, use this printable one-page medication list template to keep things simple at check-in.
If you want a one-sentence mantra for the timer: “I’m not trying to feel nothing. I’m trying to be ready.” I’ve used it on nights when my nervous system was convinced it was auditioning for a disaster film. It’s simple. It works. Read official cataract surgery preparation guidance (AAO).
Conclusion
Remember the unfinished sentence your anxiety kept trying to complete: “What if ___ happens?” Tonight, you don’t need to answer every “what if.” You only need a next step. That’s the loop-closer. When you give your brain one clean action and follow the instructions, it stops sprinting in circles and starts walking in a line.
Your 15-minute win is simple: do the 10-minute protocol, stage your essentials by the door, and pick one steadying script. Then let the night be imperfect. Tomorrow belongs to the team, the plan, and the quiet competence of showing up anyway. And if you’re preparing for cataract logistics, it can also help to know what’s typically covered: Medicare cataract surgery cost (2026) and the Medicare glasses-after-cataract-surgery rule are common “I wish I’d known this earlier” questions.
Last reviewed: 2026-02-20.