
Navigating the Threshold:
Making Your Home Predictable Again
That small shoulder-thud against the door frame can feel almost ridiculous, until it happens again, in the same hallway, under the same bad light. For those living with glaucoma field loss, familiar rooms can start behaving unpredictably. The doorway is open, the path seems clear, yet peripheral vision loss, glare, and low contrast can make the frame arrive before the brain has fully registered it.
Keep guessing, and a “minor bump” can become a bruise, a near-fall, or a quiet reason to avoid parts of your own home.
This guide provides practical fixes—better contrast, safer lighting, and movement habits—to make the safest route feel natural again. No warning labels required; just home-safety logic built for the daily reality of vision loss.
Table of Contents
Safety / Disclaimer: Door-Frame Bumps Are Data, Not Just Clumsiness
Repeatedly bumping into door frames is not a character flaw. It is not proof that someone is “getting careless.” It is information.
With glaucoma, side vision can narrow or develop missing areas. The National Eye Institute explains that glaucoma can cause loss of side vision and blind spots, sometimes before a person notices major trouble in central vision. That matters at home because door frames live in the edges of awareness, not in the center of the stage.
Treat Repeated Collisions as a Vision-Safety Signal
If you or someone you love keeps clipping the same doorway, treat the pattern like a smoke alarm with a low battery. Not panic. Not blame. But attention.
A single bump may be ordinary life. A 7-day pattern is different. If the same shoulder hits the same frame in the same lighting, the house is giving you a map.
- Notice which side of the body hits.
- Notice the time of day and lighting.
- Notice whether the person was turning, carrying something, or rushing.
Apply in 60 seconds: Write down the last doorway you hit and what direction you were moving.
This Guide Supports Care, It Does Not Replace an Eye Exam
This guide is practical education, not a diagnosis. Glaucoma management belongs with an eye doctor, and changes in vision deserve medical attention.
Home changes can reduce collisions, but they do not treat eye pressure, optic nerve damage, medication problems, or disease progression. A safer doorway is a tool. It is not a medical plan wearing little rubber feet.
Why New or Worsening Field Loss Needs Prompt Attention
Call an eye doctor promptly if bumping increases, side vision feels worse, or daily movement suddenly becomes harder. Seek urgent care for sudden vision loss, severe eye pain, new weakness, confusion, facial drooping, or trouble speaking.
Simple rule: if the change is sudden, severe, or neurologic, do not troubleshoot the hallway first.
Start Here: Why Door Frames Become Invisible With Glaucoma Field Loss
Door frames are sneaky because they are not usually what you are looking at. You look through the doorway toward the bedroom, bathroom, kitchen, or phone ringing in the next room. The frame is only a border.
But with glaucoma field loss, borders may be exactly where the trouble begins. If the larger pattern feels new, it may help to compare doorway bumps with other senior vision changes warning signs so the home fix does not accidentally replace needed care.
Peripheral Vision Loss Changes the “Edges” of a Room
Central vision helps you read a label, see a face, or spot the mug on the counter. Peripheral vision helps you sense the wider room: the wall edge, the cabinet corner, the dog drifting in from the left like a furry footnote.
When side vision is reduced, you may still see the doorway opening clearly. Yet the frame, threshold, or nearby object may not register early enough for your body to adjust.
The Doorway Problem: Your Center Vision Sees the Opening, Not the Frame
Most people do not walk through a doorway by staring at the frame. They aim for the open space. That works beautifully until the margin of safety shrinks.
Imagine the brain saying, “Opening detected. Proceed.” Meanwhile, the shoulder says, “Excuse me, there was wood here.” It is a tiny committee failure, and the shoulder usually files the complaint.
Here’s What No One Tells You: Familiar Rooms Can Become Riskier Than New Ones
Familiar rooms invite autopilot. Autopilot is efficient, but it can be rude.
In a new building, people often slow down, scan, and move carefully. At home, they carry laundry, answer phones, turn quickly, and move by memory. That memory may be based on the visual field they used to have, not the visual field they have today.
Infographic: Why a Familiar Doorway Starts Catching Your Shoulder
Side information arrives late or not at all.
Frame and wall blend together.
The body turns before the eyes confirm the edge.
Shoulder, elbow, hip, or walker clips the frame.
Best first fix: increase contrast, improve approach lighting, and slow the turn at the worst doorway.
Who This Is For, and Who It Is Not For
This guide is for practical people who want fewer bruises, fewer surprises, and fewer “I swear that doorway moved” moments.
It is especially useful when glaucoma field loss is already diagnosed or suspected, and the problem is happening in daily movement at home.
This Is For People Who Still Walk Independently but Keep Clipping Doorways
You may still cook, shower, take out the trash, and answer the door. You may still be very capable. That does not make the bumps imaginary.
One older reader once described it this way: “I see the room. I just don’t see the attack corners.” That phrase stuck with me because it is exactly how a home can feel when edges become unreliable.
This Is For Caregivers Who Hear “I’m Fine” After Another Shoulder Bump
Caregivers often notice the pattern before the person experiencing it wants to name it. That can create tension.
The goal is not to win an argument. The goal is to make the safer path easier than the risky path. Good home safety has the manners of a thoughtful host: present, useful, and not shouting from every wall. For families unsure how to step in, a guide to offering help to someone with low vision can make the conversation feel less like criticism and more like teamwork.
Not For Emergencies: Sudden Vision Loss, Eye Pain, or New Neurologic Symptoms Need Care
This guide is not for sudden symptoms. If vision changes quickly, if severe eye pain appears, or if new weakness, confusion, speech trouble, or facial drooping occurs, seek urgent medical help.
- Use home fixes for repeated patterns.
- Use eye care for new or worsening vision issues.
- Use urgent care for sudden, severe, or neurologic symptoms.
Apply in 60 seconds: Decide whether your problem is repeated and familiar, or new and rapidly changing.
The First Fix: Map Where the Bumps Actually Happen
Before buying tape, lamps, grab bars, smart bulbs, or a heroic little basket labeled “safety,” do one boring thing.
Map the bumps.
Boring often wins because it refuses to be theatrical. It simply tells the truth.
Track the “Collision Corners” for 7 Days
For one week, write down each collision or near-collision. Include the doorway, side of body, time, lighting, and what was happening.
You are looking for patterns like:
- Right shoulder hits bathroom door frame at night.
- Left hip clips kitchen entry while carrying dishes.
- Walker catches hallway trim during tight turns.
- Cabinet edge disappears when morning sun creates glare.
Separate Door-Frame Bumps From Balance, Dizziness, or Footing Problems
Not every collision is only visual. Doorway bumps can involve field loss, poor lighting, medication side effects, dizziness, foot pain, neuropathy, loose rugs, rushing, or turning mechanics.
This matters because the solution changes. If the person is dizzy, contrast tape is not enough. If the frame is invisible in dim light, balance exercises alone will not fix the doorway. When home movement, aging vision, and fall risk begin overlapping, use a broader aging vision fall prevention at home checklist to avoid fixing only the prettiest part of the problem.
The Tiny Notebook Test: Time, Doorway, Lighting, Direction, Speed
Use five quick notes:
- Time: morning, afternoon, evening, night.
- Doorway: bathroom, bedroom, kitchen, hallway, garage.
- Lighting: dim, glare, shadow, backlit, uneven.
- Direction: entering, exiting, turning left, turning right.
- Speed: normal, rushed, carrying something, half-awake.
Money Block: Eligibility Checklist
Use this checklist before spending money on home safety products.
- Yes or no: Have bumps happened more than once in the same doorway?
- Yes or no: Is one side of the body hit more often?
- Yes or no: Does the problem worsen at night, in glare, or while turning?
- Yes or no: Has an eye doctor already evaluated recent vision changes?
Neutral action: If you answered yes to the first three, start with one doorway test before changing the whole house.
Show me the nerdy details
Collision mapping works because it turns a vague complaint into a small behavioral dataset. The useful variables are not fancy: location, lighting, direction, speed, and body side. If the right shoulder repeatedly hits a bathroom frame during left turns at night, the fix is likely different from a kitchen doorway that disappears under daytime glare.
Make Door Frames Visible: Contrast Beats Decoration
Pretty trim is not the goal. Detectable trim is the goal.
For glaucoma field loss, the best visual cue is often simple: a high-contrast, matte marker placed where the body actually needs the warning.
Add High-Contrast Tape Where the Shoulder Actually Hits
Start at shoulder height, because that is often where the collision happens. Add a strip of high-contrast tape or a contrasting edge marker on the problem side of the doorway.
White wall with white trim? Try dark tape. Dark frame on dark wall? Try light tape. The point is not matching the curtains. The point is making the frame announce itself before your shoulder reads the memo.
Mark the Latch Side, Not Just the Pretty Trim
Many people mark the most visible part of the doorway rather than the most useful part. That is understandable, and also how homes end up with decorative safety confetti.
Mark the side where the person clips the frame. If the latch side catches the shoulder, mark that side. If the hinge side is the problem during tight turns, mark that side.
Use Matte Finishes to Avoid Glare Traps
Glossy tape can shine under lamps or daylight. That shine may create glare, which can be especially frustrating for people with low vision.
Choose matte, non-reflective material when possible. In many homes, a $6 roll of tape placed well beats a $60 gadget placed vaguely. If you are also repainting trim or walls, the same principle applies to matte vs glossy paint: the less glare a surface throws back, the easier it may be for edges to behave.
Don’t Do This: Random Strips Everywhere Can Create Visual Noise
More markings are not always better. Too many strips can turn a hallway into a barcode with opinions.
Use contrast like punctuation. A few clear marks guide attention. Too many marks compete for it.
- Start with one problem doorway.
- Place the cue at shoulder height or walker-contact height.
- Use matte contrast to reduce glare.
Apply in 60 seconds: Stand at the doorway you hit most and point to the exact place your body meets the frame.
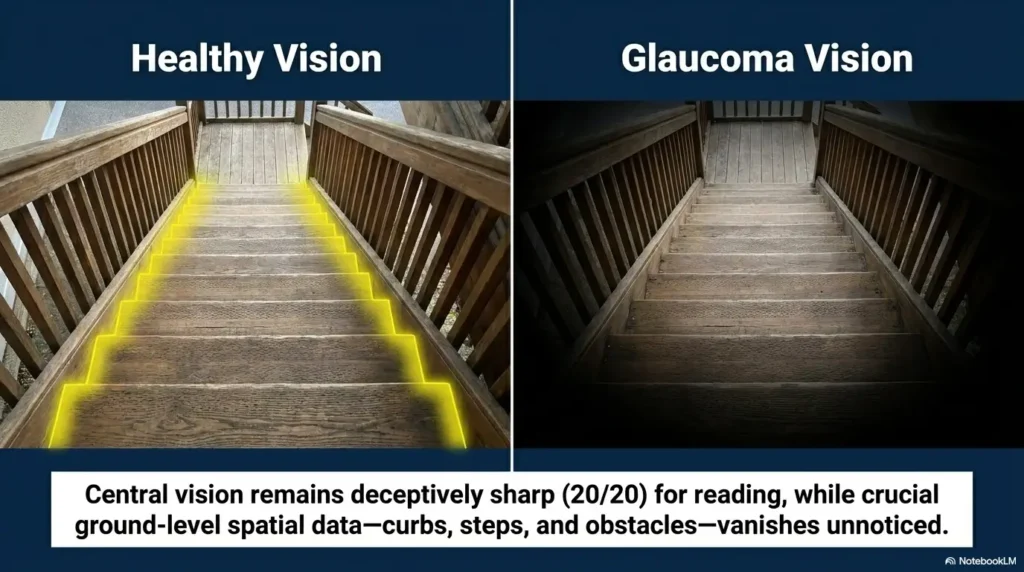
Lighting Changes That Stop the Hallway From Lying
Bad lighting does not merely make a room darker. It edits the room.
It erases edges, exaggerates shadows, and turns a door frame into a rumor. For glaucoma field loss, the lighting before the doorway often matters as much as the lighting inside the room.
Put Light Before the Doorway, Not Only Inside the Room
If a hallway is dim and the bathroom is bright, the doorway may become a high-contrast hole with a poorly defined edge. Place light along the approach path so the frame is visible before the person reaches it.
Motion-sensor plug-in lights can help in hallways, bedrooms, and bathroom routes. The best ones are not dramatic. They simply appear before the shin negotiates with furniture. If the first light you try feels harsh, a guide to what to do when a motion sensor light is too bright can help you keep the automation without turning the hallway into a tiny airport runway.
Reduce Backlighting That Turns Frames Into Shadows
Backlighting happens when bright light comes from behind or beyond the doorway. The frame may become a dark shape against a bright room, or disappear into glare.
Try adjusting blinds, moving lamps, or adding softer side lighting. Your aim is even light, not interrogation-room brightness.
Night Path Lighting: Bedroom to Bathroom Is the High-Risk Route
The bedroom-to-bathroom path deserves special treatment because it combines low light, sleepiness, urgency, and sometimes medication effects.
Use low, steady night lights along the route. Avoid cords across walking paths. If a light must be switched on manually, place the switch or remote where it can be reached before standing. For the color question, red vs amber night light choices may matter more than people expect, especially when the goal is orientation without glare.
Let’s Be Honest: “Just Turn On the Light” Is Not a Real System
People forget. People wake up groggy. People rush. People also say, “I was only going two steps,” which is how many household injuries introduce themselves.
A real system makes the safe action automatic. Motion lights, predictable switches, and clear paths beat noble intentions before coffee.
Money Block: Mini Doorway Priority Calculator
Score each problem doorway from 0 to 2 in three areas.
- Frequency: 0 never, 1 sometimes, 2 weekly or more.
- Lighting trouble: 0 clear, 1 dim or shadowed, 2 glare or night route.
- Consequence: 0 harmless brush, 1 bruise or near-fall, 2 fall or fear of falling.
Output: A score of 4 to 6 means fix that doorway first.
Neutral action: Pick the highest-scoring doorway and test one lighting change for 7 days.
Build a Doorway Routine: Slow the Turn, Find the Edge, Then Enter
Home safety is not only objects. It is choreography.
A doorway routine gives the body a repeatable sequence: slow, locate, align, enter. It sounds too simple until you realize most collisions happen when one of those steps gets skipped.
Pause One Beat Before Narrow Doorways
Pause before tight doorways, especially bathrooms, closets, laundry rooms, and garage entries. One beat is enough.
The pause does two useful things. It lets the eyes confirm the edge, and it lets the feet stop dragging the rest of the body through a guess.
Use a Gentle Hand Trail on the Safe Side
Some people benefit from lightly trailing a hand along the wall or frame on the safer side. This is not grabbing. It is information gathering.
Think of it as letting the hand read the room’s margin. A wall can be a quiet guide when vision is busy doing harder work. For outdoor routes, appointments, and crowded buildings, sighted guide assistance may also be worth learning so help feels clear, respectful, and physically safer.
Turn With Your Feet, Not Just Your Head
Doorway collisions often happen during turns. The head turns toward the destination, but the feet keep the body angled toward the frame.
Practice turning in small steps with the feet, then entering. This is especially important for people using walkers, canes, or carrying laundry. Laundry baskets are notorious for stealing peripheral information and dignity at the same time. A broader set of low vision walking guidance can help connect doorway habits with the way someone moves through longer routes.
The “Shoulder First” Mistake That Makes Frames Win
Many people lead through a doorway with the shoulder when rushing. That narrows the margin and makes the frame more likely to win.
Instead, square up before entering. Nose, chest, and feet should agree on where the doorway is. A house becomes safer when the body stops entering rooms like a distracted shopping cart.
- Pause one beat.
- Find the edge visually or by gentle touch.
- Turn with feet before entering.
Apply in 60 seconds: Practice one slow doorway pass right now without carrying anything.
Clear the Approach Zone: Doorway Safety Starts Three Feet Earlier
A doorway collision rarely begins at the doorway. It begins three feet earlier, where the approach gets messy.
Shoes, mats, baskets, pet bowls, small tables, umbrella stands, and decorative objects can pull attention away from the frame. The doorway becomes the final act of a play that started with clutter.
Remove Shoes, Baskets, Mats, and Small Furniture Near Frames
Clear at least three feet on both sides of the problem doorway when possible. This gives the body time to align before entering.
Do not underestimate small objects. A pair of shoes near a frame can change foot placement just enough to send a shoulder into the trim. Shoes have no shame. They just sit there, smug and trip-shaped.
Keep Doors Fully Open or Fully Closed
Half-open doors are visual traps. They create new edges, unexpected shadows, and narrow angles.
For frequently used routes, keep doors fully open or fully closed. If a door must stay open, use a stopper so it does not drift into the walking path.
Use Contrasting Thresholds Only If They Do Not Create Trip Hazards
A contrasting threshold can help define room changes, but avoid raised strips or loose materials that increase trip risk.
Flat, secure, matte contrast is safer than anything thick, curled, slippery, or dramatic. The floor should not become a tiny obstacle course in the name of safety.
Don’t Do This: A Beautiful Rug at the Door Can Become a Sneaky Fall Tax
Rugs near doorways often look cozy and behave badly. They curl, slide, bunch, and hide edges.
If a rug is necessary, use a low-profile, non-slip option and check the edges regularly. If it moves underfoot, it is not decor. It is paperwork for gravity.
Money Block: Decision Card
- The frame blends into the wall.
- Bumps happen at the same shoulder height.
- Lighting is already fairly even.
- Objects collect near the doorway.
- Turns feel tight or rushed.
- A walker, cane, or basket catches the edge.
Neutral action: If both are true, clear the approach today and add contrast tomorrow.
Room-by-Room Fixes for Glaucoma Field Loss at Home
Every room has its own little personality. The bedroom is sleepy. The bathroom is slippery. The kitchen has corners with ambitions.
Do not fix every room the same way. Match the solution to the task, the lighting, and the collision pattern.
Bedroom: Mark the Door Edge and Keep the Night Path Predictable
The bedroom needs predictability. Keep the path from bed to door consistent. Avoid moving chairs, laundry baskets, slippers, or charging cables into the walking route.
Place a night light so the doorway edge appears before standing or within the first few steps. If the same shoulder hits the same frame in the morning, add a matte contrast cue at that height. A stable low vision bedside organization system can also keep glasses, phone, water, and eye drops from migrating into the walking path.
Bathroom: Add Contrast Near Entry, Toilet, Shower, and Towel Reach Zones
The bathroom deserves extra caution because wet surfaces and urgency make small errors more expensive.
Use contrast near the entry frame, toilet area, shower edge, and towel reach zone. Avoid loose mats. If grab bars are needed, discuss proper placement and installation with a qualified professional. A towel bar is not a grab bar, even if it has been lying about its strength for years.
For bathroom-specific details, pair doorway contrast with practical fixes such as toilet seat contrast color, anti-slip shower strips placement, and tactile faucet marking, especially when glare, wet floors, and half-awake bathroom trips all arrive together.
Kitchen: Protect Corners, Cabinet Edges, and Appliance Doors
Kitchens create moving hazards: open cabinets, dishwasher doors, refrigerator doors, sharp corners, and counters that blend into floors or walls.
Keep frequently used cabinet doors fully closed. Add contrast to cabinet edges if they disappear. If the person often clips the kitchen entry while carrying plates, reduce the carry load or create a landing zone near the doorway.
Hallways: Give the Wall a Visual Rhythm, Not a Maze
Hallways need rhythm. A few predictable contrast points can help orientation. Too many decorations can create visual clutter.
Use clear wall edges, stable lighting, and a simple approach path. If frames, walls, and floors are all similar in color, the hallway may need contrast more than it needs another framed print of a boat looking emotionally complicated.
Short Story: The Bathroom Door That Kept Winning
A caregiver once told me her father kept hitting the same bathroom door frame but insisted nothing was wrong. They argued for two weeks, which helped no one except the doorway, which continued its undefeated season. Finally, they taped a small piece of dark matte contrast at shoulder height, moved a laundry basket away from the approach, and added a night light before the bathroom entry instead of inside the bathroom only.
The fix looked almost too humble. No renovation. No lecture. No dramatic family meeting around a screwdriver. But the next week, the bumping dropped enough that her father admitted, with great reluctance and excellent dignity, “That little strip is not terrible.” Sometimes independence is preserved by changes small enough that pride can walk around them.
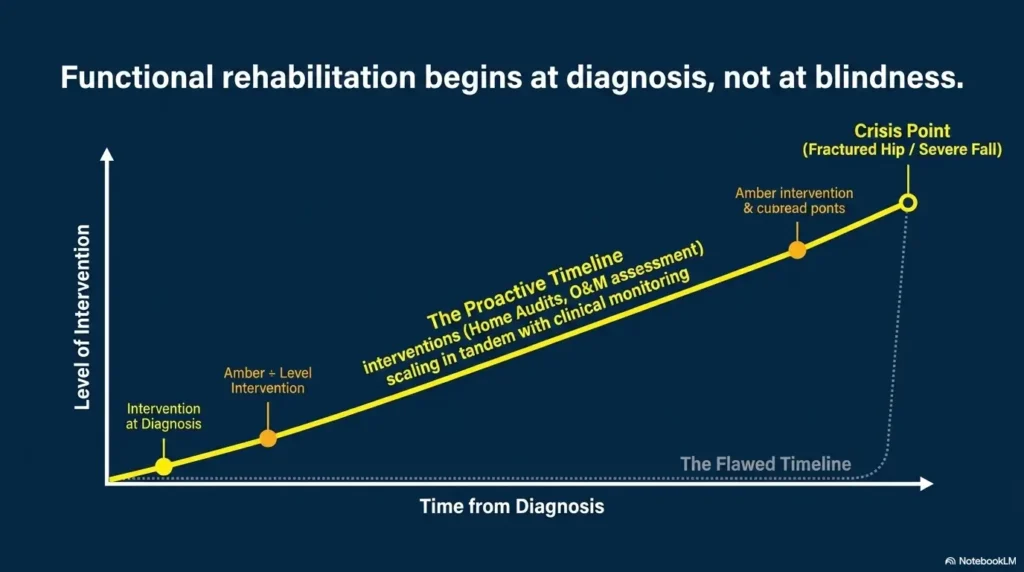
Low-Vision Rehabilitation: The Professional Help Many People Meet Too Late
Low-vision rehabilitation is not admitting defeat. It is learning how to use remaining vision, tools, lighting, contrast, scanning, and movement strategies more effectively.
The National Eye Institute describes vision rehabilitation as services that help people with visual impairment manage daily life and maintain independence. That is exactly the territory we are in: not just seeing an eye chart, but moving through a real home with real corners.
What a Low-Vision Therapist Can Help You Practice
A low-vision therapist may help with lighting, contrast, task setup, scanning habits, reading aids, glare control, and daily routines.
For door-frame collisions, therapy may focus on how to locate edges, move through narrow spaces, organize rooms, and reduce visual confusion. This can be especially helpful when the person still has good central vision and wonders why the house suddenly feels rude.
When Orientation and Mobility Training Makes Sense
Orientation and mobility training can help people with visual impairment move more safely and confidently. It may include scanning, route planning, cane skills when appropriate, and travel strategies inside or outside the home.
This does not mean everyone needs a cane. It means movement deserves training when vision changes daily navigation.
Why “I Know My Own House” Is Not Always Enough
Knowing the house helps. It also tempts the brain to run old software.
If glaucoma field loss changes what the eyes detect, the body may need updated habits. Familiarity can reduce anxiety, but it can also hide risk because nobody expects the hallway they have walked for 20 years to become a problem.
- Ask about lighting and contrast strategies.
- Ask about scanning and doorway movement habits.
- Ask whether orientation and mobility training fits your situation.
Apply in 60 seconds: Write one sentence for your eye doctor: “I keep bumping into door frames at home and want help with low-vision safety.”
Common Mistakes That Keep Door-Frame Bumps Happening
Most home safety mistakes come from good intentions moving too quickly.
The family wants to help. The person wants independence. Everyone buys something. The doorway remains undefeated. Let’s not feed the doorway.
Blaming Age Instead of Measuring the Pattern
Age may be part of the story, but it is too vague to be useful. “Getting older” does not tell you whether the bathroom light is behind the person, whether the right shoulder hits during turns, or whether the rug edge moved again.
Patterns give you levers. Labels do not.
Fixing the Whole House Before Fixing the Worst Doorway
Trying to fix the entire house in one weekend can exhaust everyone and create resistance.
Start with the worst doorway. Test one change. Watch for one week. Then adjust. This is not slow. This is precision wearing comfortable shoes.
Adding More Light Without Reducing Glare
More light can help, but glare can make vision worse. A bright bulb pointed at a shiny floor may create more confusion, not less.
Aim for even, soft, well-placed light. The best lighting is not the brightest lighting. It is the lighting that makes edges honest. In bathrooms and kitchens, surfaces can be especially treacherous, so problems like white tile floor glare deserve attention before adding stronger bulbs.
Assuming a New Glasses Prescription Solves Field Loss
Glasses can correct refractive problems, but they do not restore glaucoma-related visual field loss. A current prescription is still important, but it may not solve doorway collisions by itself.
This is why medical follow-up, low-vision strategies, and home design need to sit at the same table.
Waiting Until a Fall Before Asking for Mobility Help
A near-fall is already useful information. So is fear of falling. So is avoiding a doorway, shower, hallway, or room because it feels risky.
Do not wait for the dramatic event. Prevention works best before the floor gets involved.
Show me the nerdy details
Many doorway fixes fail because they target the object instead of the interaction. The relevant interaction includes visual field, contrast sensitivity, glare, walking speed, turn angle, balance, footwear, medication effects, and whether the person is carrying something. A useful fix changes at least one of those variables in a measurable way.
Money Block: Quote-Prep List
If you compare help from an occupational therapist, low-vision clinic, handyman, or home safety service, gather this first.
- Photos of the three worst doorways in daytime and nighttime light.
- A 7-day bump log with time, direction, and body side.
- A list of current mobility aids, glasses, eye drops, and recent falls or near-falls.
- Measurements of doorway width and the approach space.
- Notes on rugs, thresholds, stairs, pets, and night bathroom trips.
Neutral action: Put these details in one folder before calling anyone for estimates or appointments.
When to Seek Help: The Red Flags Worth Taking Seriously
Some bumps are home-design problems. Some are medical signals. The difficult part is not pretending you can always tell the difference from the hallway.
When symptoms change, get help sooner rather than later.
Call an Eye Doctor Promptly for Noticeably Worse Side Vision
Contact an eye doctor if side vision feels worse, blind spots seem larger, collisions increase, or daily activities become harder.
Also call if eye drops are hard to manage, doses are missed, or side effects make routines difficult. Glaucoma care depends partly on treatment consistency, and real life has a talent for eating routines. If medication routines are part of the problem, a practical low vision medication management setup can reduce missed doses and search-time chaos.
Seek Urgent Care for Sudden Vision Loss, Severe Eye Pain, New Weakness, or Confusion
Sudden vision loss, severe eye pain, headache with vision symptoms, new weakness, confusion, trouble speaking, or facial drooping should be treated as urgent.
Do not spend the afternoon testing tape placement if the symptom arrived like a slammed door.
Talk to a Clinician After Falls, Near-Falls, or New Unsteadiness
A fall or near-fall deserves a conversation with a clinician. So does new unsteadiness, dizziness, faintness, or fear of walking through parts of the home.
The CDC’s fall-prevention materials emphasize screening and reducing fall risk in older adults. Vision impairment is one important piece of that risk picture.
Ask About Fall Risk Screening if Vision Loss Is Changing Daily Movement
If glaucoma field loss is changing how someone moves, ask about fall risk screening. This may involve reviewing medications, strength, balance, footwear, home hazards, and vision care.
Good fall prevention is not one magic device. It is a stack of small protections, each one catching what the others miss.
Caregiver Script: How to Help Without Turning the House Into a Warning Label
Caregiving around vision loss is delicate because safety and dignity share the same hallway.
Too little help leaves risk untouched. Too much help can feel like a home invasion conducted with label makers.
Ask “Where Did the Bump Happen?” Instead of “Are You Okay?”
“Are you okay?” often gets one answer: “I’m fine.” It closes the conversation.
Try: “Where did it happen?” or “Was it the right shoulder again?” These questions are less dramatic and more useful. They turn the event into shared problem-solving, not a courtroom scene with a bruise as Exhibit A.
Offer One Fix Per Week, Not a Full Home Takeover
One fix per week protects cooperation. It also helps you learn what actually works.
Try this sequence: first clear the approach, then add contrast, then adjust lighting, then practice the routine. A gentle pace often gets more done than a heroic Saturday that leaves everyone silently furious near a roll of tape.
Photograph Doorways Before and After Changes
Photos help caregivers notice whether changes are visible, clutter has returned, or glare is worse at certain times of day.
Take photos from the person’s usual approach angle, not from the prettiest real-estate angle. The house is not trying to sell itself. It is trying to stop ambushing a shoulder.
Protect Independence by Making the Safer Path the Easier Path
The best caregiver fix does not require constant reminders. It makes the safer behavior natural.
Put the light where it turns on automatically. Put the contrast cue where the body needs it. Move clutter so the route feels obvious. Independence grows when safety stops requiring a speech.
- Ask location-based questions.
- Make one change at a time.
- Let the safer route become the easiest route.
Apply in 60 seconds: Replace “Be careful” with “Which doorway has been most annoying this week?”
FAQ
Why do I keep hitting door frames with glaucoma?
Glaucoma can reduce side vision or create blind spots, so the center of the doorway may look clear while the frame edge is detected too late. Poor lighting, glare, clutter, speed, and turning can make the problem worse.
Can glaucoma cause trouble judging doorways?
Yes. Some people with glaucoma have trouble noticing edges, obstacles, or movement outside central vision. Doorways are especially tricky because people usually look through them, not directly at the frame.
Does bumping into walls mean my glaucoma is getting worse?
Not always, but it is worth taking seriously. Repeated or worsening collisions can signal changes in vision, lighting problems, balance issues, medication effects, or home hazards. If the pattern is new or increasing, contact your eye doctor.
What home changes help with peripheral vision loss?
Useful changes often include high-contrast door-frame markers, matte finishes, better approach lighting, reduced glare, cleared walking paths, stable rugs or no rugs, predictable furniture placement, and practiced doorway routines.
Should I use contrast tape on door frames?
Contrast tape can help when the frame blends into the wall. Place it where the collision happens, often at shoulder height or walker-contact height. Use matte tape and avoid covering every edge in the home, which can create visual clutter.
Can low-vision therapy help if I still have central vision?
Yes. Low-vision rehabilitation is not only for people with severe central vision loss. It can help with daily tasks, scanning habits, lighting, contrast, glare control, and movement strategies when field loss affects function.
Is bumping into door frames a fall risk?
It can be. A shoulder bump may seem minor, but the same visual, lighting, or movement problem could also contribute to a trip, stumble, or fall. This is especially important for older adults, people using mobility aids, and anyone with dizziness or balance changes.
When should I call my eye doctor about new collisions?
Call promptly if collisions increase, side vision feels worse, blind spots seem larger, or daily movement becomes harder. Seek urgent care for sudden vision loss, severe eye pain, new weakness, confusion, or speech trouble.
Next Step: Fix One Doorway Before You Fix the Whole House
Remember the hook: that small, insulting thud of shoulder against trim. The answer is not to fear the whole house.
The answer is to make one doorway tell the truth.
Choose the Doorway You Hit Most Often
Pick one doorway. Not five. Not the entire hallway kingdom. One.
Choose the doorway with the highest score: frequent bumps, poor lighting, glare, nighttime use, or a near-fall. Bathrooms and bedroom routes often deserve first attention, especially when the same path repeats after dark. For a deeper bathroom-route setup, use low vision nighttime bathroom safety ideas alongside the doorway changes here.
Add Contrast at Shoulder Height and Improve the Approach Lighting
Place matte contrast where the body actually clips the frame. Then improve the light before the doorway, not only inside the room.
If clutter sits within three feet of the frame, remove it. If a rug curls near the threshold, secure it or take it away. If a door floats half-open, make it fully open or fully closed.
Test It for One Week, Then Adjust
Live with the change for 7 days. Track bumps and near-bumps. Ask whether the doorway feels easier, not whether it looks perfect.
If the bumping improves, keep the change and consider the next doorway. If not, adjust placement, lighting, or approach routine. Safety is often a small experiment, not a grand announcement.
The 60-Second Action: Mark One Frame, Clear Three Feet, Slow One Turn
Here is the entire plan in one minute:
- Mark the problem edge with matte contrast.
- Clear three feet before and after the doorway.
- Add or adjust approach lighting.
- Practice one slow pause-turn-enter routine.
- Write down whether the next week feels safer.
Final CTA: Within the next 15 minutes, choose the one doorway that has been quietly collecting bruises, clear its approach, and place one temporary contrast cue at the exact height where the collision happens. Do not remodel the whole house today. Teach one doorway some manners first.
Last reviewed: 2026-05.

